When William Osler arrived at The Johns Hopkins Hospital to serve as its first physician-in-chief in 1888, he would quickly become revered for his bedside teaching and mantra to “care more particularly for the individual patient than for special features of the disease.” His legacy endures in today’s Osler Medical Residency program — considered a model for medical training worldwide.
Less known, perhaps, is that Osler recognized that long hours, medical complexities and self-doubt exact an emotional toll. ”The best preparation for today is to live superbly well,” he advised residents, urging them to “read a good story, see a play and not to take oneself too seriously.”
More than a century later, managing burnout, family obligations and other challenges are top concerns among directors of medical residency programs nationwide. Mindfulness, meditation and psychiatric resources are now widely available to residents at many internal medicine training programs, including the Johns Hopkins program.
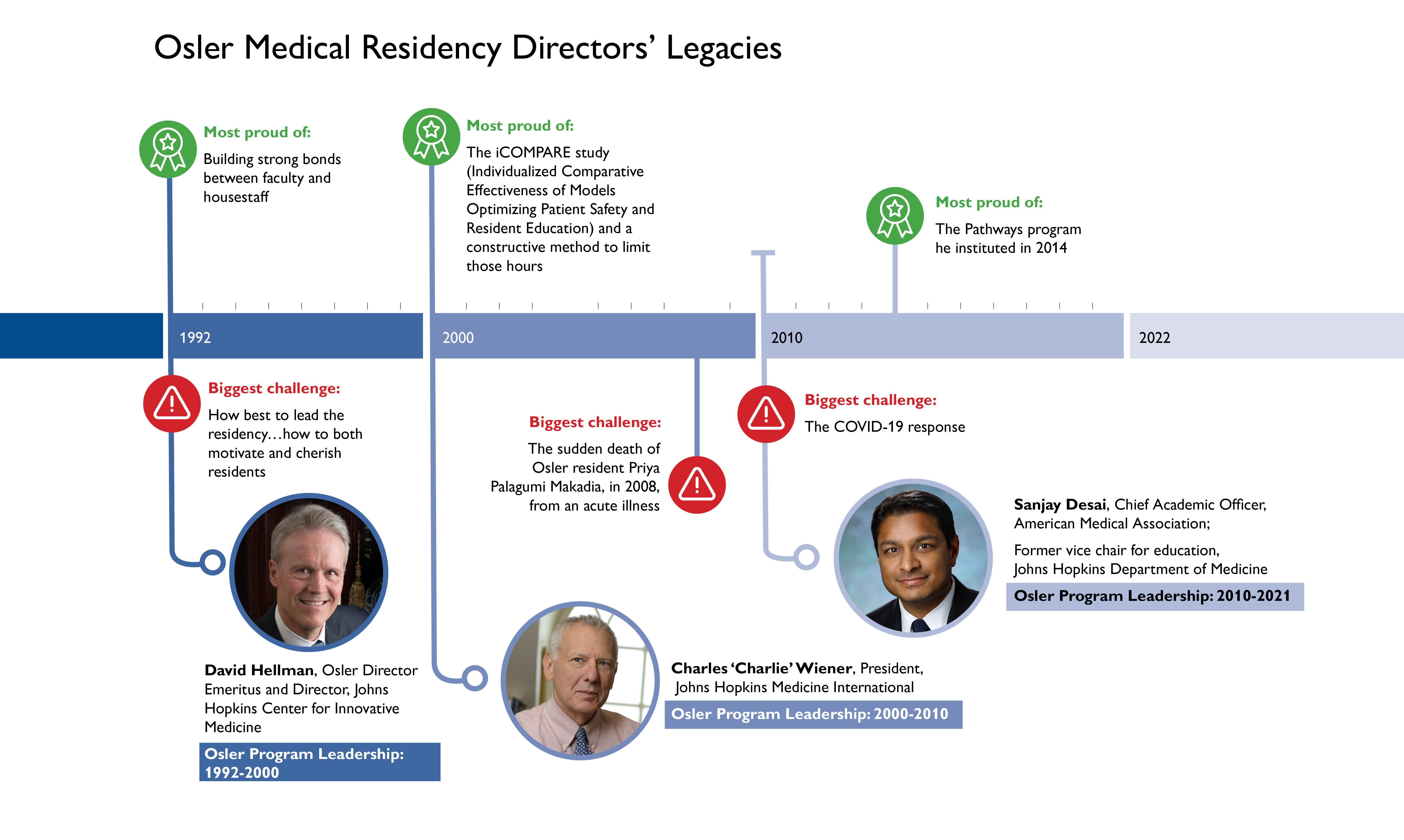
We contacted three Osler Medical Residency directors who led the program during three different decades and asked them to describe their greatest challenges and accomplishments, how those experiences have evoked pride and how they are reflected in the program today.
