Portal Hypertension
Portal hypertension is elevated pressure in your portal venous system. The portal vein is a major vein that leads to the liver. The most common cause of portal hypertension is cirrhosis (scarring) of the liver.
Portal Hypertension Symptoms
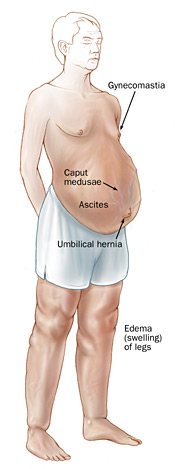
If you have an advanced liver disease, such as cirrhosis, you have an increased risk of developing portal hypertension. Be aware of unusual symptoms and report them to your doctor right away. Symptoms and signs of portal hypertension include:
- Gastrointestinal bleeding: You may notice blood in the stools, or you may vomit blood if any large vessels around your stomach that developed due to portal hypertension rupture.
- Ascites: When fluid accumulates in your abdomen, causing swelling
- Encephalopathy, or confusion and fogginess in thinking
- Jaundice, the yellowing of the skin and the whites of the eyes
- Edema, (swelling) of the legs
- Caput medusa, a visible network of dilated veins surrounding your navel
Portal Hypertension Diagnosis
There are a number of ways to diagnose portal hypertension. For patients with end-stage liver disease who present with ascites and varices, the doctor may not need to perform any diagnostic tests and can confirm a diagnosis based on symptoms.
Diagnostic procedures your doctor may order include:
- Imaging and blood tests
- Pressure measurement studies
- Endoscopic diagnosis
Imaging Studies
An imaging study helps in the diagnosis of cirrhosis and portal hypertension. They are noninvasive and can give your doctor a detailed image of your portal venous system. A duplex Doppler ultrasound is typically the first imaging test ordered. A Doppler ultrasound uses sound waves to see how the blood flows through your portal vein. The ultrasound gives your doctor a picture of the blood vessel and its surrounding organs, as well as the speed and direction of the blood flow through the portal vein.
Pressure Measurement Studies
An interventional radiologist may perform a pressure measurement study to evaluate the level of pressure in the hepatic (liver) vein. This can be done as an outpatient, where a radiologist will access one of your veins, usually via internal jugular vein.
Endoscopic Diagnosis
Endoscopy is another way to diagnose varices, which are large vessels associated with portal hypertension. An endoscopy can provide a definitive diagnosis of the varices and allow your doctor to treat and reduce the risk of bleeding or active bleeding. During a gastrointestinal endoscopy, your doctor can see the mucous lining of the upper gastrointestinal tract, including the esophagus, stomach and duodenum (first part of the small intestine).
During an upper endoscopy:
- You receive an anesthetic to help relax your gag reflex. You will also receive pain medication and a sedative.
- You lie on your left side, referred to as the left lateral position.
- Your doctor inserts the endoscope (a thin, flexible, lighted tube with a camera) through your mouth and pharynx, into the esophagus.
- Your doctor can visualize the esophagus, stomach and duodenum with the endoscope.
Complications of Portal Hypertension
Ascites
Ascites is excess fluid in your abdominal cavity. Patients with chronic liver disease often develop ascites, though it may be caused by other factors. Symptoms of ascites include:
- Early feeling of fullness
- Increase in size of abdomen
- Feeling out of breath (if the fluid begins pushing on your lungs)
You will need to follow a low-sodium diet, as sodium causes fluid retention in your body. In severe cases, you may need to restrict your water intake. A prescription diuretic may help reduce sodium retention in your kidneys.
Sometimes, a large volume paracentesis may be necessary if the ascites is difficult to manage. During a paracentesis, your doctor inserts a needle into your abdomen to remove the fluid.
Varices
Varices are varicose veins associated with portal hypertension. Your doctor can view them during an endoscopy (internal viewing of your gastrointestinal tract) or other imaging study. Varices most often occur in the esophagus or stomach as a result of portal hypertension. This is often because the liver tissue is scarred and blood cannot flow through normally. As the portal blood is rerouted due to the increased resistance, varices develop. In patients with cirrhosis, most often the bleeding is related to esophageal varices, which are enlarged veins in your esophagus. Acute bleeding from varices in patients with portal hypertension requires immediate attention in order to control the bleeding and prevent it from recurring.
Encephalopathy
Hepatic encephalopathy is impairment in neuropsychiatric function associated with portal hypertension. Symptoms are usually mild, with subtle changes in behavior, changes in sleep pattern, mild confusion or slurred speech. However, it can progress to more serious symptoms, including severe lethargy and coma. Although we lack clear understanding of encephalopathy, there is an association with increase in ammonia concentration in the body. (However this does not correlate to regular blood test levels of ammonia).
Hepatic encephalopathy is diagnosed by healthcare providers in clinic. It is usually treated with medications such as lactulose, which can decrease the ammonia absorption in the GI tract. It is also treated with antibiotics, such as rifaximin and neomycin.