Lifeline: About Us

Johns Hopkins Lifeline provides all types of patient transportation with a specialty in critical care. This hospital based program, among the first-of-its-kind in the region, it was primarily designed to provide advanced life support and critical care services for patients referred to Johns Hopkins Health System hospitals and transferred from other hospitals. In an effort to expedite and streamline patient flow into and throughout member hospitals, an integrated delivery system was developed to meet the demands for all types of transportation. Approximately 40,000 transports are coordinated annually through the Hopkins Communications Center. Contractual agreements, which support the various types of transportation demands (ground, rotor wing and fixed wing) have been instrumental to the success of the program.
-
In early 1992, Mr. James Scheulen, Administrator of the Department of Emergency Medicine, first initiated the idea of a patient transportation system based at The Johns Hopkins Hospital. His vision was to provide for a safe, efficient and rapid transportation system for critically ill and injured patients being referred to the Hospital System. The Johns Hopkins Advanced Life Support Transport Team transported its first patient in July of 1992. In the teams first year of service, a single ambulance was utilized for an average of 3.5 calls per day.
Initially operating through a contractual relationship with Metropolitan Ambulance, the program began its assent into the world of critical care transport. We can provide transport by virtually any mode available under the umbrella of the Center for Transport Medicine. We have the capability to move patients all across the world, in an effort to bring them to the services offered at The Johns Hopkins Hospital. We are able to begin the care at the patients’ location, and continue that level of service throughout transport until delivery is made at the Johns Hopkins Hospital or one of its affiliates.
Lifeline also provides in-house patient transports at the main hospital campus. Our teams are responsible for moving patients from in-patient units for a procedure or test within the hospital that require continued specialized monitoring. This additional service provides a continuity of care for the patient while being moved within the institution.
The primary mission of Johns Hopkins Lifeline is to provide ground/air transport to critically ill and injured patients to the The Johns Hopkins Hospital and its affiliates. Our secondary mission is to transport patients and their families requiring less intensive monitoring and assistance. The addition of Yellow Transportation gives Lifeline access to a large fleet of cabs, sedans, Para transit vehicles and limousines.
-
Mission
The Johns Hopkins Lifeline Transportation Program is dedicated to delivering the highest level of quality care and safe, cost-effective and efficient patient transport with a commitment to professional excellence. Lifeline offers a collaborative approach to meeting the multidimensional needs of referring physicians and their patients.
Vision
The Johns Hopkins Lifeline transportation program vision is to provide an environment that promotes safe, efficient and appropriate medical transportation while achieving excellence in patient care, evidence-based research, and education.
Values
The Johns Hopkins Lifeline organization is committed to the following principles and values:
- Promoting safety awareness
- Upholding a commitment to professional and clinical excellence
- Providing timely service
- Expanding our leadership, educational and research role in the industry and community
- Creating a rewarding, enriching and challenging environment for our staff
- Maintaining continuity of care
- Exhibiting an interdisciplinary team focus
-
- Centralized communications center (24/7)
- Wheel chair van
- Ground ambulance service (basic life support, advanced life support, critical care transport)
- Rotor-wing program
- Fixed-wing program
- Specialty team transports
- Intrahospital critical care transport program
- Event medical standby units
- Community support/services
- Adult, pediatric and neonatal care
- International and domestic medical transports
By using a team of dedicated staff, the critical care and advanced life support divisions of Lifeline are among the most successful and recognizable transport teams in the state.
Lifeline is able to transport a diverse patient population, including patients of all ages in need of care for the following:
- Cardiac conditions
- High-risk pregnancies
- Severe burns
- Neurological emergencies
- Transplant medicine
- Trauma and other surgical needs
The program is active in the transportation of high risk patients requiring cardiopulmonary supportive adjuncts such as extracorporeal membrane oxygenation, intra-aortic bypass, cardiac assist devices, and intra-aortic balloon pumps, with the ability to transport patients who require nitric oxide therapy as a treatment modality.
The Lifeline of Johns Hopkins
One of the first of its kind in this region, The Johns Hopkins Lifeline Transportation program was designed to provide advanced life support and critical care services for patients referred to a Johns Hopkins Health system hospital.
Transport Services

As Lifeline grew, its transportation modes and contracts grew as well. In 2017, the HopComm team joined colleagues in the new Capacity Command Center to work as one team dedicated to patient transport, access, throughput and capacity management. Learn about our transportation services below.
