Myelogram
What is a myelogram?
A myelogram is a diagnostic imaging test generally done by a radiologist. It uses a contrast dye and X-rays or computed tomography (CT) to look for problems in the spinal canal. Problems can develop in the spinal cord, nerve roots, and other tissues. This test is also called myelography.
The contrast dye is injected into the spinal column before the procedure. The contrast dye appears on an X-ray screen allowing the radiologist to see the spinal cord, subarachnoid space, and other nearby structures more clearly than with standard X-rays of the spine.
The radiologist will also use a CT scan when doing a myelogram. A CT or CAT scan is an imaging test that uses X-rays and a computer to make detailed images of the body. A CT scan shows details images of the spinal canal. CT scans show more details than standard X-rays.
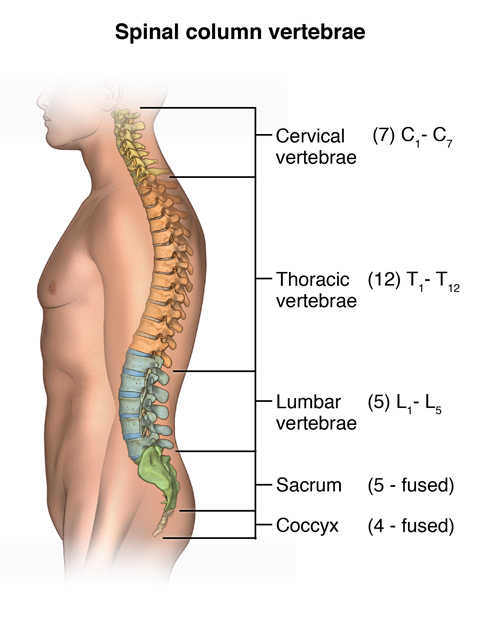
Why might I need a myelogram?
A myelogram may be done to assess the spinal cord, subarachnoid space, or other structures for changes or abnormalities. It may be used when another type of exam, such as a standard X-ray, does not give clear answers about the cause of back or spine problems. Myelograms may be used to evaluate many diseases, including:
- Herniated discs (discs that bulge and press on nerves and/or the spinal cord)
- Spinal cord or brain tumors
- Infection and/or inflammation of tissues around the spinal cord and brain
- Spinal stenosis (degeneration and swelling of the bones and tissues around the spinal cord that make the canal narrow)
- Ankylosing spondylitis (a disease that affects the spine, causing the bones to grow together)
- Bone spurs
- Arthritic discs
- Cysts (benign capsules that may be filled with fluid or solid matter)
- Tearing away or injury of spinal nerve roots
- Arachnoiditis (inflammation of a delicate membrane that covers the brain.)
There may be other reasons for your healthcare provider to recommend a myelogram.
There may be other reasons for your healthcare provider to recommend a myelogram.
What are the risks of a myelogram?
There is a risk of an allergic reaction to the contrast dye. Be sure to let your healthcare provider know if you have ever had a reaction to any contrast dye.
Because the contrast is injected into the cerebrospinal fluid (CSF) which also surrounds the brain, there is a small risk of seizure after the injection.
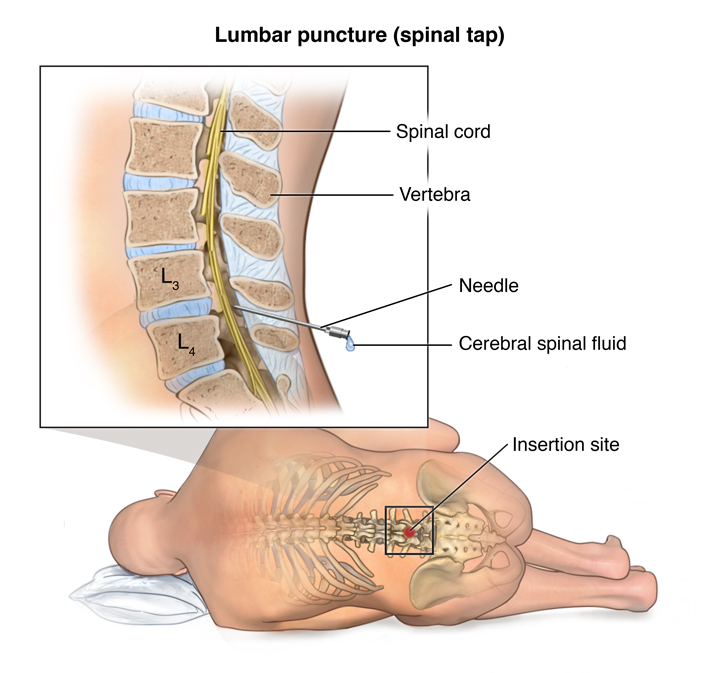
Because this procedure involves a lumbar puncture, these potential complications may occur:
- A small amount of CSF can leak from the needle insertion site. This can cause headaches after the procedure. If there is a persistent leak the headache can be severe.
- There is a slight risk of infection because the needle breaks the skin's surface, providing a possible entry point for bacteria.
- Short-term numbness of the legs or lower back pain may be experienced.
- There is a risk of bleeding in the spinal canal.