David Hellmann
Osler Director Emeritus and Director, Johns Hopkins Center for Innovative Medicine
Osler Program Leadership: 1992–2000
After David Hellmann (Thayer, 1980) completed his training at Johns Hopkins as a medical student and internal medicine resident, he had a rheumatology fellowship at the University of California, San Francisco. But he so missed the challenging and collaborative environment at Johns Hopkins that he returned in 1986, ultimately accepting the position as first executive vice chairman of the Department of Medicine, and becoming the inaugural director of the Osler Medical Residency program.
Hellmann and the then Osler professor of medicine, John Stobo, thought the training program was at its best “when it both inspires and cherishes its residents,” says Hellmann. In 1987, to pursue both goals, Hellmann and Stobo worked with Thomas Traill and others to create the Firm faculty system. Outstanding faculty members with diverse clinical and research interests were assigned to each Firm, allowing them and residents to know one another better as colleagues and as people, and to learn from one another.
“Hopkins,” Hellmann says, “is one of the few places in the country that allows people access to the Mount Everest of the medical profession. Climbing Mount Everest is incredibly challenging. Our program is at its best when it not only points to the peak of Mount Everest, but also provides Sherpas [expert navigators], who ensure that everyone is well equipped, safe, and successful in reaching the peak. We don’t have to choose between inspiring or treasuring our residents. We can and must do both.”
Charles Wiener
President, Johns Hopkins Medicine International
Osler Program Leadership: 2000–2010
From the outset of his tenure as director of the Osler residency, Charlie Wiener made it clear to his residents that he was “accessible to them 24/7.” It was a position he says he relished, and helping trainees deal with struggles and witnessing their success was something he says he’ll never forget.
“To see the impact the program has had on them was the pinnacle of my career,” Wiener says. “It’s like having almost 500 children who are impacting the world in the most amazing ways.” But he acknowledges inherent challenges that came with the job. “Micromanaging the residency work hours was especially intense,” he recalls. “The Accreditation Council for Graduate Medical Education wanted to proscribe in great detail how duty hour limits would be applied, and some were difficult to accommodate within the Osler model. Eventually, the iCOMPARE study [Individualized Comparative Effectiveness of Models Optimizing Patient Safety and Resident Education, led by Sanjay Desai] imposed academic rigor to designing the residency experience within the guardrails of work hours, and gave programs the flexibility to develop schedules specific to their learning objectives.”
Wiener says his greatest challenge, however, was the sudden death of Osler resident Priya Palagummi Makadia, in 2008, from an acute illness. “Seeing one our most treasured colleagues pass away so quickly was one of the most jarring moments of my career,” Wiener says. “Her sudden loss shook us all to the core. The experience reminded many of us about the importance of our colleagues and family.”
Osler residency directors, he says, “have fostered a huge amount of loyalty to the residency, and there are many ways to do the job. The key is to stand up for the core values of the Osler program for the patients and the residents: accountability and love of medicine.”
Sanjay Desai
Chief Academic Officer, American Medical Association;
Former Vice Chair for Education, Johns Hopkins Department of Medicine
Osler Program Leadership: 2010–2021
For Sanjay Desai (Janeway, 2005), the Pathways program he instituted in 2014 was “probably the most important innovation” during his term. Pathways nurtures dedicated career development for second- and third-year residents in one of four areas for each resident: patient safety and quality improvement, global health, medical education and scientific discovery. These trainees are offered a “pathway” to apply individualized coursework, hands-on experiences and sophisticated mentorship to their chosen field of interest, culminating with a research project with a mentor.
“It embedded formal, rigorous training in these additional sciences into the residency experience,” says Desai. “We wanted to bring the world’s expertise that we are fortunate to have across our university directly to our residents — feasibly and effectively — to develop them into leaders.”
He also notes that spearheading the national iCOMPARE study and participating in work regarding the American Medical Association’s Reimagining Residency grant to address burnout were major accomplishments, using data to inform residency training.
Desai’s greatest challenge during his career was something unexpected and unprecedented: the COVID-19 response. “It was a sobering realization that we were on the front lines in the greatest crisis in modern history,” he says.
At the same time, he adds, “Treating patients during the pandemic has been one of our greatest triumphs. What the Osler residents and their colleagues have done throughout the hospital — and, indeed, throughout the country — will be talked about for generations. We will never forget the dedication and sacrifice by everyone to care for our patients, communities and families.” Desai was reminded during this time how the Firm system, with its assistant chiefs of service, is “a unique model in the country, is capable of preserving the training and well-being of our residents through any circumstance,” he says. “The Osler program remains proud of its traditions, and is never encumbered by them. The tradition of pursuing excellence will always prevail.”
In every generation, the Osler residency will no doubt evolve, as expected and unexpected scenarios arise. And each new director will draw from predecessors’ experiences to impart knowledge, respond to challenges, strengthen bonds with residents and inspire pride in distinct ways. In the words of Sir William Osler, “To have striven, to have made an effort, to have been true to certain ideals — this alone is worth the struggle.”
Learn about Natasha Chida, the new director of the Osler Medical Residency, and read a message from Mark Anderson, director of the Johns Hopkins Department of Medicine.


