Amyloidosis
What is amyloidosis?
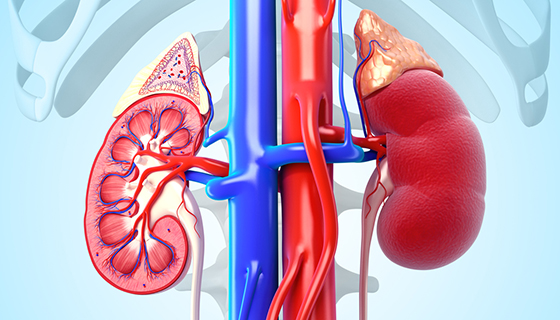
Amyloidosis is a rare disease characterized by a buildup of abnormal amyloid deposits in the body. Amyloid deposits can build up in the heart, brain, kidneys, spleen and other parts of the body. A person may have amyloidosis in one organ or several.
What You Need to Know
- Almost 70 percent of people with amyloidosis are men.
- Some forms of amyloidosis are more likely to strike people living with infections or other conditions that cause chronic inflammation.
- People receiving long-term kidney dialysis are at risk for developing one type of amyloidosis, but modern dialysis techniques are making this less likely.
- Amyloidosis can exist on its own, or it can be related to another problem.
- There are different types of amyloidosis, and some are hereditary.
What causes amyloidosis?
Amyloidosis may be secondary to a different health condition or can develop as a primary condition. Sometimes it is due to a mutation in a gene, but other times the cause of amyloidosis remains unknown.
Types of Amyloidosis
Light-chain (AL) amyloidosis can affect the kidneys, spleen, heart, and other organs. People with conditions such as multiple myeloma or a bone marrow illness called Wadenström’s macroglobulinemia are more likely to have AL amyloidosis.
AL starts in plasma cells within the bone marrow. Plasma cells create antibodies with both heavy chain and light chain proteins. If the plasma cells undergo abnormal changes, they produce excess light chain proteins that can end up in the bloodstream. These damaged protein bits can accumulate in the body’s tissues and damage vital organs such as the heart.
AA amyloidosis is caused by fragments of amyloid A protein, and affects the kidneys in about 80 percent of cases. It can complicate chronic diseases characterized by inflammation, such as rheumatoid arthritis (RA) or inflammatory bowel disease (IBS).
Transthyretin amyloidosis (ATTR) can be inherited from a family member (familial amyloidosis). People of African descent may be more likely to carry the gene that causes this kind of amyloidosis. Transthyretin is a protein that is also known as prealbumin. It is made in the liver. Excessive normal (wild-type ATTR) or mutant transthyretin can cause amyloid deposits.
There are other forms of amyloidosis, including APOA1, gelsolin, fibrinogen, and lysozyme.
Amyloidosis Symptoms
Signs and symptoms of amyloidosis include:
- Feeling very weak or tired
- Losing weight without trying
- Swelling in the belly, legs, ankles or feet
- Numbness, pain or tingling in hands or feet
- Skin that bruises easily
- Purple spots (purpura) or bruised-looking areas of skin around the eyes
- Bleeding more than usual after an injury
- Increased tongue size
- Shortness of breath
As amyloidosis progresses, the deposits of amyloid can harm the heart, liver, spleen, kidneys, digestive tract, brain or nerves.
Kidney problems can result in too much protein in the urine. If amyloid deposits block the filters in the kidney, you may experience swelling or even kidney failure.
Amyloidosis Diagnosis
To see if you have amyloidosis, your doctor will likely order tests. A urine test and a blood test may be followed by one or more imaging procedures to take a look at your body’s internal organs, such as an echocardiogram , nuclear heart test or liver ultrasound . A genetic test may be necessary to see if you have the familial form of amyloidosis.
You might undergo a biopsy, where the doctor takes a small sample of your bone marrow or another organ to examine under the microscope.
Amyloidosis Treatment
The goals of amyloidosis treatment are to slow the progression, reduce the impact of symptoms, and prolong life. The actual therapy depends on which form of amyloidosis you have. Your doctor may discuss:
Chemotherapy : Some medicines used to kill cancer cells or stop them from growing can also stop the growth of cells that are making the abnormal protein in people with AL amyloidosis.
Bone marrow transplant : Also called a “stem cell transplant,” this procedure uses healthy stem cells from your own body. The stem cells are removed from your blood, and then you get chemotherapy to kill the abnormal cells in your bone marrow. Afterward, the stem cells are infused back into your body where they travel to the bone marrow and replace the unhealthy cells destroyed by the chemotherapy. If you have AL amyloidosis, your doctor may discuss this treatment with you.
Medications: The FDA recently approved multiple medications for transthyretin amyloidosis. These medicines work by either “silencing” the TTR gene or by stabilizing the TTR protein. As a result, further amyloid plaque should not deposit in the organs. Which medication you are eligible for will depend on your symptoms and whether or not you have the hereditary form of TTR amyloidosis.
Clinical trial : Your doctor or nurse may be able to provide you with information on research studies that use volunteers to test new medicines and procedures.
Your doctor may continue to test you to ensure that abnormal protein levels in your body have declined, and check the function of your body organs.
Amyloidosis Complications: Amyloid Neuropathy
Disorders of peripheral nerves are the most common neurological complications of systemic amyloidosis. Amyloidosis can affect peripheral sensory, motor or autonomic nerves, and deposition of amyloid leads to degeneration and dysfunction in these nerves.
Common symptoms of amyloid neuropathy are due to sensory and autonomic dysfunction and include:
-
Painful paresthesia (unusual sensations)
-
Numbness and balance difficulties
-
Persistent nausea and vomiting
-
Diarrhea, constipation and incontinence
-
Sweating abnormalities
-
Sexual dysfunction
Diagnosis of amyloid neuropathies is based on medical history, clinical examination and laboratory tests. These tests include electromyography with nerve conduction studies, skin biopsies to evaluate cutaneous nerve innervation, and nerve and muscle biopsies for histopathological evaluation. In cases of familial amyloidosis, genetic testing may be useful.
Treatment of amyloid neuropathies is directed at both preventing further deposition of amyloid in peripheral nerves and treating painful symptoms. Depending on the type of amyloid protein, patients may benefit from liver or bone marrow transplant. Nerve pain due to amyloid neuropathy can be treated with anti-seizure medications, antidepressants, or analgesics.