Patient Story
Type 1 Diabetes: Simon's Story
Patient Story Highlights
- With the care and several helpful classes offered by Johns Hopkins All Children’s Hospital, Simon is learning how to manage his Type 1 diabetes.
- Simon’s positivity and his goofy sense of humor—along with a caring family—are definitely working in his favor.
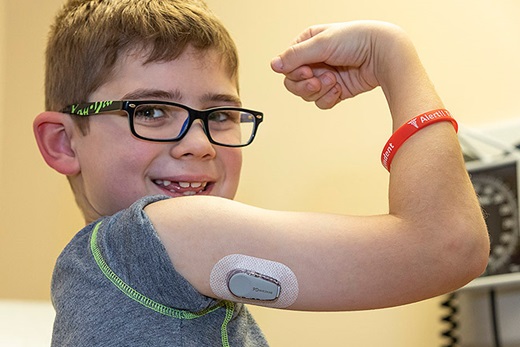
The first thing you need to know about Simon is he’s a character.
Nothing gets this 8-year-old down. He was diagnosed with type 1 diabetes on Halloween, the best candy day of the year. But he took it in stride.
“Aladdin took my blood and Elastigirl from The Incredibles put in my IV,” he recalls of the Johns Hopkins All Children’s Emergency Center costume vibe on Halloween.
“It was weird being there on Halloween,” his dad, Andrew, agrees before recounting the tale of how they got here. “We were doing Trunk-or-Treat with our church where you go from car to car in the parking lot getting candy, and Simon wasn’t doing very well.”
The family of eight had dressed as a bowl of fruit, and Simon was the sunny orange. But he didn’t act like it. “He wasn’t eating much candy, but he was drinking water constantly and kept asking to use the bathroom.” Andrew and Christine, Simon’s mom, weren’t sure how seriously to take it.
“You know, Simon is the fourth of six kids, and I hate to say it, but by the time you reach number four, you’re kind of like, ‘OK, the arm didn’t fall off, I guess you’ll survive,’” Andrew says, joking. But when Simon kept begging them to stop the car on the way home so he could go to the bathroom, they figured this might be serious.
Christine says a thought just popped into her head out of nowhere. “I don’t know what made me say it, but I said, ‘We should check his blood sugar.’ Andrew’s dad has a glucose meter, so Andrew drove across town at about 10 p.m. to pick it up.”
The results said, “High.” They weren’t sure what that meant. They did it again. “High.” They called Andrew’s dad who said the meter only reads up to 500. Anything over that, is off the charts so it reads, “High.” Normal blood sugar levels are 65-100 milligrams per deciliter (mg/dL).
The family immediately called their pediatrician at home. He said calmly, “Pack your bags for two days and take him to Johns Hopkins All Children’s right now,” Andrew recalls. They called family to watch the other kids and drove Simon to the Emergency Center.
“My numbers were dramastically high,” Simon recalls. On beat, Andrew cuts in, “That’s not a word, buddy.” “It is now,” Simon adds and you imagine canned laughter finishing this comedy routine off like a sitcom.
“We already figured we were dealing with diabetes, and we knew it must be serious when they had him hooked up to an IV to flush his system of glucose barely five minutes after we walked in,” Christine recalls.
Simon wasted no time getting to know everyone and cracking jokes. “Because I was so brave, this guy named Chris—[dressed as] Mike from Monsters, Inc.—gave me a plush toy. I had so much fun with that,” Simon explains. The nerf basketball ended up getting tossed around for quite a while as they awaited results. Simon was admitted to a room for further testing and the family officially became regular customers at Johns Hopkins All Children’s.
“We’ve had two other kids come to the hospital in the past. In fact, Dr. Phillips operated on my daughter Gwendallyn’s hand after she cut it on a seashell at the beach,” Andrew recalls of Lee Phillips, M.D., a pediatric orthopaedic surgeon who repaired her tendons. “He’s now on our Christmas card list. We love him,” Andrew laughs. Their son, Ian, was also seen in the urology program. But Simon was their first inpatient experience.
“Everyone was wonderful,” Christine adds. “We even had a volunteer stop by the room and gave Simon some cars to play with. And his nurses took such good care with him. We really appreciated it.”
The family was visited by a nurse educator who spent an hour or so explaining the basics for Simon’s care to get them through the first few days until they could attend classes offered by the hospital to teach them things like, injecting insulin and how to use the Dexcom Continuous Glucose Monitoring system, which means limited finger pricking. That’s huge for an 8-year-old.
“Simon’s blood has to be checked 8 to 10 times a day so that’s a lot of finger sticks he gets to avoid,” explains Simon’s nurse practitioner, Kevin Lewis, D.N.P., APRN, PPCNP-BC, C.D.E. “The meter means one stick every 10 days and the meter can be read on a smart phone in real time. Simon’s parents can even monitor his blood sugar from their smart phone when he’s away in class or at church. That’s only been available for the last six months or so, but it’s wonderful technology. The prick tests are often more painful than the injection, so we love that these kids can now avoid it.”
Lewis is leading research on prevention of adrenal crisis in kids with adrenal insufficiency. Endocrinology also is doing research on type 2 diabetes and plans to soon start several clinical trials, in addition to helping patients like Simon avoid needles.
“I’d tell other kids, insulin shots don’t hurt that much, because the needle is so small. It’s like spaghetti,” he shares. “No,” laughs his dad. “Spaghetti would be huge. It’s smaller than a human hair, actually. You must be hungry.”
At their next visit, the hospital’s photographer stopped by to take Simon’s picture and Andrew recalls, “He said, OK, he’d do it because it might help other kids not be so scared when they are in the hospital. He’s just that kind of kid.” Simon is also endlessly entertaining. He has amassed a few one-liners that he doles out with just the right timing. “I’m handling diabetes like a champ,” Simon says, completely serious. Then: “I want a T-shirt that says, ‘Proud Owner of a Useless Pancreas.’” To the photographer he explains that he’s working on his autobiography, My Life with a Non-functioning Pancreas.
The jokes keep coming. “I want to be a doctor when I grow up, but I’m going to be a lot of things. I also want to be a construction worker, and on Sundays I’m going to be a pastor—so I guess I’ll be a construction worker on Saturdays.” Apparently, he’s still thinking it through.
Meanwhile, thanks to his care and several helpful classes offered by the hospital on how to succeed with pediatric type 1 diabetes, Simon has stabilized. He is learning how to read his glucose meter and paying attention to signals his body sends him. He even teases his siblings about getting a little extra candy when his blood sugar is low.
“We want him to focus on being 8,” Andrew explains. “We know he has to take diabetes seriously, but we don’t want it to define him. It’s important to us that he keeps it all in perspective.”
Simon’s positivity and his goofy sense of humor—along with a caring family—are definitely working in his favor.




