Treating Lymphedema
What You Need to Know
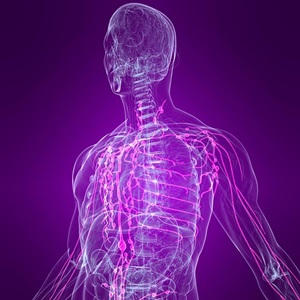
- The lymphatic system is made up of many vessels that carry fluid throughout the body.
- Lymphedema is an abnormal buildup of protein-rich fluid in any part of the body as a result of malfunction in the lymphatic system. You can be born with it (primary lymphedema) or develop it as a result of damage to the lymphatic system, such as after surgery or infection (secondary lymphedema).
- Early-stage lymphedema can be treated with nonsurgical interventions, including medication, a healthy diet and manual compression.
- For advanced-stage lymphedema, surgical intervention may be recommended.
Lymphedema Prevention
People who have had surgery to remove lymph nodes in the armpit should be aware of those activities that put too much pressure on the affected arm. Protective measures to avoid injury and infection include:
Maintaining Proper Hygiene
-
Clean the skin of the affected arm daily and apply lotion. When drying the arm, be gentle but thorough.
-
Take proper care of the fingernails and avoid cutting cuticles.
-
Clean all cuts with soap and water, and then apply antibacterial ointment and a sterile dressing.
Staying Fit
-
Do exercises regularly to improve drainage, but first consult with your doctor or physical therapist.
-
Eat a well-balanced, low-sodium diet.
-
Keep the arm elevated when possible.
Taking Precaution with Everyday Activities
-
Protect your fingers from needle pricks and sharp objects. Use a thimble when sewing.
-
Avoid vigorous, repetitive movements against resistance, such as scrubbing, pulling or pushing, with the affected arm.
-
Avoid sunburns and other burns to the affected arm.
-
Use an electric shaver when shaving underarms.
Wearing the Right Attire
-
Wear gloves when gardening and when using strong household detergents.
-
Do not wear nightgowns or clothing with elastic cuffs.
-
Carry your handbag or heavy packages in the unaffected arm.
Speaking Up at Your Doctor’s Office
-
Make sure that all injections are given and blood tests are drawn in the unaffected arm.
-
If at all possible, have all blood pressure tests done on the unaffected arm.
-
Avoid extreme hot or cold temperatures on the affected arm, such as heating pads or ice packs.
-
Notify your doctor immediately of any signs of infection, such as redness, pain, heat, increased swelling or fever.
Talk with your doctor about what you can do to try to prevent lymphedema from happening to you. If lymphedema does develop, let your doctor know right away. There are things you can do to try to keep it from getting worse.
Lymphedema Causes
Lymphedema occurs as a result of a blockage in the lymphatic system. This is most often caused by a traumatic event, such as sports injuries or deep cuts and bruises, as an aftereffect of surgery or cancer treatment. More rarely, lymphedema can occur as birth defect or symptom of infection.
Breast Cancer: Lymphedema After Treatment

Some women who have undergone treatment for breast cancer develop lymphedema after their treatment.
Lymphedema Diagnosis
There are no specific diagnostic tests for lymphedema. The doctor will complete a medical history and physical examination. The medical history may include questions regarding the following:
-
Past surgeries -
History of edema (severe swelling)
-
Current medications
-
Other medical conditions, such as high blood pressure, heart disease or diabetes
Onset of symptoms (When did the swelling appear?)
Stages
Upon diagnosis, your doctor will identify which stage best characterizes your lymphedema and diagnose treatment accordingly. Depending on how the swelling has progressed, your doctor will identify the following stages:
-
Stage 1: Abnormal flow in the lymphatic system. No signs or symptoms
-
Stage 2: Accumulation of fluid with swelling. Swelling resolves with elevation. Pressing on the area may leave a dent
-
Stage 3: Permanent swelling that does not resolve with elevation. Pressing on the area no longer leaves a dent. Changes in the skin with scarring and thickening
-
Stage 4: Elephantiasis (large deformed limb), skin thickening with “wart-like” growth and extensive scarring
Lymphedema vs. Lipedema | Q&A
Lymphedema Treatment
Decongestive Therapy for Lymphedema
Treatment for lymphedema depends on the severity and extent of the condition. Prevention and controlling lymphedema play an important role with this condition since there is no cure.
Decongestive treatment is commonly recommended for the first two stages of lymphedema. Treatment options may include:
-
Exercise. Exercise helps to restore flexibility and strength, and it improves drainage. Specific exercises will be recommended by your doctor and/or physical therapist.
-
Bandage. Wearing a customized compression sleeve or elastic bandage may help to prevent an accumulation of fluid.
-
Arm pump. Applying an arm pump often helps to increase the fluid flow in the lymphatic vessels and keeps fluid from collecting in the arm.
-
Diet. Eating a well-balanced diet and controlling body weight is an important part of treatment.
-
Keep the arm raised. Keeping the arm raised above the level of the heart, whenever possible, allows gravity to help drain the accumulated fluid.
-
Infection Prevention. It is important to follow preventive measures, such as good skin care, to protect the affected arm from infection and skin breakdown.
Surgical Treatment of Lymphedema
Once lymphedema has progressed to stages 3 or 4, surgical intervention may be recommended. Surgical options include both physiological and excisional procedures. Both procedures aim to restore lymphatic flow. However, physiological procedures involve rewiring the lymphatic system within the limb, while excisional procedures focus on removing diseased tissue.
Physiological Procedures (may be recommended for stages 3 and 4)
-
Vascularized lymph node transfer. The surgeon transfers healthy lymph nodes to the affected area and rewires the lymphatic system to reduce swelling.
-
Lymphaticovenous anastomosis (also referred to as lymphovenous bypass). The surgeon rewires the lymphatic system by connecting lymphatic channels directly to tiny veins nearby. This is an outpatient procedure with very small and minimal incisions and very little blood loss.
Excisional Procedures (may be recommended for stages 3, 4 or 5)
-
Liposuction. The affected tissue can be removed.
-
Charles procedure. The surgeon will remove affected tissue and use a part of it as skin grafts to repair the area. This is a more invasive procedure, typically recommended for stages 4 and 5.
Lymphedema: What Are Your Surgical Options?
There are several treatment options available for lymphedema. Find out what stage you’re in to see medical and surgical options.







