Achondroplasia
What You Need to Know
- Achondroplasia is the most common form of skeletal dysplasia, occurring in about one in every 40,000 births.
- Achondroplasia impairs the growth of bone in the limbs and causes abnormal growth in the spine and skull.
- Although the cause is a genetic mutation, only about one out of five cases is hereditary (passed down by a parent).
What is achondroplasia?
Achondroplasia is a genetic condition affecting a protein in the body called the fibroblast growth factor receptor. In achondroplasia, this protein begins to function abnormally, slowing down the growth of bone in the cartilage of the growth plate. This leads to shorter bones, abnormally-shaped bones and shorter stature; adult height in people with achondroplasia is between 42 and 56 inches.
In addition, 20 to 50 percent of children born with the condition will experience neurological impairment.
Risk Factors for Achondroplasia
The genetic defect can be passed from parent to child. However, in about 80 percent of cases, achondroplasia results from a spontaneous mutation (a sudden genetic defect) that occurs in the developing embryo.
Achondroplasia Symptoms
The following are the most common symptoms of achondroplasia; however, each child may experience the condition differently:
- Shortened arms and legs, with the upper arms and thighs more affected than the forearms and lower legs
- Large head size with a prominent forehead and a flattened nasal bridge
- Crowded or misaligned teeth
- Curved lower spine, a condition also called lordosis (or sway-back) which may lead to kyphosis, or the development of a small hump near the shoulders that usually goes away after the child begins walking
- Small vertebral canals that may lead to spinal cord compression in adolescence
- Bowed lower legs
- Flat feet that are short and broad
- Extra space between the middle and ring fingers (also called a trident hand)
- Poor muscle tone and loose joints
- Frequent middle ear infections that may lead to hearing loss
- Delayed developmental milestones — for instance, walking may occur between 18 to 24 months of age instead of around 12 months
The symptoms of achondroplasia may resemble other problems or medical conditions. Always consult a physician for a diagnosis.
Achondroplasia Diagnosis
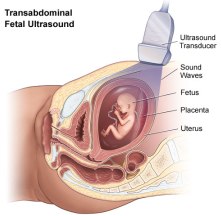
Achondroplasia can be diagnosed before birth by fetal ultrasound or after birth by complete medical history and physical examination.
DNA testing is now available before birth to confirm fetal ultrasound findings for parents who are at increased risk of having a child with achondroplasia.
Neurologic Problems in Achondroplasia
Neurological impairment is caused by compression created as children grow faster than their bones. Arrested bone growth at the base of the skull and the spine can cause the spinal cord and brain stem to become compressed.
This can compress key nervous system structures, like the brain stem, spinal cord, spinal nerve roots and cerebrospinal fluid (CSF) spaces. Eventually, this may lead to neurological deficits, including:
Cervicomedullary Myelopathy
Compression at the foramen magnum — the bony hole at the base of the skull through which the brainstem and spinal cord exit the skull — can cause a child’s brainstem to “kink,” resulting in:
- Very brisk reflexes
- Numbness
- Weakness
- Increased irritability
- Poor feeding
- Difficulty walking
- Loss of bowel and bladder control
- Sleep apnea (periods during sleep when the child stops breathing)
Brainstem compression can ultimately lead to death if it is left untreated, so parents and physicians of children with achondroplasia should watch for these symptoms.
If any of these occur, your child should be seen by a pediatric neurologist, pediatric neurosurgeon or pediatric orthopaedist, who might recommend MRI scans of your child’s head, neck or spine.
Hydrocephalus
When the narrowing near the base of the spine prevents CSF from flowing freely around the brainstem or in and out of the skull, the CSF collects in ventricles (spaces in the brain). The resulting condition is hydrocephalus. In babies, the most evident symptom of hydrocephalus is a quickly enlarging head circumference. Additional symptoms include:
- Headaches
- Irritability
- Lethargy
- Vomiting
Because an enlarged head is normal in children with achondroplasia, pediatricians can use a special head circumference growth chart to distinguish between normal growth and possible hydrocephalus.
Spinal Cord Myelopathy
Sometimes the vertebrae of children with achondroplasia do not grow enough to allow sufficient space for nerves exiting and entering the spinal cord to pass in and out of the bony spinal column.
If only a single nerve root is compressed, children may experience pain, numbness or weakness in a specific arm or leg. They may seem to prefer using one hand over another very early as babies, or complain of pain in their back or affected arm.
In more severe cases, the entire spinal cord can be compressed, causing weakness and numbness in the entire body below the spinal cord pinch, as well as a loss of bowel and bladder control.
Achondroplasia Treatment
Infants should be monitored closely for the first two years of life and then followed every one to two years, to be evaluated for complications.
In providing care for children with achondroplasia, doctors will periodically take X-rays to monitor the position of the spine and lower extremities. MRI scans of the brain and spine help doctors spot development of spinal stenosis, and CT scans are occasionally ordered to visualize the vertebrae in the spine.
Treatment for spinal stenosis might include decompression and fusion. Treatment for lower extremity misalignment might include surgery to correct the limbs.
If a dangerously compressed region of the foramen magnum or spinal column is found, a surgeon can remove bone and ligaments from the problem area to make more room for the brain’s and spine’s structures.
The structural integrity of the neck and spinal column are not compromised in these procedures, and patients tend to do very well. Because children are continuing to grow, they may require additional decompressions. Surgical decompression is most successful when performed quickly, since compression problems can become permanent over months or years if untreated.
A child with achondroplasia who has developed hydrocephalus may require a ventriculoperitoneal shunt. In this case, a pediatric neurosurgeon can relieve the accumulation of CSF in the child’s brain ventricles by placing a long, thin tube under the skin. One end is placed in the ventricle and the other in the abdomen, allowing CSF to flow at a controlled pace out of the child’s head to where it can be quickly and safely absorbed into the bloodstream.
Prompt identification and modern medical interventions for children with achondroplasia can optimize their chance for a whole and happy life.