Stevens-Johnson Syndrome
Featured Expert:
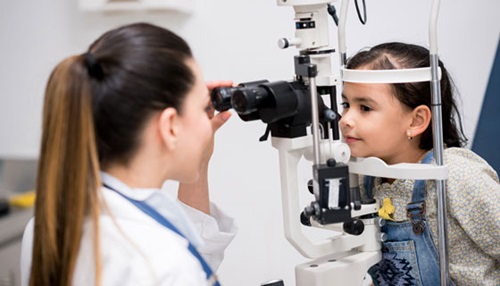
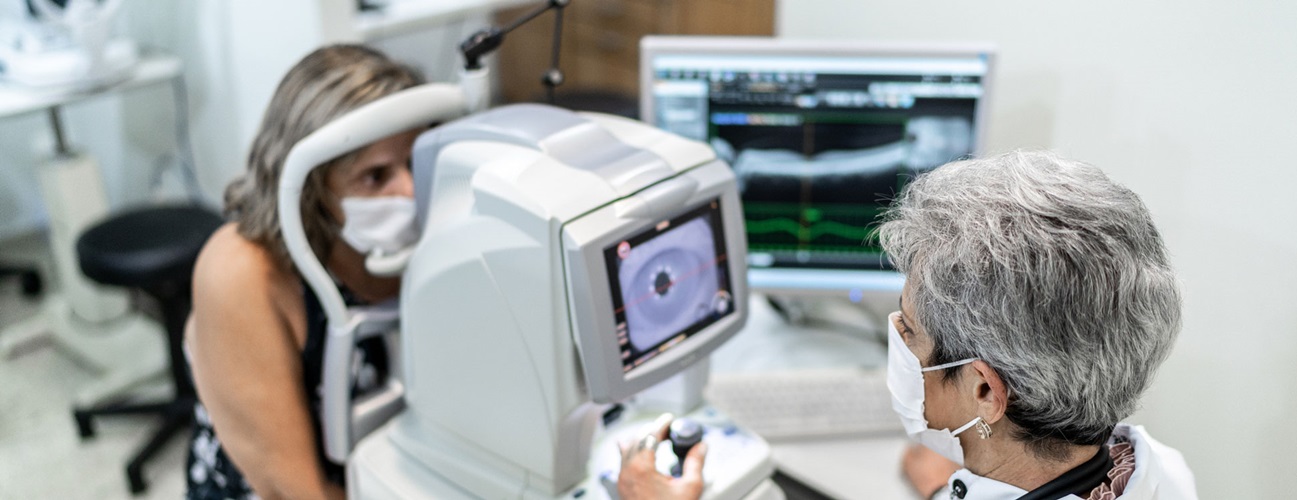
Stevens-Johnson syndrome (SJS) is a disorder that causes painful blisters and lesions on the skin and mucous membranes and can cause severe eye problems.
Who is at risk of developing Stevens-Johnson syndrome?
Some groups of people are at a higher risk of getting Stevens-Johnson syndrome, including:
- People who have experienced certain symptoms after taking specific medications
- Those with a weakened immune system
- Individuals with AIDS or HIV
- People undergoing chemotherapy
- Those who have family members with Stevens-Johnson syndrome
Stevens-Johnson Syndrome Causes
The most common cause of SJS is an adverse drug reaction. Almost any drug can result in SJS, but medicines such as antibiotics, anticonvulsants and anti-inflammatory treatments most frequently cause it. SJS is more common in children and younger adults, but can develop at any age. Typical eye problems associated with SJS can include:
- Conjunctivitis
- Ulceration of the eyelids
- Inflammation inside the eye (iritis)
- Corneal blisters
- Corneal perforation, a hole in the cornea that can lead to permanent vision loss
After the acute stage of the disease, conjunctival and corneal scarring, which lead to decrease or loss of vision, are common.
In children, Stevens-Johnson syndrome can also be caused by infections such as cold or flu, or cold sores.
Stevens-Johnson Syndrome Symptoms
Early stage Steven-Johnson syndrome can include flu-like symptoms, such as fever, sore throat, cough or joint pain. A few days later, a skin rash may appear on any part of the body and may feel like sunburn or lesions. Other symptoms, which appear shortly after the initial issues, may include:
- Blisters on the skin, mouth, eyes, nose and genitals
- Shedding skin after the blisters form
- Unexplained pain on the skin
- Swelling of the mouth, lips, throat, tongue or face
Stevens-Johnson Syndrome Diagnosis
Diagnosis of SJS is made by an ophthalmologist or dermatologist during a thorough medical evaluation that includes a physical exam and review of medication history. A skin biopsy may be performed by a dermatologist for exact diagnosis.
An important element of the early diagnosis is high degree of suspicion by emergency room providers after gathering medication history. The providers will then ask for ophthalmology and dermatology consults. It is important to immediately stop use of medications while the care team determines the cause of the inflammation.
Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis
Occasionally, Stevens-Johnson syndrome can develop into toxic epidermal necrolysis. SJS is when the inflammation affects less than one-tenth of the body surface area. When the lesions cover about one-third or more of the body surface area, it is considered toxic epidermal necrolysis.
Stevens-Johnson Syndrome Treatment
Stevens-Johnson syndrome needs to be treated in the hospital, usually in an intensive care unit. These treatments can include:
- IV fluids to prevent dehydration from skin loss.
- Treatment of affected areas such as blisters on the skin. Cold compress, creams and bandages can help protect the skin, and medications can control inflammation, manage pain and prevent additional infection. Special wound dressing or amniotic membranes may be required for significant cases.
- Intravenous immunoglobulin treatment, or high dose steroids might be helpful at early stages to limit the disease.
- Care for eye inflammation starts by using artificial tears and ointments to lubricate the ocular surface. Steroid drops should be used in patients with significant conjunctival redness and inflammation. Antibiotic drops and ointment are added to regimens in patients with ulcerations, which can be diagnosed through eye examinations. Corneal transplants, limbal stem cell transplantations or artificial corneal procedures may be considered in the later stages of the disease, after the acute inflammation, if advised by an ophthalmologist.
Stevens-Johnson Syndrome Complications
Seeking immediate medical attention for Stevens-Johnson syndrome is important. The reaction can continue during the use of the causative medication and up to two weeks after stopping. In addition, some people may experience complications such as:
- Dehydration: Sores in the throat and mouth may make fluid intake challenging, and areas where the skin has shed tend to lose fluids through evaporation.
- Sepsis: Blood infection or sepsis occurs when bacteria enters the bloodstream from the open sores in the skin and spreads throughout the body. If left untreated, it can cause shock and/or organ failure.
- Eye problems: If the rash from SJS spreads to the eye, it can lead to inflammation, light sensitivity, redness or painful ulcers in the conjunctiva or cornea. In chronic stages, dry eyes and vision impairment due to corneal involvement can occur.
- Respiratory distress: In some cases, Stevens-Johnson syndrome can lead to a situation in which the lungs aren’t able to transport enough oxygen into the blood, leading to wheezing, tightness in the throat or chest, and not being able to breathe or talk.
Frequently, after the skin grows back, scars, bumps or unusual coloring may remain. Some patients may experience loss of hair, or toenails and fingernails not growing as they did before.
Wilmer Eye Institute