Mammogram Age Guidelines: What You Need to Know
Featured Expert:
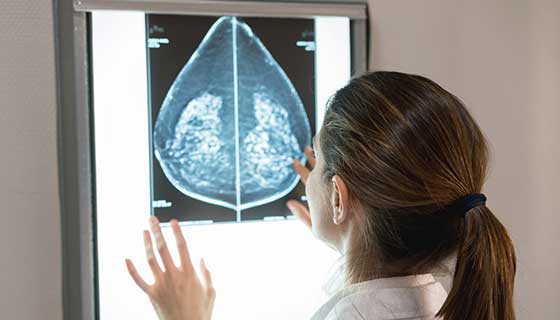
Annual mammograms are the best way to detect breast cancer early, when treatment is most effective. Yet changing national guidance about what age to start – from 40 to 50 and now back to 40 again – can be confusing.
Pouneh Razavi, M.D., director of Breast Imaging in the National Capital Region, oversees breast imaging operations at the Sullivan Breast Center at Sibley Memorial Hospital and Johns Hopkins Medical Imaging in Bethesda. She cuts through the clutter with clear advice for breast cancer screenings.
Q: What are the latest national guidelines for breast cancer screenings?
A: The Society of Breast Imaging recommends that a woman at average risk for breast cancer women begin getting annual mammograms at age 40.
Q: Why should screening mammograms begin at 40 – not at 50 – years of age?
A: Data show that one out of six new breast cancers develop in people who are in the age range of 40 to 50. Cancers detected during screenings are usually early-stage, and the earlier we catch a cancer, the better the prognosis and survival rate for the patient.
At Johns Hopkins, we have always recommended that our patients start screening at age 40.
Q: Can false positives be reduced in mammograms?
A: At Johns Hopkins Medicine, the only clinicians who read breast imaging are radiologists who have been fellowship-trained in breast imaging. This helps us keep our false positives rates down across the whole Hopkins system.
Studies show that when you have radiologists dedicated to reading just mammograms, as opposed to a wide range of screenings, they tend to flag fewer mammograms for follow-up, and the ones they flag turn out to be true positives.
To keep false positive rates down we also encourage consultations among the radiologists who are reading the scans.
Q: Should some people start getting mammograms before the age of 40?
A: Yes. We always tell patients to have this conversation with their gynecologist or referring physician. For example, patients with a higher-than-average risk, for example because they have a family history of breast cancer or known genetic mutations such as the BRCA gene, are generally urged to start earlier.
Q: Is there an age when women no longer need breast cancer screenings?
A: The guidelines do not include recommendations for women after age 74, as there is limited data on whether mammograms save lives in that age group. But we have patients who are much older than that and healthy, who would benefit from early detection that would inform treatment decisions. As long as the patient is in good health otherwise, we recommend that they continue getting annual mammograms.
Q: What is the current mammogram guidance for women with dense breasts?
A: Updated Food and Drug Administration regulations require mammography facilities to notify patients about the density of their breasts so they can consult with their physicians about whether additional screening is needed.
Dense breasts can make cancers more difficult to detect. All of our Hopkins sites offer 3D mammography, which gives us much more information because it lets us see the layers of cells, one millimeter at a time.
Q: Should you keep your old mammogram images?
A: Mammography works best when we can compare new images to older ones. We ask our patients to please bring any previous mammogram images to a new mammogram appointment at our facility. Comparing current mammogram images to prior images can be very helpful in assessing for a change. Even if you had a mammogram 15 years ago and you don’t think it’s useful, it is.
Schedule a Mammogram
Learn more about our breast imaging locations: