POTS: A Little Known Cause of Extreme Fatigue
Featured Expert:
Everyone knows what being tired feels like at the end of a long day. But some people experience fatigue so severe and so seemingly random that it’s hard to describe. If that sounds familiar, there could be more going on than daily stress.
While there are many causes of fatigue, one of them is frequently missed and misdiagnosed: postural orthostatic tachycardia syndrome (POTS). Physical medicine and neuromuscular specialist Tae Chung, M.D., answers questions about POTS and extreme fatigue as one of its symptoms.
When is fatigue considered extreme?
There is no good criteria for assessing the level of fatigue — it depends on the person. However, most people know when their tiredness is more than a lack of sleep. Some of my patients remember the exact day they got hit with fatigue so overwhelming that they knew something was wrong.
Postural Orthostatic Tachycardia Syndrome (POTS)
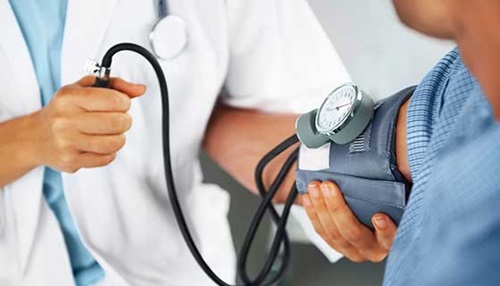
POTS is a common condition affecting an estimated one to three million Americans. Researchers don’t fully understand the causes of POTS, but it is more common in women than men and is more likely to develop in adolescents and young adults.
How would you describe fatigue associated with POTS?
People with POTS experience fatigue differently. Many describe it as feeling beyond exhausted. It’s as if your energy is completely depleted. The fatigue is probably hundreds of times worse than your worst flu. People with POTS may also have trouble concentrating and thinking straight. Doing simple tasks may feel like you’ve just run a marathon.
This fatigue might come and go, hitting you without warning daily, weekly or less frequently. For some people, extreme fatigue lasts for days. Others may experience periodic “attacks.” It can come on at any moment — even if you just woke up. And there is no amount of sleep or coffee that can make it go away.
What is POTS and why does it cause fatigue?
POTS is a group of symptoms resulting from dysfunction of the autonomic nervous system. This branch of the nervous system regulates functions we don’t consciously control like sweating and blood circulation.
In people with POTS, more blood collects in the lower body when standing upright. The heart beats faster to pump it up to the brain, but with little success. The causes of POTS are unknown, but the problem is thought to lie in the communication breakdown between the brain and the cardiovascular system.
POTS-related fatigue is physical in nature and the mechanism behind it is not fully understood. It may have several causes, including your body working harder to move the blood.
What are other symptoms of POTS besides the extreme fatigue?
People with POTS may experience different symptoms to a different extent. These symptoms may include but are not limited to:
- Dizziness when standing
- Nausea and vomiting
- Lightheadedness and fainting
- Brain fog
- Muscle pain and cramps
- Headaches
- Excessive sweating
- Shakiness
Some people feel as though their heart is beating really fast or skipping a beat. This is called heart palpitations.
Is POTS more common in certain people?
There are no established risk factors for POTS. However, it is known to run in families, so it could have a genetic component. Researchers have also established a link between POTS and Ehlers-Danlos Syndrome (highly mobile joints). So if you have one of these conditions, you might also have the other.
A big group of those diagnosed with POTS is young women and teens. However, this doesn’t mean they are more likely to develop this condition.
Is it possible that I have POTS and was incorrectly diagnosed?
This is entirely possible. Given how common POTS symptoms are and how unfamiliar many doctors are with this condition, diagnostic mishaps happen. POTS is frequently misidentified as chronic fatigue syndrome, fibromyalgia, myofascial pain syndrome, anxiety disorder, ADHD, irritable bowel syndrome, myositis, etc. It is also possible that you have both POTS and one of these conditions, which may complicate the diagnosis. Sometimes people with POTS are told that “it’s all in your head,” implying that the cause of their symptoms is psychological. If you feel like something is physically wrong, don’t hesitate to seek a second, and even a third or fourth opinion.
COVID-19 and POTS: Is There a Link?
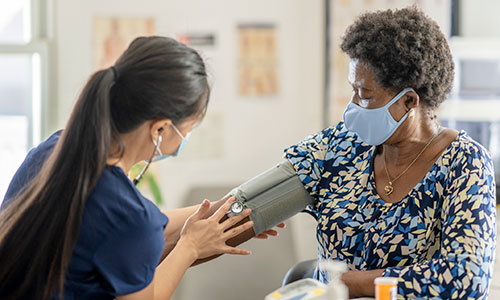
Although many people recover quickly from COVID-19, the disease caused by the coronavirus, others who recover may continue to experience symptoms for months. Researchers are still determining the cause of these extended symptoms, but some COVID-19 "long-haulers" may actually be dealing with POTS.
How is a POTS diagnosis made?
Problems with the autonomic nervous system can be difficult to diagnose. The standard test for POTS is the tilt table test. During the test, you are secured to a table that tilts from being horizontal to almost a 90-degree angle. The test measures your heart’s response to switching from laying down to standing up. Some people with POTS faint during this test, even if they rarely faint standing up.
Although the test seems straightforward, many things can interfere with it. It’s important that a POTS specialist oversees it. It’s best to work with a doctor who has diagnosed and treated patients with POTS. This could be a cardiologist, a neuromuscular specialist or another doctor.
Is POTS treatable?
While there is nothing that can make POTS go away for good, there are ways to address the symptoms. One treatment option is a diet that involves increasing your salt and water intake. This helps your body retain fluids and increase the blood volume.
The other treatment is exercise — even though it may be the last thing on your mind. Pushing through fatigue is difficult, but exercise can help you maintain healthy blood circulation. Exercise should be prescribed and closely monitored by your doctor. It often starts as low-intensity exercise that can be done while you are lying down, and gradually increases as your body is able to tolerate more physical activity, although each person's experience is different.
POTS treatment has to be tailored to address your specific symptoms and underlying conditions. Be wary of trying treatments you find online without consulting with your doctor. A treatment that makes one POTS patient better may make another worse.
Sign Up for Our Free Newsletter

One of the best things you can do to protect and improve your health is to stay informed. Your Health is a FREE e-newsletter that serves as your smart, simple connection to the world-class expertise of Johns Hopkins.





