Venous Disease
Venous Disease Overview
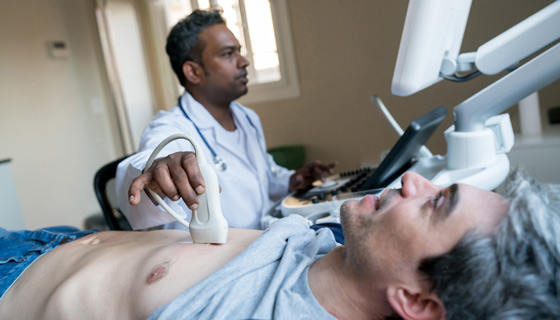
Veins are thin-walled structures inside of which a set of valves keeps blood in the body flowing in one direction. The heart pumps oxygen-rich blood to the body’s tissues through thicker-walled arteries; the veins return that blood to the heart. Veins located close to the surface of the skin are called superficial veins and the veins found in the muscles of the arms and legs are called deep veins.
Damaged vein walls hinder the circulatory system, allowing blood to collect and flow in a retrograde (backward) fashion when the muscles relax. This creates an unusually high pressure buildup in the veins. This buildup causes further stretching and twisting of the veins, increased swelling, more valve incompetence, sluggish blood flow and potential blood clot formation. Eventually, this condition can lead to various disorders known as venous disease.
Venous disease is quite common. Approximately 15 percent of the United States population is affected by varicose veins, which generally do not pose great health risk. However, thrombophlebitis can be much more serious, even life-threatening, affecting millions of people each year.
Varicose Veins
Varicose veins are twisted, swollen veins near the surface of the skin and occur when weak or defective valves allow blood to flow backward or stagnate within the vein. Chronic obstruction of the veins can also cause varicose veins, but in most cases no underlying abnormality can be identified. Varicose veins are quite common, though women are affected twice as often as men. Usually appearing in the legs, varicose veins may also occur in the anus, where they are known as hemorrhoids. While not a serious health risk, varicose veins can be eliminated for cosmetic reasons or if they cause discomfort.
Superficial Thrombophlebitis
Thrombophlebitis is the inflammation of a vein (usually in an extremity, especially one of the legs) that occurs in response to a blood clot in the vessel. When it occurs in a vein near the surface of the skin, it is known as superficial thrombophlebitis, a minor disorder commonly identified by a red, tender vein.
Deep-vein Thrombophlebitis
Deep-vein thrombophlebitis (affecting the larger veins farther below the skin’s surface) is more serious. It may produce less-pronounced symptoms at first (half of all cases are asymptomatic) but carries the risks of pulmonary embolism (when the clot detaches from its place of origin and travels to the lung) and chronic venous insufficiency (impaired outflow of blood through the veins), resulting in dermatitis, increased skin pigmentation and swelling.
When to Call Your Doctor
Call your doctor if you have a painful, swollen vein that does not disappear in a few days, or if you have unexplained swelling in an arm or leg.
Symptoms
Symptoms of venous disease include:
- Varicose Veins: enlarged, swollen, knotted clusters of purple veins; edema (swelling in the legs); aching or a sensation of heaviness in the legs; itching skin above the affected veins; skin discoloration and ulcers on the inner aspect of the ankles (in advanced cases).
- Superficial thrombophlebitis: a red, engorged, cordlike vein, associated with localized swelling, pain or tenderness.
- Deep-vein thrombophlebitis: generalized swelling, warmth and redness in the affected limb; distention of superficial veins; bluish skin color in the limb or toes (cyanosis); and rarely, fever and chills.
Johns Hopkins Vein Center

The Johns Hopkins Vein Center provides advanced minimally-invasive procedures and treatments for a variety of vein disorders.
Causes
The cause of venous disease varies but may be caused by one or more of the following factors:
- Stagnation of blood flow due to immobility. This is common among bedridden patients (such as heart patients and those who have undergone any type of major or orthopedic surgery, especially of the hip or knee) and healthy persons who sit or lie still for an extended period --for example, on a long trip.
- Blood vessel injury, caused by trauma, intravenous catheters or needles, chemotherapeutic agents, or infectious organisms.
- Conditions that increase the tendency for blood to coagulate, such as a familial deficiency in anti-clotting factors or disorders like systemic lupus erythematosus.
- Pregnancy and varicose veins are associated with a higher risk of superficial thrombophlebitis.
- Deep-vein thrombophlebitis is associated with a number of different cancers.
Prevention
Follow prevention tips as recommended by your doctor. These can include walking, controlling weight, wearing low-heeled shoes and avoiding long periods of sitting or standing in one position.
Be sure to stand up and walk around often on long trips in airplanes or automobiles.
Following a heart attack or major surgery, low doses of an anticoagulant (such as heparin or warfarin) may be recommended. Getting up and walking around again as soon as possible following either of those events is also advised.
Diagnosis
Varicose vein diagnosis may be made by observation of veins and does not require a doctor. In some cases x-rays may be taken after a contrast medium is injected into the veins (venography) to highlight them.
Doctors can usually diagnose superficial thrombophlebitis based on your medical history and a physical examination.
Treatment
Doctors at Johns Hopkins recommend the following for treating varicose veins:
- Elevated feet. Raise the foot of your bed from two to four inches with blocks to aid circulation at night.
- Avoid scratching itchy skin above varicose veins, as this may cause ulceration or profuse bleeding.
- Special elastic support stockings may be recommended by your doctor to prevent blood from pooling in the veins.
Surgical options for treating varicose veins include the following:
- Sclerotherapy is an option for superficial varicose veins. In this outpatient procedure, the doctor injects small- and medium-sized varicose veins with a solution that scars those veins. The process closes the veins, forcing your blood to reroute to healthier blood vessels.
- Laser therapy and other evolving technologies are among newer options.
- Surgical ligation (tying off) and removal (stripping) of the varicose vein is the definitive therapy in severe cases. Other veins compensate for the absent ones.
Non-surgical care for thrombophlebitis may include:
- If superficial thrombophlebitis is the diagnosis, your doctor will recommend you be up and active. You also should be checked frequently to make sure that the blood clot does not progress.
- Patients with deep-vein thrombophlebitis may require hospitalization, though some patients can be seen on an outpatient basis. Bed rest and elevation of the affected limb are essential. The doctor will usually prescribe an anti-clotting medication, usually heparin, to be given intravenously for seven to ten days. Outpatients are given anti-clotting pills.
- Clot-dissolving agents, such as urokinase or tissue plasminogen activator, may be administered to resolve the condition.
- Special elastic support stockings may be prescribed to aid circulation in the lower limbs.
- The doctor may implant a small filter in the main vein of your abdomen to prevent clots in the legs from going to the lung.