Vision
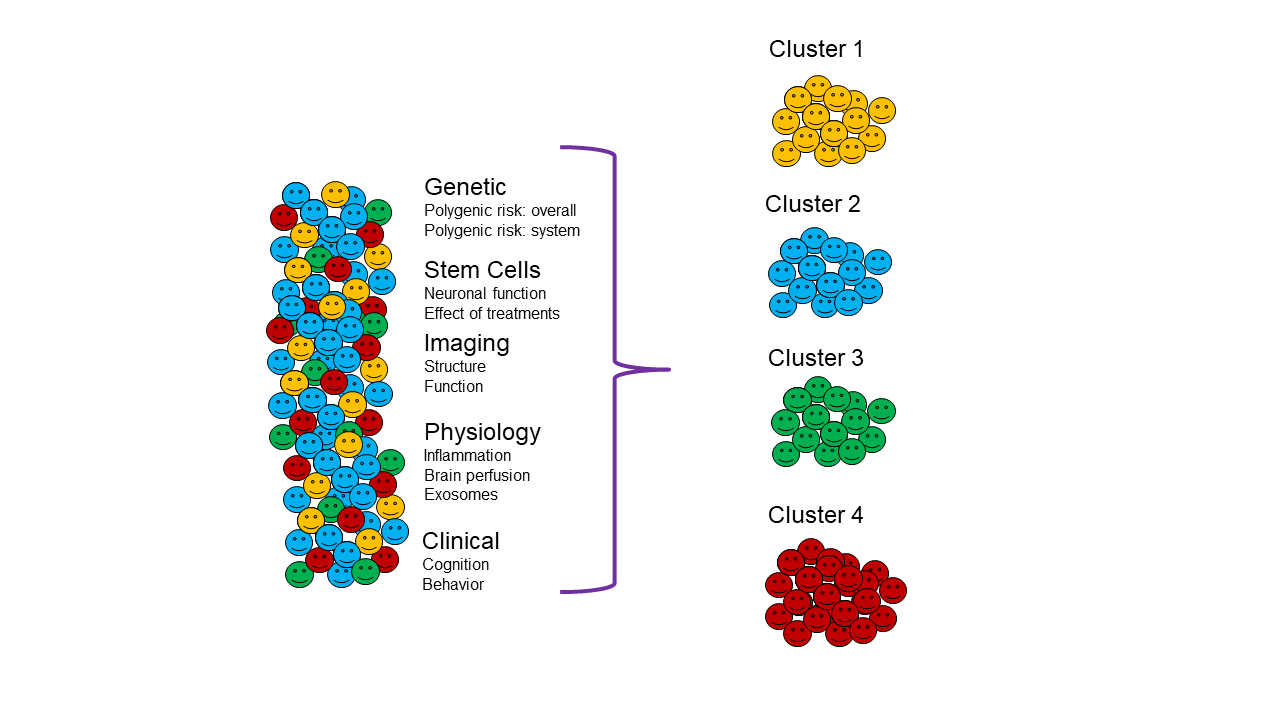
Recognizing that Alzheimer’s disease and related disorders (ADRD) are not unitary biologic entities, we seek to define subtypes of ADRD that are therapeutically relevant to identify the right treatment for the right patient at the right time.
Mission
Harnessing the power of exciting new methods such as artificial intelligence, advances in the understanding of extracellular vesicles, and stem cell derived individualized models of brain disease we seek to disrupt and accelerate treatment development targeting novel therapies to distinct ADRD subtypes.
Alzheimer's and Dementia Research
Big Data Power Analyzing Real World Data from Medical Records
How can we predict individuals at-risk for cognitive decline and faster progression?
Scaling Evidence-Based Care
How can cutting edge quality care be made available to all persons with ADRC throughout Johns Hopkins and beyond?
Expedite Discovery - Closing the Loop
How can we fast track the research from clinic to test tube and back to the clinic with blood biomarkers for subtyping and for advancing therapeutics?
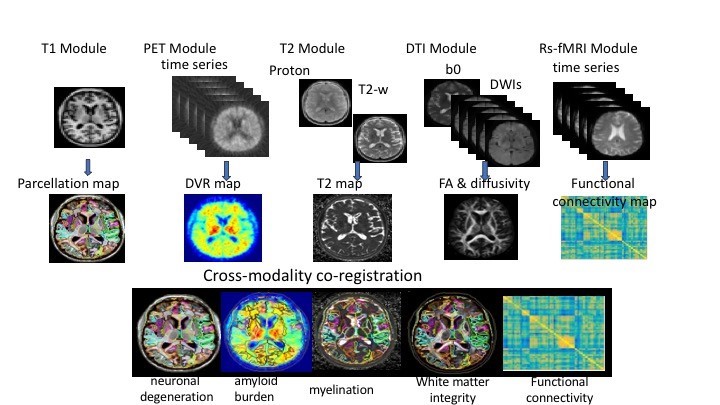
Innovation: Brain Scans
How can existing brain MRI methods be refined for early detection, prognosis, or predicting response to available medications?
