Sigmoidoscopy
A sigmoidoscopy is a diagnostic test used to check the sigmoid colon, which is the lower part of your colon or large intestine. This section of your colon is close to your rectum and anus.
A sigmoidoscopy can help diagnose the following symptoms:
-
Belly pain
-
Polyps (abnormal growths)
-
Bleeding
A sigmoidoscopy may also be used to take a tissue sample or biopsy. And it can be used to remove polyps or hemorrhoids (swollen veins in your rectum and anus). It is also a screening test for colon cancer and rectal cancer.
A sigmoidoscopy is performed using a thin, flexible tube called a sigmoidoscope. The tube has a tiny light and a camera. The tube is put into your anus and moved slowly through your rectum into the lower part of your colon. The tube is used to blow air into your colon, which makes the colon swell up a bit to improve visibility.
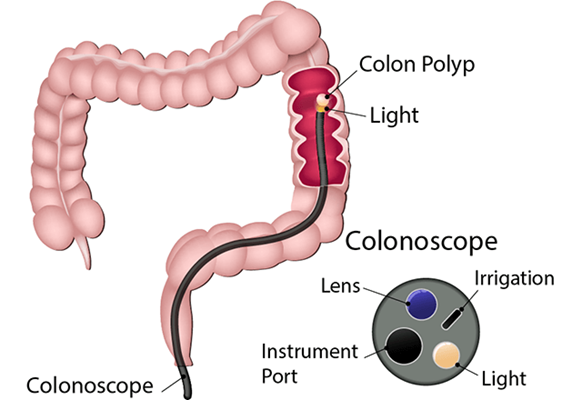
Why might I need a sigmoidoscopy?
A sigmoidoscopy may be used to examine or diagnose certain conditions or structures in your lower colon, including the following:
-
Polyps
-
Tumors
-
Ulcers (sores)
-
Inflammation (redness and swelling)
-
Hemorrhoids
-
Diverticula (pouches on your colon wall)
-
Strictures (narrowing of your lower colon)
It can also be used to investigate the following:
-
Changes in your bowel habits
-
Lower belly pain
-
Itching around your anus
-
Blood or mucus in your stool
-
Low iron levels
-
Low blood counts
A sigmoidoscopy is one type of test used to screen for colon and rectal cancers. Health experts recommend that both men and women follow a colon and rectal cancer screening schedule starting at age 50. Talk with your health care provider about a screening schedule that works for you. Many choices are available to screen for colon cancer.
Your health care provider may have other reasons to recommend a sigmoidoscopy. If a sigmoidoscopy shows polyps, a colonoscopy may be recommended as the next step to examine the remainder of the colon.
What are the risks of a sigmoidoscopy?
The following complications may occur after a sigmoidoscopy:
-
Continued bleeding after biopsy
-
Inflammation of the lining of your belly (peritonitis)
-
A perforation (hole) in your intestinal wall, which is a rare complication
The following problems or situations may interfere with a sigmoidoscopy:
-
Using laxative enemas before the test, which can irritate the lining of your colon
-
Having barium in your colon from another recent test used to check your colon
-
Inadequate bowel preparation before the procedure
-
Issues that may restrict the movement of the tube, including strictures, adhesions (surgical scars) or a disease such as chronic inflammatory disease
-
Rectal bleeding, which may restrict visibility
You may have other risks that are unique to you. Discuss any concerns with your health care provider before the procedure.
How do I prepare for a sigmoidoscopy?
Your health care provider will fully explain the procedure and answer your questions. You will be asked to sign a consent form prior to the test. Read the form carefully and ask questions you may have. Before your procedure, be sure to tell your health care provider:
-
If you are pregnant or think you may be pregnant
-
If you are sensitive to or allergic to any medicines, latex, tape or anesthesia medicines (local and general)
-
About all the medicines you take, including over-the-counter drugs, prescription medicines, vitamins, herbs and other supplements
-
If you have a history of bleeding disorders
-
If you are taking any blood-thinning medicines, aspirin, ibuprofen or other medicines that affect blood clotting; these drugs may need to be stopped before the procedure
Your health care provider will give you instructions on how to prepare your bowel for the test. You may be asked to take a laxative, an enema or a rectal laxative suppository. Or you may have to drink a special fluid that helps prepare your bowel. You will be given specific instructions about fasting (not eating) or following a special diet before the test.
Follow any other instructions your provider gives you to get ready for your sigmoidoscopy.
What happens during a sigmoidoscopy?
You may have a sigmoidoscopy in an outpatient setting or as part of your stay in a hospital. The way the test is done may vary depending on your condition and your health care provider's practices. You usually will not need a sedative (medicine to help you relax) or anesthesia (medicine to put you into a deep sleep) before the test.
Preparation and Positioning
Before the procedure, you will be asked to remove any jewelry or other objects that may interfere with the procedure. You may be asked to remove your clothing and change into a hospital gown.
To get you into the proper position, you may be asked to lie on the exam table on your left side with your knees bent towards your chest. Or you may be put in the knee-chest position, which involves kneeling with your head and chest bent down, touching the table.
Sigmoidoscopy Process
Generally, a sigmoidoscopy follows this process:
-
Your provider will do a rectal exam to check for any blood, mucus or stool. He or she will also gently dilate (enlarge) your anus.
-
Your provider will slowly insert a lubricated tube into your anus and move it into your rectum and the lower part of your colon. After the lower part of your colon is checked, the tube will be removed.
-
Air may be injected into your bowel to improve visibility. A suction device may be used to remove liquid stool.
-
A sigmoidoscopy may be done together with an anoscopy (a test to check your anus) or a proctoscopy (a test to check your anus and rectum). If another test is done, a special tube will be inserted to check your lower rectum or anal canal.
A sigmoidoscopy can cause mild discomfort. You may feel a strong urge to have a bowel movement when the tube is inserted. You may also have brief muscle spasms or lower belly pain during the test. Taking deep breaths while the tube is being inserted may help decrease any pain.
Biopsy
During the test, biopsies (tissue samples) may be taken from the lining of your large intestine. This will be done using a special brush, forceps or a swab. If a polyp is seen, it may be removed, biopsied or left alone until a future surgery is performed.
What happens after a sigmoidoscopy?
You should lie on your side or back for a few minutes before getting up from the table. Move slowly when you stand up. This will help you feel less dizzy from having your head down during the test.
You may go back to your normal diet and activities, unless your doctor gives you other instructions.
If a biopsy or polyp was removed during the test, you may see a small amount of blood in your bowel movements. This bleeding should stop within a day or so.
It is normal for patients to be very flatulent (pass a lot of gas) and have gas pains after the test. Walking and moving around may help to ease any mild pain.
Call your health care provider if you experience any of the following:
-
Fever or chills
-
Bleeding from the rectum that lasts longer than a day
-
Belly pain or swelling
-
The inability to pass gas
Your health care provider may give you other instructions related to your specific situation.