There may be other risks depending on your specific medical condition. Be sure to discuss any concerns with your healthcare provider before the procedure.
How do I get ready for a myelogram?
If you are having a myelogram at Johns Hopkins Hospital or Bayview Medical Center, a neuroradiologist or radiology nurse will contact you by phone two or three days prior to your myelography to discuss the procedure and answer any questions you may have.
Please inform the neuroradiologist/nurse if:
- You are on antibiotics - you may need to wait to do the procedure if currently on antibiotics for an in infection in your blood. If you have an active infection or fever, your procedure may need to be rescheduled.
- You have a history of seizures
- You are allergic to any local anesthetics (lidocaine) or IV contrast
- There is any chance that you could be pregnant
- You are on anticoagulant therapy (blood thinners)
PRECAUTIONS: If you are pregnant or think you might be pregnant, please check with your doctor before scheduling the exam. Options should be discussed with you and your doctor.
CLOTHING: You may be asked to change into a gown. A gown will be provided for you. However, the procedure may also be done while you remain in your clothes from home. For this reason, try to wear non-restrictive, comfortable clothing and slip on shoes if possible. Please remove all piercings and leave all jewelry and valuables at home.
EAT/DRINK: Try to increase your fluid intake (such as water and juice) for the two days leading up to your procedure unless a medical condition does not allow you to safely do so. If you are not sure if it is safe for you, contact your primary care provider or referring provider.
However, on the day of the procedure, do not eat for three hours before the procedure. You may have liquids and can take your usual medications unless previously advised to hold certain medications in preparation for the myelography.
MEDICATION: All patients can take their prescribed medications as usual unless instructed to hold certain medications such as blood thinners. Please bring a current list of your medications and allergies with you.
TRAVEL: You must have an adult driver accompany you so they can drive you home after the procedure. This is for your safety and comfort.
- Arrive one hour prior to the scheduled procedure time for check-in and to be prepped for the procedure.
- Please note: You will be unable to drive for 24 hours after the procedure. If you are taking a cab or using public transportation, you need to bring a friend or family member to accompany you after the procedure to your home or hotel. A cab or public transportation driver is not considered an escort.
What happens during a myelogram?
A myelogram may be done on an outpatient basis or as part of your stay in a hospital. For outpatients, please allow four hours for the preparation, procedure, and recovery time.
Generally, a myelogram follows this process:
- Your healthcare provider will explain the procedure to you and ask if you have any questions.
- You will be asked to sign a consent form that gives your permission to do the procedure. Read the form carefully and ask questions if anything is not clear.
- You may be asked to remove any clothing, jewelry, or other objects that may interfere with the procedure.
- You may be asked to wear a gown. However, the procedure may also be done while you remain in your clothes from home. For this reason, please try to wear non-restrictive, comfortable clothing and slip on shoes if possible.
- You will be reminded to empty your bladder prior to the start of the procedure.
- During the procedure, you will lie on your stomach on a padded table.
- Your back will be cleaned with an antiseptic solution and draped with sterile towels.
- The radiologist will numb the skin by injecting a local anesthetic (numbing) drug using a thin needle. This injection may sting for a few seconds, but it makes the procedure less painful.
- A needle will be inserted through the numbed skin and into the space where the spinal fluid is located. You will feel some pressure while the needle goes in, but you must remain still.
- The radiologist will remove some of the spinal fluid from the spinal canal. Next, a small amount of contrast dye will be injected into the spinal canal through the needle. You may feel a warming sensation when the contrast dye is injected.
- The X-ray table will be tilted in various directions to allow gravity to help move the contrast dye to different areas of your spinal cord. You will be held in place by a special brace or harness. More contrast dye may be given during this process through the secured lumbar puncture needle.
- The needle is then removed and the X-rays and/or CT scan pictures are taken.
- You should tell the radiologist right away if you feel any numbness, tingling, headache, or lightheadedness during the procedure.
You may experience discomfort during the myelogram. The radiologist will use all possible comfort measures and complete the procedure as quickly as possible to minimize any discomfort or pain.
What happens after a myelogram?
You need to sit or lay down for several hours after the procedure to reduce your risk of developing a CSF (cerebral spinal fluid) leak. Most patients are asked to lie down for two hours after the procedure. If you need to urinate, you may need to do so in a bedpan or urinal during the time that you need to stay flat.
You will be asked to drink extra fluids to rehydrate after the procedure. This helps to wash out the contrast dye and it helps your body replace the spinal fluid that was removed. It also reduces the chance of developing a headache.
When you have completed the recovery period, you will be taken to your hospital room or discharged to your home. If you go home, usually your healthcare provider will advise you to rest for the remainder of the day
Once you are at home, tell your doctor of any changes including:
- Numbness and tingling of the legs
- Blood or other drainage from the injection site
- Pain at or near the injection site
- Nausea or vomiting
- Inability to urinate
- Fever
- Stiff neck
- Leg numbness
- Headaches
If the headaches persist for more than 24 hours after the procedure, or are worse when you change positions, contact the neuroradiology team with the phone number provided on your discharge instructions.
You may be instructed to limit your activity for 24 hours after the procedure.
Your healthcare provider may give you other specific instructions about what you should do after a myelogram.