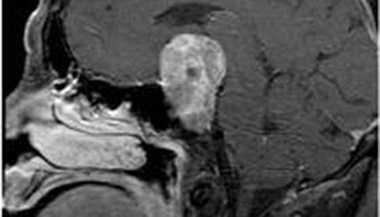
Craniopharyngioma
What You Need to Know Craniopharyngioma
- Craniopharyngiomas are benign tumors that grow near the pituitary gland. They can develop as solid tumors or cysts (hollow sacs filled with fluid).
- Approximately 10 percent to 15 percent of pituitary tumors are craniopharyngiomas. In addition, this type of tumor accounts for about 6 percent of all brain tumors in children.
- Craniopharyngiomas are most commonly found in children between the ages of 5 and 14. However, adults over age 50 can also develop these tumors.
Craniopharyngioma Symptoms
A growing craniopharyngioma can put pressure on the nerves, blood vessels or brain tissue near the pituitary gland, resulting in symptoms such as:
-
Balance problems
-
Confusion, mood swings or behavior changes
-
Headache
-
Increased thirst and urination
-
Nausea and vomiting
-
Slow growth in children
-
Vision problems
Craniopharyngioma Diagnosis
At present, there are no known causes or proven risk factors for craniopharyngioma.
Blood and urine tests can indicate a hormone imbalance that may be caused by a problem with the pituitary gland.
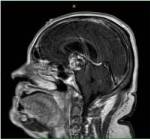
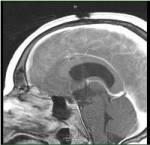
If your doctor suspects a craniopharyngioma, he or she may recommend an MRI or a CT scan of the area surrounding the pituitary gland. These tests can provide a detailed image of the brain and pituitary gland and help distinguish a craniopharyngioma from other pituitary tumors.
If your doctor recommends a biopsy, the tumor may be diagnosed and removed at the same time.
Craniopharyngioma Treatment
Your neurosurgeon and endocrinologist (hormone disorder specialist) will work together to develop the optimal treatment plan for you. Treatment for a craniopharyngioma (or other brain tumor) may include the surgical removal of the tumor through a procedure called a craniotomy.
Orbitozygomatic Craniotomy
The orbitozygomatic craniotomy is a traditional surgical approach used to access the skull base in order to treat difficult tumors and aneurysms. It is based on the concept that it is safer to remove extra bone than to unnecessarily manipulate the brain.
To remove the craniopharyngioma using this technique, the neurosurgeon makes an incision in the scalp behind the hairline and removes the bone that forms the contour of the orbit and cheek. Temporarily removing this bone allows the surgeon to access areas of the brain that are more difficult to reach while minimizing severe damage to the brain. The surgeon replaces the bone at the end of the procedure.
After surgery, your physician team may also recommend hormone replacement therapy and/or stereotactic radiosurgery.
The Johns Hopkins Proton Therapy Center
Proton therapy is used to treat certain tumors in children and adults. Our treatment center, located at Sibley Memorial Hospital in Washington, D.C., combines advanced proton therapy technology, the latest research and caring specialists.