-
 All transports that fall outside of the scope of practice of a Maryland EMT-Paramedic are termed Critical Care. Highly trained Critical Care Transport Nurses, are dispatched along with an advanced life support team to provide care during transport. Working within the guidelines of the Maryland Nurse Practice Act, Hopkins transport nurses provide advanced skills to their patients in a variety of transport settings. Our critical care units are equipped with the most advanced equipment available for our patients. In addition to this equipment, each unit is stocked with approximately 75 medicines for use by the Registered Nurse in the transport environment. This allows for the management of a wide variety of disease processes prior to the patients’ arrival to the Johns Hopkins Medical Campus’.
All transports that fall outside of the scope of practice of a Maryland EMT-Paramedic are termed Critical Care. Highly trained Critical Care Transport Nurses, are dispatched along with an advanced life support team to provide care during transport. Working within the guidelines of the Maryland Nurse Practice Act, Hopkins transport nurses provide advanced skills to their patients in a variety of transport settings. Our critical care units are equipped with the most advanced equipment available for our patients. In addition to this equipment, each unit is stocked with approximately 75 medicines for use by the Registered Nurse in the transport environment. This allows for the management of a wide variety of disease processes prior to the patients’ arrival to the Johns Hopkins Medical Campus’.Lifeline also facilitates specialty transports of pediatric patients. A nurse and a physician from the Pediatric Intensive Care Unit provide care for the patient during transport with the Lifeline Paramedic. The Maryland Regional Neonatal Transport Team is staffed by the Neonatal Intensive Care Unit and responds to all requests for neonatal transports.
Through a thorough and comprehensive training program, patients of all acuity levels can be transported safely and efficiently to The Johns Hopkins Hospital. On-line medical direction (Consultation with our Medical Director), is available for every call on a 24 hour, 7 day a week basis.
Our Critical Care Registered Nurses come to our program with a solid foundation of expertise from working in a critical care environment (ICU). They are expected to be credentialed as a CCRN (Critical Care Registered Nurse) within one year of employment.
All Nurses, Paramedics and EMT’s with the program attend mandatory continuing education on a regular basis to assure that they maintain an adequate knowledge base and display competency in performing skills and techniques which are required in their respective discipline.
Education and Certifications By Team Members
- Advanced Cardiac Life Support (ACLS)
- Advanced Burn Life Support (ABLS)
- Neonatal Advanced Life Support (NRP)
- Pediatric Advanced Life Support (PALS)
- Trauma Nursing Core Course (TNCC)
- Emergency Nurse Pediatric Course (ENPC)
- Basic and Advanced Trauma Life Support (ATLS)
- Critical Care Registered Nurse (CCRN)
- Certified Emergency Nurse (CEN)
- Certified Flight Registered Nurse (CFRN)
- Critical Transport Registered Nurse (CTRN)
- National and State Certified EMT-Paramedic
Equipment Carried or Available for Critical Care Transports
- Ventilator for each patient
- Three chamber IV pumps (3)
- Zoll Defribrillator with external pacer
- End-Tidal CO2 and Pulse Oximetry Monitoring Equipment
- Internal Pacemaker
- IABP ( Intra-Aortic Balloon Pump)
- Doppler
- Isolette
- Ventricular Assist Devices (VAD and BiVAD Devices)
- Intubation and Emergency Airway Equipment
- Medications
-
Paramedic and EMT-B level care transports
Johns Hopkins Lifeline has dedicated emergency medical technicians (EMTs) and paramedics to provide care for patients who require some level of medical monitoring. These personnel, who are employed by Lifestar Response, provide staffing for our ground basic life support (BLS) and advanced life support (ALS) ambulances. Medical direction is provided by a Johns Hopkins medical control physician and protocols set forth by the Maryland Institute for Emergency Medical Services Systems. Our paramedics and EMTs attend routine continuing education classes.

BLS ambulances are staffed by EMT caregivers and provide transports for patients who require basic medical monitoring for situations such as:
- Lower extremity fractures
- Discharges to home and sub-acute care facilities (nursing homes)
- Medical and surgical patients who do not require cardiac monitoring
- Psychiatric patients
ALS ambulances staffed by a paramedic, transport patients who require a higher level of medical monitoring. Patients who require ALS transport may include:
- Medical/surgical patient with continuous IV medicine.
- Patient on a cardiac monitor
- Patients moving to a higher level of care
- Patients on a chronic ventilator
-
Medevac 10
 Rotor-wing service is provided in collaboration with STAT MedEvac, an FAA-certified air carrier service and is staffed with a pilot, paramedic and Johns Hopkins Lifeline flight nurse.
