Intestinal Polyps
What is an intestinal polyp?
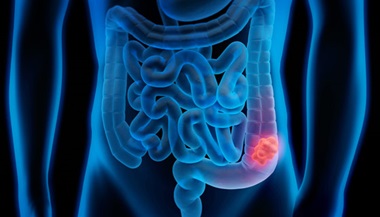
A colorectal polyp is a growth that sticks out of the lining of the colon or rectum. There may be single or multiple polyps. Polyps greater than 1 cm have a greater cancer risk associated with them than smaller polyps. Risk factors include a family history of polyps or colon cancer.
Polyps may also be associated with some hereditary disorders, including:
-
Gardner's syndrome
-
Peutz-Jeghers syndrome
-
Juvenile polyposis
-
Lynch syndrome (hereditary nonpolyposis colorectal cancer, or HNPCC)
Symptoms
Colonic polyps in children most commonly present with rectal bleeding.
Diagnosis
A rectal examination may reveal a polyp that can be felt by the physician. However, the physical exam is usually normal.
Tests that show polyps:
-
Sigmoidoscopy: an internal examination of the lower large bowel (colon), using an instrument called a sigmoidoscope
-
Colonoscopy: an internal examination of the colon (large intestine), using an instrument called a colonoscope
Treatment
Small polyps can be removed with an electrocautery snare passed through a rigid or flexible sigmoidoscope but since total colonoscopy is usually recommended in all patients who have a polyp, it is best to wait and do the polypectomy in a well-prepared colon during that procedure.
Large, fixed, soft, velvety lesions in the rectum are usually villous adenomas. These tumors have a high potential of being malignant and must be excised completely. With the patient anesthetized, this can be accomplished in most instances through the anus.
Pedunculated polyps (those with stalks) and small sessile (non-stalked) lesions in the sigmoid and above should be removed with biopsy forceps or an electrocautery snare passed through the colonoscope.
Depending on your medical history, age and risk factors, your physician will recommend how often to screen for colon cancer, including how often you should perform the fecal occult blood test and how frequently you should have a flexible sigmoidoscopy, colonoscopy or other tests performed.