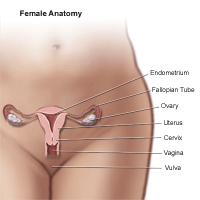
Vaginitis
What is vaginitis?
Vaginitis refers to any inflammation of the vagina. Inflammation may be infectious or noninfectious. It's common in women of all ages. One-third of women have at least one form of vaginitis at some time during their lives.
When the walls of the vagina become inflamed, because some irritant has disturbed the balance of the vaginal area, vaginitis can occur.
What causes vaginitis?
Bacteria, yeast, viruses, chemicals in creams or sprays, and even clothing can cause vaginitis. Sometimes, it occurs from organisms that are passed between sexual partners. Also, a number of different factors can affect the health of your vagina. These include your overall health, your personal hygiene, medicines, hormones (particularly estrogen), and the health of your sexual partner. Changes in any of these factors can trigger vaginitis.
These are the most common types of vaginitis:
-
Candida or "yeast" infection
-
Bacterial vaginosis
-
Trichomoniasis vaginitis
-
Viral vaginitis
-
Noninfectious vaginitis
Your health care provider will consider other causes of vaginal discharge such as gonorrhea and chlamydia. These organisms don't infect the vagina directly. If left untreated, they can lead to serious conditions, such as pelvic inflammatory disease (PID). PID increases a woman's risk of infertility, pelvic scarring, chronic pelvic pain, and ectopic pregnancy. Chlamydia is one of the most common sexually transmitted diseases in the U.S., although it often goes undiagnosed.
What is candida or "yeast" infections?
Yeast infections, as they are commonly called, are caused by one of the many species of fungus known as candida. It normally lives in the vagina in small numbers. Candida can also be present in the mouth and digestive tract in both men and women.
Yeast is normally present and well-balanced in the vagina. Infection occurs when something upsets this normal balance. For example, taking an antibiotic to treat another infection may upset this balance. In this case, the antibiotic kills the bacteria that normally protects and balances the yeast in the vagina. In turn, the yeast overgrows, causing an infection. Other factors that can cause imbalance include a weak immune system, pregnancy, and diabetes.
What are the symptoms of a yeast infection?
The following are the most common symptoms of a candida infection:
-
A thick, white, cottage cheese-like vaginal discharge that is watery and usually odorless
-
Itching and redness of the vulva and vagina
-
Pain with urination or sex
The symptoms of a vaginal candida infection may look like other conditions or medical problems. Always consult your health care provider for a diagnosis.
Who is at risk for yeast infections?
Any woman can get a yeast infection. A woman may be at an increased risk if she:
-
Has had a recent course of antibiotics
-
Is pregnant
-
Has diabetes that is not well-controlled
-
Has HIV
-
Is taking an immunosuppressant medicine
-
Is using high-estrogen contraceptives
-
Is undergoing corticosteroid therapy, which weakens the immune system
How is a yeast infection diagnosed?
Your health care provider will review your medical history and do a physical and pelvic exam. He or she may also examine the vaginal discharge with a microscope.
Treatment for yeast infection
Treatment for candida may include:
-
Antifungal vaginal creams and suppositories
-
Vaginal tablets
-
Oral antifungal medicines
What is bacterial vaginosis?
Bacterial vaginosis is the most common cause of vaginal discharge in women of reproductive age. This is caused by an imbalance of bacteria. With bacterial vaginosis, there is a change in the type of bacteria that grows in the vagina.
What are the symptoms of bacterial vaginosis?
These are the most common symptoms for bacterial vaginosis:
-
A homogeneous, thin discharge at times
-
"Fishy" odor
The symptoms of bacterial vaginosis may look like other conditions. Always consult your health care provider for a diagnosis.
Treatment for bacterial vaginosis
Bacterial vaginosis is caused by bacteria; therefore, it is generally treated with antibiotics.
