-
Ahmet Alexander Baschat, M.D., M.B. B.CH. B.A.O.

- Director, Center for Fetal Therapy
- Professor of Gynecology and Obstetrics
- Joint Appointment in Surgery
-
Jena Lyn Miller, M.D.

- Assistant Professor of Gynecology and Obstetrics
- Assistant Professor of Surgery
-
Jamie Deneen Murphy, M.D.

- Director of Obstetric Anesthesia
- Associate Professor of Anesthesiology and Critical Care Medicine
- Associate Professor of Gynecology and Obstetrics
Conditions We Treat: Fetal Anemia
Fetal anemia occurs when the amount of circulating red blood cells and hemoglobin in a fetus fall below normal levels. Because hemoglobin carries oxygen and red blood cells are important in maintaining the normal function of the blood, fetal anemia can have several adverse effects, including cardiac complications. In an effort to maintain oxygen delivery to the tissues, the heart needs to pump the blood faster.
When anemia gets severe, the combination of decreased oxygen-carrying capacity of the blood and blood cells places the fetus at danger of heart failure. If this occurs, there may be fluid accumulation in the body of the fetus. This is called hydrops. If left untreated, anemia can lead to fetal death.
The most common cause for fetal anemia is an incompatibility between the blood type of the mother and the fetus, called isoimmunization. Under these circumstances, antibodies from the mother destroy the red blood cells of the fetus. Viral infections that interfere with the fetal bone marrow to produce red blood cells can also cause fetal anemia.
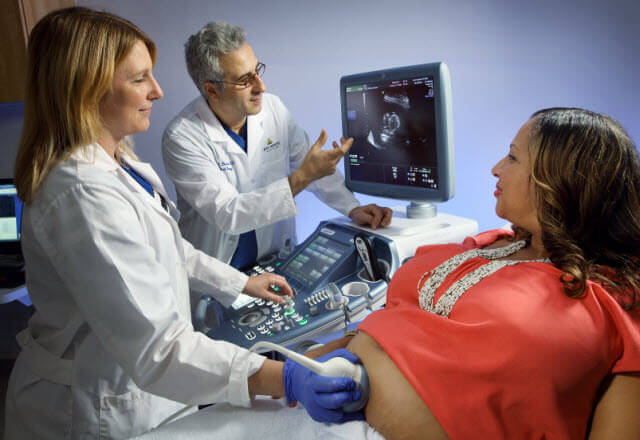
Fetal Anemia: Why Choose Johns Hopkins
- We understand the urgency involved with treating a fetus with a fetal anemia diagnosis. Our care team is available to take your call at any time and will see you as soon as possible.
- After treatment for fetal anemia, our patients will have continued access to the most advanced multidisciplinary care at Johns Hopkins, including our fetal, maternal and pediatric specialties.
- Our care plan also provides options for long-term developmental assessment of infants and children affected by TAPS and TTTS, which can lead to fetal anemia.
- The majority of fetal anemia cases have an excellent outcome.
Patient Resources
Discover how the Tingle family triplets were treated at the Johns Hopkins Center for Fetal Therapy
Our Physicians
Rely on the expertise of our physicians to help you treat fetal anemia.