Rotor-wing service is provided in collaboration with STAT MedEvac, an FAA-certified air carrier service and is staffed with a pilot, paramedic and Johns Hopkins Lifeline flight nurse.Request for a rotor-wing transport can be initiated through the Hopkins Access Line (HAL) at 1-800-765-JHHS (5447).
The Lifeline of Johns Hopkins | Providing Patient Care from the Sky
 In 2001, the Johns Hopkins Lifeline transportation team expanded its patient care capabilities to include rotor-wing, or helicopter, service through a collaboration with STAT MedEvac. This extended Lifeline’s reach, giving the team the ability to fly to pick up patients and provide Johns Hopkins’ level of care more quickly to patients from their bed side at other hospitals. In 2021, Lifeline celebrated 20 years of its helicopter division’s accomplishments, including more than 10,000 patient flights.
In 2001, the Johns Hopkins Lifeline transportation team expanded its patient care capabilities to include rotor-wing, or helicopter, service through a collaboration with STAT MedEvac. This extended Lifeline’s reach, giving the team the ability to fly to pick up patients and provide Johns Hopkins’ level of care more quickly to patients from their bed side at other hospitals. In 2021, Lifeline celebrated 20 years of its helicopter division’s accomplishments, including more than 10,000 patient flights. -
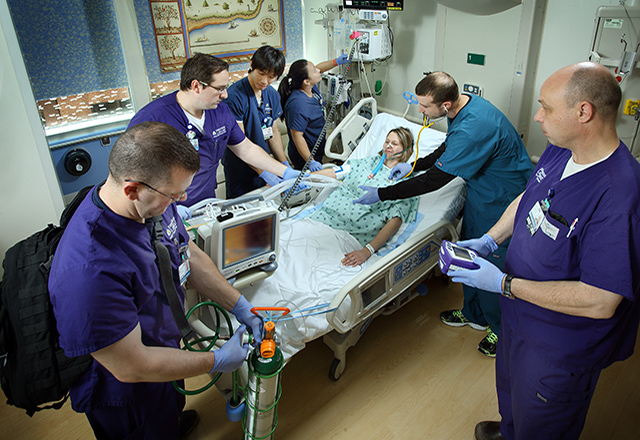
Unique to The Johns Hopkins Hospital, transportation of critically ill patients within the hospital has become a specialty of the Lifeline transport team. The intrahospital transport team applies their expertise in critical care transport to a setting inside the hospital, providing transport for patients from an inpatient unit to a testing or procedure area, while maintaining the level of care that the patient is receiving on the unit itself. Originally a pilot program, it has flourished and grown to cover all intensive care and monitored units within Johns Hopkins. This program not only provides consistency in clinical care when the patient leaves the unit, but also allows the patient’s nurse to remain in the unit to care for other patients in their assignment. The interdisciplinary team can assist with or maintain virtually any monitor or machine found at the bedside during a transport, including a ventilator, intra-aortic balloon pump and ventricular assist device.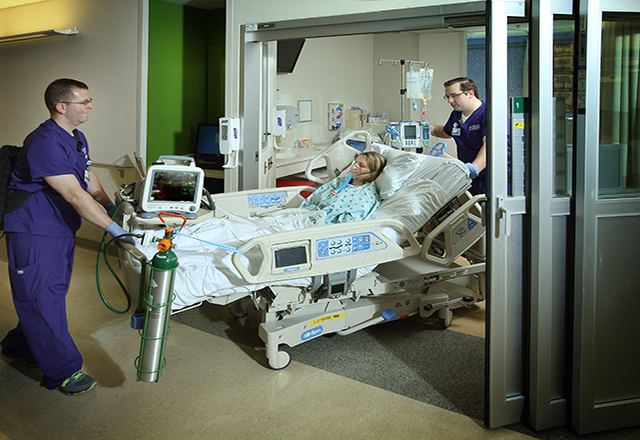
In addition, this team provides emergency transport from the adult emergency department for urgent cardiac intervention, and responds to staff/visitor medical emergencies throughout the campus. The multidisciplinary team approach and their expertise in transport medicine ensure that patients receive the highest level of care during a critical time away from the inpatient unit. -
 Lifeline presently uses several established fixed-wing programs to facilitate domestic and international patients being moved to a Johns Hopkins Health System hospital. These transports are arranged and coordinated through the Hopkins Access Line (HAL), which can be reached 24/7 at 1-800-765-5447.
Lifeline presently uses several established fixed-wing programs to facilitate domestic and international patients being moved to a Johns Hopkins Health System hospital. These transports are arranged and coordinated through the Hopkins Access Line (HAL), which can be reached 24/7 at 1-800-765-5447.
-
 The Lifeline Transport Team routinely provides Critical Care, ALS and BLS coverage at events that require on-scene medical personnel. Some of these events include events at The Johns Hopkins University and community events in East Baltimore.
The Lifeline Transport Team routinely provides Critical Care, ALS and BLS coverage at events that require on-scene medical personnel. Some of these events include events at The Johns Hopkins University and community events in East Baltimore.
-
The Lifeline Ground and Air Transportation Services Program is available to visit your hospital, service or program upon your request to discuss and educate your staff members about our program and services.
You may make a request by email: [email protected]
-
History
The Maryland Regional Neonatal Transport Program began over 25 years ago. The first neonatal transport team was developed at City Hospital (Francis Scott Key and now Johns Hopkins Bayview). Through the years the participation of various hospitals has changed. The participation of Johns Hopkins Hospital and University of Maryland Medical System dates back to 1981. The oversight for the program was also provided by the state of Maryland via the Maryland Institute of Emergency Medical Services Systems (MIEMSS) from 1981-1996. In 1997, the Maryland Regional Neonatal Transport Program became a joint partnership between Johns Hopkins Hospital and University of Maryland Medical System with oversight by the respective hospitals.
The team is staffed by Neonatal Nurse Practitioners/Transport Nurses and specially trained medics. Each institution provides staff, equipment and additional resources to provide for the function of the team. Hospital staff includes neonatal transport nurses/nurse practitioners and a shared coordinator. The ambulance vendor provides the dedicated EMT staff.
There is a rotating schedule between the hospitals, developed a year in advance. The schedule is completed by the transport nurses/nurse practitioners to ensure equal distribution of weekends, holidays, etc...
The Maryland Regional Neonatal Transport Program (MRNTP) performs over 700 transports on an annual basis. The program is an essential service for the neonatal community within the State of Maryland for multiple types of transports. Approximately 30 referral hospitals utilize the service. Two specially designed ambulances are dedicated to the team on a 24/7 basis. Each ambulance is capable of transporting up to two neonates simultaneously. The Maryland State Police provide helicopter support for air transports.
As part of our outreach education program, MRNTP offers a multitude of educational/didactic offerings, preceptorship programs, self?paced individual educational programs and comprehensive multidisciplinary chart reviews are available.
Most didactic programs have been approved for continuing education credit for nurses, respiratory therapists, and pre?hospital providers.
Mission Statement
The Maryland Regional Neonatal Transport Program supports the mission statements of University of Maryland Medical System and Johns Hopkins Hospital to provide comprehensive care and health care education to the community by:
- Promoting the physical health of the neonate.
- Initiating or continuing stabilization of the sick neonate.
- Collaborating with the multidisciplinary team in evaluating and making recommendations for treatment.
- Acting as an advocate for neonates and their families.
- Transporting the infant in the most safe, effective and efficient manner.
- Promoting an understanding of neonatal problems and their management throughout the hospital, community and state through outreach education, chart reviews, lectures and workshops.
-
Pediatric Specialty Team
The Pediatric Team is a service of the Johns Hopkins Children's Center (www.hopkinschildrens.org). The team is staffed by pediatric critical care nurses and physicians who accompany the Lifeline staff on pediatric calls by ground ambulance, helicopter, and fixed wing aircraft. All requests for pediatric transport are received by the transport team in the Pediatric Intensive Care Unit (PICU). The team triages the call to determine the need for specialty care prior to arrival of the team. The team uses specialized equipment to monitor and provide care for children from birth through eighteen years of age.
How to transfer a pediatric patient into Johns Hopkins
The Johns Hopkins Children's Center provides a wide range of pediatric specialty services including extracorporeal membrane oxygenation (ECMO) and is the designated Pediatric Trauma Center for Maryland. The pediatric transport service transports on average 160 patients each month. About 80% of the children are transported to the Pediatric Emergency Department and 20% are transported directly to the PICU which is a Division of Anesthesia and Critical Care (www.hopkinsmedicine.org/anesthesiology).
The Johns Hopkins Children's Center sponsors a variety of education programs for the care of pediatric patients. Courses that are offered include Pediatric Advanced Life Support (PALS), Emergency Nurse Pediatric Course (ENPC), and Advanced Life Support Trauma Course for Nurses (ATCN). For information about upcoming courses, contact the Hopkins Outreach for Pediatric Education (HOPE) Program.