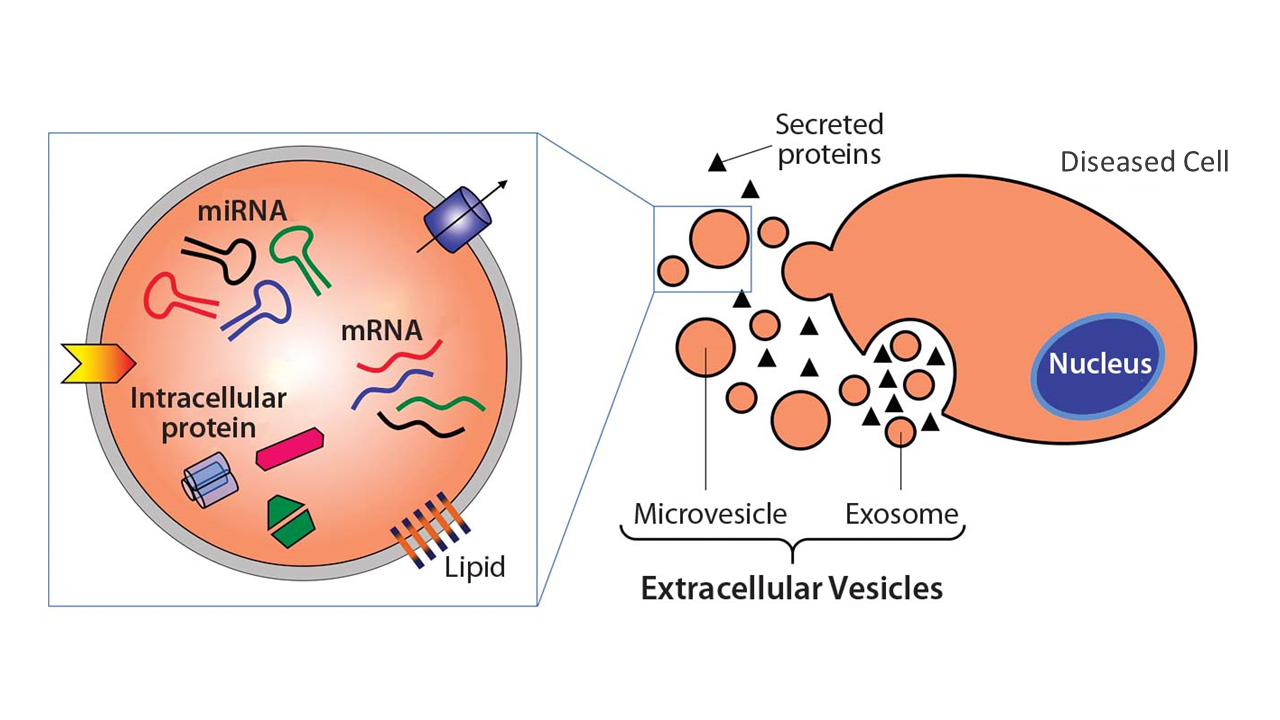
Innovation: New Blood Test
Can novel blood tests based on "extracellular vesicles (EVs)” be developed to learn about what’s going on in the brain so as to stage the ADRD brain disease and monitor treatment response?
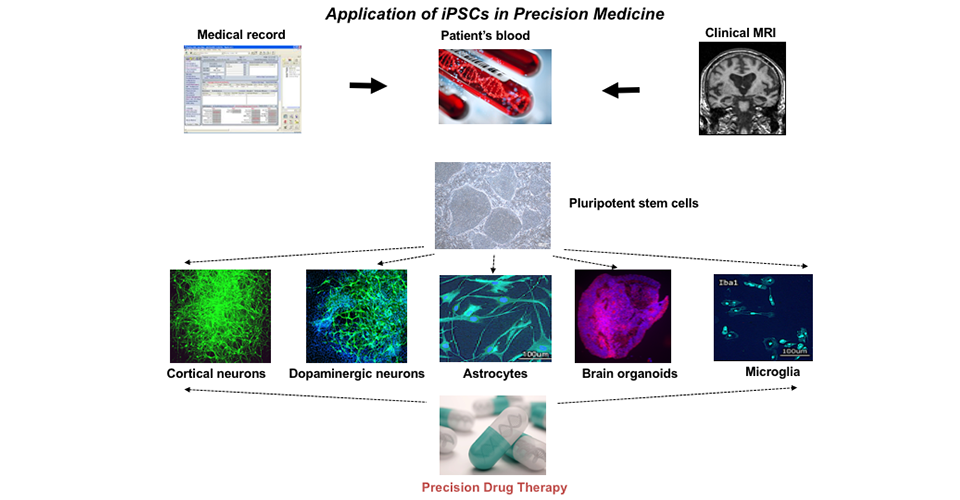
Innovation: Stem Cell Models
Can blood derived stems cells models be used to test whether individual patients will be helped by available and emerging medication treatments?
Deeper Dive Lecture and Panel Videos
-
2023 Visiting Lectureship in Memory Disorders and Alzheimer’s Disease
Dina Katabi, Ph.D. presented on “AI-Enabled Markers of Parkinson's Disease and Others.” (This panel was recorded May 16, 2023)
-
Dementia and Precision Medicine
Dr. Constantine Lyketsos presents the current medical knowledge and research to date on memory and Alzheimer's disease and answers frequently asked questions. ("What We Are Learning About Memory and Alzheimer's" was presented in April 10, 2021.)
Patient Care for Alzheimer's Disease
The research we do directly impacts the treatment options available to our patients. Find out more about patient care for Alzheimer's Disease.
The Johns Hopkins Memory and Alzheimer's Treatment Center
The Johns Hopkins Bayview Medical Center
5300 Alpha Commons Drive, Floor 4
Baltimore, MD 21224