Research Shows Vaginal Microbiota Transplants
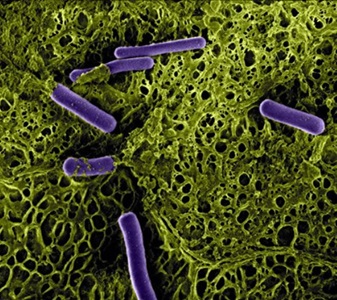
Bacterial vaginosis is a common, often frustrating condition that occurs when the vagina's main bacterial companion, lactobacilli (shown here in purple), is overtaken by competing microbes, leaving patients at higher risk of sexually transmitted infections and preterm births. Researcher Laura Ensign is looking to treat this imbalance by creating vaginal microbiota transplants - moving bacteria from healthy vaginas into patients with BV. The researchers hope that by establishing a way to find healthy donors for transplant, they can help make this treatment available sooner.
What is trichomoniasis?
Trichomoniasis, trichomonas, or "trich" as it is commonly called, is a sexually transmitted infection. It is caused by a one-celled parasite called Trichomonas vaginalis that passes between partners during sex. Since most men do not get symptoms with trichomoniasis, the infection is often not diagnosed until the woman develops symptoms of vaginitis.
What are the symptoms of trichomoniasis?
The following are the most common symptoms of trichomoniasis:
-
A frothy, often musty-smelling, greenish-yellow discharge
-
Itching or burning in and around the vagina and vulva
-
Swelling or redness at the opening of the vagina
-
Light bleeding, especially after sex
-
Burning during urination
-
Discomfort in the lower abdomen
-
Pain during sex
Some women with trichomoniasis have no symptoms. The symptoms of trichomoniasis may look like other conditions or medical problems. Always consult your health care provider for a diagnosis.
Treatment for trichomoniasis
Both partners must be treated for trichomoniasis to avoid reinfection. Treatment generally involves taking oral antibiotics. If a woman has more than one sexual partner, each partner (and any of their other partners) should also be treated.
What is viral vaginitis?
Viruses are a common cause of vaginitis, with most being spread through sexual contact. One type of virus that causes viral vaginitis is the herpes simplex virus (HSV, or simply herpes). The main symptom is pain in the genital area associated with lesions and sores. These sores are generally visible on the vulva, or vagina, but may be found inside the vagina during a pelvic exam. Often stress or emotional situations can be a factor in triggering an outbreak of herpes.
Another source of viral vaginitis is the human papillomavirus (HPV), a virus that is also transmitted through sexual contact. HPV is the main cause of cervical cancer in women. This virus also causes painful warts to grow on the vagina, rectum, vulva, or groin. However, visible warts are not always present, in which case, the virus is generally detected by a test for HPV done with a Pap test.
HPV vaccines are effective in preventing infection by the particular strains of HPV that cause most cervical cancers. New vacciness may be effective against genital warts as well as some cancers of the vulva, vagina, and anus.
7 Things You Should Always Discuss with Your Gynecologist

When it comes to sexual and reproductive health, it can be hard to know what’s “normal” and what may be a sign of a potential health problem. Even if you feel embarrassed about certain issues, your gynecologist has seen and heard it all and is there to help you, not to pass judgment.
What is noninfectious vaginitis?
Noninfectious vaginitis usually refers to vaginal irritation without an infection being present. Most often, this is caused by an allergic reaction to, or irritation from, vaginal sprays, douches, or spermicidal products. It may be also be caused by sensitivity to perfumed soaps, detergents, or fabric softeners.
Another form of noninfectious vaginitis, called atrophic vaginitis, usually results from a decrease in hormones because of menopause, surgical removal of the ovaries, radiation therapy, or even after childbirth--particularly in breastfeeding women. Lack of estrogen dries and thins the vaginal tissue, and may also cause spotting.
What are the symptoms of noninfectious vaginitis?
The following are the most common symptoms of noninfectious vaginitis:
-
Vaginal itching
-
Vaginal burning
-
Vaginal discharge
-
Pelvic pain (particularly during sex)
The symptoms of noninfectious vaginitis may look like other conditions or medical problems. Always consult your health care provider for a diagnosis.
Treatment for noninfectious vaginitis
Treatment for noninfectious vaginitis depends greatly on the cause. If the cause is a reaction to an irritant, the irritant should be avoided.