Endoscopic Ultrasound
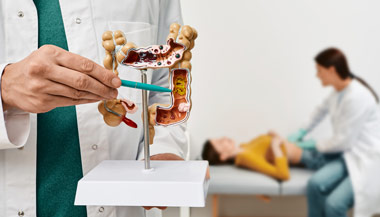
Endoscopic ultrasound (EUS) combines two techniques — endoscopy and ultrasound — to help doctors see, evaluate and diagnose conditions in and near the gastrointestinal (GI) tract.
What You Need to Know
- Endoscopic ultrasound, also called endoscopic sonography, uses a special endoscope with an ultrasound probe.
- EUS can be used to examine problems not only in the GI tract but also in nearby organs, including the pancreas and liver.
- Depending on where the area of concern is in your body, the gastroenterologist will introduce the EUS device through the mouth or the anus.
- EUS is usually an outpatient procedure, meaning you can go home the same day.
What is an endoscopic ultrasound?
Endoscopic ultrasound is a minimally invasive procedure that uses a camera device (endoscope) together with high frequency sound waves (ultrasound) to examine the GI tract and beyond.
A regular endoscope is a thin, lighted tube that can be inserted through the mouth or anus to view inside your esophagus, stomach or intestines. EUS uses a special endoscope with a small ultrasound device on its tip, called an echoendoscope. Addition of ultrasound lets the doctor see the GI tract and surrounding organs.
How does endoscopic ultrasound work?
Endoscopic ultrasound works similar to abdominal ultrasound, except the source of the sound waves is inside your body. As the high frequency sound waves travel from the echoendoscope, they hit tissues of various density and bounce back. For example, endoscopic ultrasound can pick up outlines of a tumor or a cyst, which the computer then processes and displays as lighter and darker areas on the screen.
Because the sound waves don’t need to pass through the skin and muscle to reach internal organs, endoscopic ultrasound offers a better view of the GI tract and nearby organs than abdominal ultrasound. It may also be more precise in identifying small tumors and cysts that other imaging methods such as MRI (magnetic resonance imaging) and CT (computerized tomography) can miss.
During EUS, the gastroenterologist can take a tissue sample (biopsy) of a suspicious lesion by using a thin needle fed through the echoendoscope. This procedure, called fine-needle aspiration, can be used to collect cells and tissues from the pancreas, liver and other organs adjacent to the GI wall. Biopsy can determine the presence of cancer and examine its characteristics.
What is endoscopic ultrasound used for?
EUS can help diagnose conditions in the upper GI tract (esophagus, stomach and duodenum), the lower GI tract (colon and rectum) and nearby organs including the lungs, pancreas, liver and gallbladder. Endoscopic ultrasound can be used to better examine areas of concern identified by other imaging tests such as an X-ray, MRI or CT.
Your gastroenterologist may recommend EUS to:
- Locate tumors or cysts in the pancreas
- Help diagnose chronic pancreatitis
- Assess cancerous areas of the esophagus, stomach, colon or rectum, and help with staging cancers (determining how advanced or aggressive they are); ultrasound helps detect whether the cancer has affected major lymph nodes or blood vessels
- Detect stones in the biliary ducts
- Drain pancreatic pseudocysts or other abnormal fluid collections in the abdomen
- Treat the pancreas and liver with precise medicine delivery
Preparing for Endoscopic Ultrasound
Your doctor will provide specific instructions on how to prepare for EUS. The steps will vary depending on whether you are having upper GI or lower GI ultrasound, and may include fasting, a liquid diet, bowel prep or a combination of these steps. The goal is to make sure your digestive tract is clear of food and waste so the doctor can see the interior clearly.
Make sure your doctor knows about any allergies you have and all the medications and supplements you take. The doctor will instruct you on taking your medications before the procedure.
Make sure a responsible adult can take you home after the procedure, since you might be drowsy from anesthesia.
What happens during endoscopic ultrasound?
- An IV will be placed into your vein to receive fluids and a medication to make you relaxed and drowsy.
- The doctor will pass the echoendoscope through your mouth for upper GI ultrasound or your rectum for lower GI ultrasound. If you are having an upper GI EUS, the doctor may apply an anesthetic to your throat to make the procedure more comfortable.
- The doctor observes the images on a nearby monitor and adjusts the direction of the sound waves to get a clear image.
- If EUS identifies a suspicious area, the doctor may collect a small sample of cell or tissue using the fine-needle aspiration technique.
- If EUS reveals an abnormal fluid collection, such as a pseudocyst, the doctor may use the echoendoscope to place a stent to drain it.
How long does the endoscopic ultrasound procedure last?
Simple exploratory endoscopic ultrasound typically takes less than an hour to complete. If a biopsy or a cyst is drained during EUS, the procedure may take longer.
Your doctor may instruct you to arrive at the treatment facility an hour or so before the EUS is scheduled so that preparation for the procedure can begin. This can extend the total time of the procedure.
What to Expect After Endoscopic Ultrasound
When the procedure is finished, you will be in the recovery room until the sedative starts to wear off. Your doctor will discuss the initial findings with you, but you may need to wait a few days for the results of a biopsy if one was performed.
After you talk to the doctor, your care partner can drive you home, where you should rest for the remainder of the day. As you recover from EUS, you might experience:
- A sore throat or tongue, or swollen lips if the endoscope was inserted through your mouth
- Nausea or vomiting
- Excessive intestinal gas
- Stomach bloating or cramping
Serious side effects are rare. If you experience severe or persistent abdominal pain, very dark bowel movements, fever or chest pain, contact your doctor or go to an emergency room.
If a problem is diagnosed on the basis of your endoscopic ultrasound, your doctor will follow up with you to discuss the next steps and, if needed, to start treatment.