How to Tell If You Have a Hernia
Reviewed By:
Wondering if the aching in your belly or groin could be a hernia? Hernias are common in both men and women, but symptoms vary. Groin hernias are much less common in women. Hernias may cause some form of discomfort and don’t go away on their own, says Gina Adrales, M.D., M.P.H., director of the Division of Minimally Invasive Surgery at Johns Hopkins Medicine.
The good news? Nearly all hernias can be surgically repaired. Adrales explains how to recognize hernia signs in men and women, the most common types, and what surgery and recovery are like.
Q: What is a hernia?
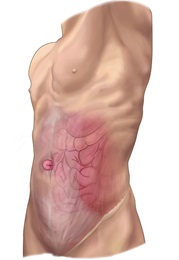
A: Your abdomen is covered in layers of muscle and strong tissue that help you move and protect internal organs. A hernia is a gap in this muscular wall that allows the contents inside the abdomen to protrude outward. There are different types of hernias, but the most common hernias occur in the belly or groin areas.
Q: What Does a Belly or Abdominal (Ventral) Hernia Feel Like?
A: If you have a ventral hernia in the belly area, you may see or feel a bulge along the outer surface of the abdomen. Typically, patients with ventral hernias describe mild pain, aching or a pressure sensation at the site of the hernia. The discomfort worsens with any activity that puts a strain on the abdomen, such as heavy lifting, running or bearing down during bowel movements. Some patients have a bulge but do not have discomfort.
Q: Who is at higher risk for a ventral hernia?
A: Anyone can develop a ventral hernia, but those who’ve had abdominal surgery have a higher risk. If you have an incision that disrupts the abdominal wall, the scar will never be as strong as the original tissue. This makes it more likely that you’ll develop a hernia, known as an incisional hernia, along the incision area. This occurs in up to 30% of patients who have open abdominal surgery.
Pregnancy is a risk factor that makes women more susceptible to developing another type of ventral hernia near the belly button, called an umbilical hernia. The umbilicus is the thinnest part of the abdominal wall. It’s a very common site to develop a hernia, whether you’re a man or a woman.
Q: How can you tell if you have an inguinal (groin) hernia?
A: First, it’s important to understand that both men and women can develop inguinal hernias. People often believe that only men get them, and for anatomical reasons, they do have a higher risk. But women can certainly have inguinal hernias, too.
Many experts agree that women are likely underdiagnosed for this condition because they tend to have different symptoms than men. Women may not have a noticeable bulge. If symptoms indicate a possible hernia but your doctor cannot confirm it by an exam, an MRI can provide definitive evidence.
Symptoms in Men
- A bulge you can see or feel
- Aching pain in the area
- A feeling of pressure
- A tugging sensation of the scrotum around the testicles
- Pain that worsens with activities that add pressure to the area, such as heavy lifting, pushing and straining
Symptoms in Women
- Aching or sharp pain
- Burning sensation
- A bulge at the hernia site, but this may not be present with a groin hernia
- Discomfort that increases with activity
Q: How are hernias treated?
A: Treatment varies depending on the type of hernia, symptoms and the patient's sex.
Inguinal (Groin) Hernias
Inguinal hernias in women are more likely to become emergencies. Women also have a greater chance of developing complications than in men. So, we typically recommend surgical repair after diagnosis.
Men with inguinal hernias often may put off surgery if they’re not symptomatic. Studies of men with inguinal hernias indicate the risk of having an emergency, like part of the bowel getting stuck or strangled in the muscle gap, is quite low. But because hernias tend to grow larger or cause symptoms over time, most men will require surgery within 10 years of hernia diagnosis.
There are two surgical treatments for inguinal hernias. Minimally invasive surgery is often performed laparoscopically, requiring only keyhole-size incisions through which a tiny camera and instruments can be inserted to make repairs. Minimally invasive robotic surgery (similar to laparoscopy, but surgeons use a controller to move instruments) is also an option. With minimally invasive surgery, patients are back to their regular activity within two weeks. Open surgery is the other treatment option — recovery takes four to six weeks.
Abdominal Hernias
For both men and women, repair is recommended for most abdominal hernias. The exception is if you have risk factors for complications or hernia recurrence, such as obesity or poorly controlled diabetes. It’s better to get those conditions under control before surgery. Some patients do not have symptoms and may decide to delay repair after discussion of the risks and benefits with their surgeon.
Surgical options and recovery time for ventral hernias vary widely because these hernias come in all shapes and sizes. A small umbilical or incisional hernia can often be treated on an outpatient basis. However, repairing more complicated hernias may require a hospital stay of one to five days.
Q: What are the signs of a hernia emergency?
A: When most hernias start, the internal tissue that pushes through the muscle gap is usually fat. But it’s also possible for part of the bowel to protrude through the opening. The risk of this is very low, but when it happens, it needs emergency repair. Seek immediate medical attention if you have:
- A painful bulge that doesn’t reduce in size when you lay down and rest
- Worsening pain
- Nausea and/or vomiting
- Difficulty having a bowel movement
- Bloating
- Racing heart rate
- Fever
For more information about hernias and their treatment, visit the Johns Hopkins Comprehensive Hernia Center.