Myelopathy
What You Need to Know
- Myelopathy is a disorder that results from severe compression of the spinal cord.
- The only way to treat the compression of the spinal cord is through decompression surgery.
- Causes of myelopathy include spinal stenosis, spinal trauma and spinal infections, as well as autoimmune, oncological, neurological and congenital disorders.
- Myelopathy can be cervical and thoracic; cervical myelopathy is the most prevalent.
- Myelopathy is typically a gradual degenerative process affecting older adults.
What is myelopathy?
Myelopathy is an injury to the spinal cord due to severe compression that may result from trauma, congenital stenosis, degenerative disease or disc herniation. The spinal cord is a group of nerves housed inside the spine that runs almost its entire length. When any portion of the spinal cord becomes compressed or constricted, the resulting symptoms are known as myelopathy.
Myelopathy Versus Myopathy
Myopathy is a muscular disorder and should not be confused with myelopathy, which has to do with nerve damage inside the spinal cord.
Myelopathy Versus Radiculopathy
Myelopathy may sometimes be accompanied by radiculopathy. Radiculopathy is the term used to describe pinching of the nerve roots as they exit the spinal cord or cross the intervertebral disc, rather than the compression of the cord itself (myelopathy).
Types of Myelopathy
Myelopathy can occur in any area of the spine and has a different name depending on where in the spine it appears.
Cervical Myelopathy
Cervical myelopathy occurs in the neck and is the most common form of myelopathy. Neck pain is one of the symptoms of cervical myelopathy, but not all patients experience it.
Thoracic Myelopathy
Thoracic myelopathy occurs in the middle region of the spine. The spinal cord in this area typically gets compressed due to bulging or herniated discs, bone spurs, or spinal trauma.
Lumbar Myelopathy
Lumbar myelopathy is a rare condition because in most people, the spinal cord ends in the top section of the lumbar spine. However, if the spinal cord is low-lying or tethered, it can be affected by lumbar myelopathy.
Causes of Myelopathy
As you age, inflammation, arthritic illness, bone spurs and the flattening of the spinal discs between the vertebrae can put pressure on the spinal cord and the nerve roots. Myelopathy typically develops slowly as result of the gradual degeneration of the spine (spondylosis), but it can also take an acute form or stem from a spine deformity present at birth.
- Common causes of myelopathy are degenerative spinal conditions, such as spinal stenosis, a narrowing of the bony passageways of the spine through which the spinal cord and nerve roots travel.
- Central disc herniations can also result in compression on the spinal cord, leading to the development of myelopathy.
- Autoimmune disorders, such as rheumatoid arthritis in the spine, can also lead to degenerative changes in the vertebrae that result in spinal cord compression and myelopathy.
- Hernias, cysts, hematomas and spinal tumors, including bone cancer, may also press on the spinal cord and lead to myelopathy.
- Acute myelopathy can develop quickly as a result of a spinal injury, spinal infection, inflammatory disease, radiation therapy or neurological disorders.
Below is an example of how a herniated disc may press on the spinal cord, leading to myelopathy.
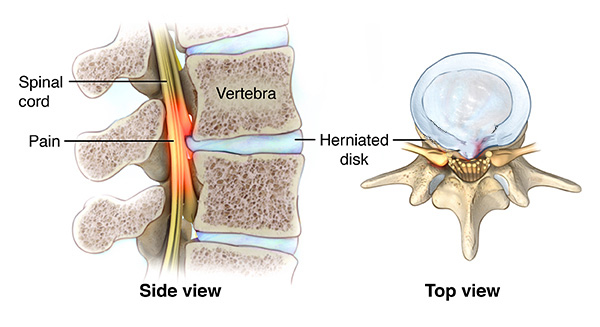
Symptoms of Myelopathy
When the spinal cord is compressed or injured, it may cause a loss of sensation, loss of function, and pain or discomfort in the area at or below the compression point. Myelopathy symptoms may include:
- Neck, arm, leg or lower back pain
- Tingling, numbness or weakness
- Difficulty with fine motor skills, such as writing or buttoning a shirt
- Increased reflexes in extremities or the development of abnormal reflexes
- Difficulty walking
- Loss of urinary or bowel control
- Issues with balance and coordination
The exact symptoms will depend on where in the spine myelopathy is present. For example, cervical myelopathy is likely to have symptoms in the neck and arms.
Myelopathy Diagnosis
Symptoms of myelopathy are not unique to this condition. Your doctor may recommend the following tests to narrow down the myelopathy diagnosis:
- An X-ray to rule out other problems
- An MRI scan for a detailed look of the spine and spinal canal, which can show areas of stenosis
- Myelography uses a contrast material and a real-time form of an X-ray called fluoroscopy to reveal abnormalities of the spinal cord. It is sometimes used instead of MRI for patients who can’t be inside an MRI machine.
- Electrical tests, such as an electromyogram or somatosensory evoked potentials, show how well your nerves are functioning to provide sensation and movement ability to your arms and legs. These tests measure how nerve stimulation in a hand, arm, leg or foot is connecting through the spinal cord to the brain.
The diagnosis itself may be communicated to you by your doctor in several different ways. Sometimes, myelopathy is added at the end of another underlying condition to indicate the involvement of the spinal cord. For example, your doctor may tell you that you have cervical stenosis with myelopathy or thoracic disc disorder with myelopathy. Similarly, if the spinal cord is not involved, your diagnosis may say without myelopathy, as in displaced lumbar intervertebral disc without myelopathy.
If myelopathy is a complication of another disease, your doctor may refer to it in the terms of this disease. For example, diabetic myelopathy means that the spinal cord has been damaged due to diabetes. Carcinomatous myelopathy means that the spinal cord has suffered damage due to a carcinoma.
Myelopathy Treatment
Myelopathy treatment depends on the causes of myelopathy. However, in some cases, the cause may be irreversible, so the treatment may only go as far as helping you relieve the symptoms or slowing down further progression of this disorder.
Nonsurgical Myelopathy Treatment
Nonsurgical treatment for myelopathy may include bracing, physical therapy and medication. These treatments can be used for mild myelopathy and are aimed at reducing pain and helping you return to your daily activities.
Nonsurgical treatment does not remove the compression. Your symptoms will progress — usually gradually, but sometimes acutely, in some instances. If you notice progression of your symptoms, talk to your doctor as soon as possible. Some of the progression can be irreversible even with treatment, which is why it’s important to stop any progression when identified in the mild stages.
Surgical Myelopathy Treatment
Spinal decompression surgery is a common treatment for myelopathy to relieve pressure on the spinal cord. A surgery can also be used to remove bone spurs or herniated discs if they are found to be the cause of myelopathy.
For advanced myelopathy caused by stenosis, your doctor may recommend a surgical procedure to increase the channel space of your spinal cord (laminoplasty). This is a motion-sparing procedure, which means your spinal cord retains flexibility at the site of the compression. For various reasons, some patients may not be candidates for a laminopasty. An alternative is decompression and spinal fusion that can be done anteriorly (from the front) or posteriorly (from the back). During spinal fusion, vertebrae are fused to eliminate motion in the affected segment of the spine.
Minimally invasive spine surgery may offer relief with a lower risk for complications and a potentially faster recovery than conventional open surgery procedures.
While you’re awaiting surgery, a combination of exercise, lifestyle changes, hot and cold treatments, injections, or oral medication can help you control any pain symptoms. It’s very important to take any medications exactly as your doctor prescribes them, since many pain medicines and muscle relaxers can cause side effects, especially when used for a long time.