Pancreatitis Center
The Johns Hopkins Pancreatitis Center is dedicated to providing the best care to patients with acute and chronic pancreatitis and related problems.
The National Pancreas Foundation has designated the center a Pancreatitis Center of Academic and Clinical Excellence.
-
Team
Our team is skilled in endoscopic procedures as well as minimally invasive pancreatic surgery.

-
Programs and Services
Our treatment approaches are rooted in the latest science and care guidelines.

-
Care Locations
Care is available at several convenient locations.

-
Research and Clinical Trials
We conduct trials of new therapies and diagnostic methods.

Conditions We Treat
- Acute pancreatitis: sudden, painful inflammation of the pancreas
- Necrotizing pancreatitis: a complication of acute pancreatitis due to a lack of blood flow to the pancreas
- Chronic pancreatitis: persistent inflammation of the pancreas resulting in irreversible damage
- Autoimmune pancreatitis: an attack of the pancreas by the immune system
- Hereditary pancreatitis or pancreatitis associated with genetic mutations
- Idiopathic pancreatitis: pancreatitis of unknown origin
- Pancreatic pseudocyst: a fluid-filled sac that forms in the abdomen as a result of pancreatitis and can cause symptoms
- Pancreatic exocrine insufficiency: low levels of pancreatic enzymes, which can have a serious impact on health due to issues regarding digestion, metabolism and nutrition
- Pancreatogenic diabetes: a type of diabetes caused by pancreatitis, pancreatic surgery, cystic fibrosis or pancreatic cancer
- Pancreatic disorders associated with cystic fibrosis
- Pancreatic duct stones
Our Services
Our multispecialty team offers each patient a personalized treatment plan that addresses all symptoms and effects of the disease. Your treatment plan may include:
- Genetic testing and counseling to assess risk for hereditary pancreatitis or help identify gene mutations
- Evaluation for pancreatitis of an unknown cause
- Treatment with rituximab for autoimmune pancreatitis that comes back or is resistant to other treatments
- Shock wave treatment (extracorporeal shock wave lithotripsy) for pancreatic duct stones
- Pancreatic surgery, including total pancreatectomy (pancreas removal) with islet autotransplantation (TPIAT)
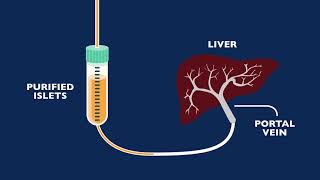
Total Pancreatectomy and Islet Autotransplantation Program (TPAIT)
If you have acute pancreatitis that keeps coming back and that affects your quality of life, or painful chronic pancreatitis that doesn’t improve after other treatments, you may benefit from pancreas removal (pancreatectomy). And to compensate for the missing pancreas, insulin-producing cells in the pancreas (islets) can be transplanted to the liver. This procedure is called total pancreatectomy with islet autotransplantation.
Learn more about this programPancreatitis Research and Clinical Trials
The Pancreatitis Center conducts research to improve understanding of pancreatitis and develop treatments that will improve patients’ lives. Johns Hopkins researchers, working with other institutions in the U.S. and around the world, explore topics such as:
Acute Pancreatitis
- Diabetes related to acute pancreatitis (multicenter National Institutes of Health Study)
- Role of genetics in the risk of pancreatitis complications
- Pancreatic exocrine insufficiency after acute pancreatitis (multicenter study)
- IV medication to treat acute pancreatitis (clinical trial)
- Relationship between gut microbes and development or worsening of pancreatitis
Chronic Pancreatitis
- Treatment of pancreatic exocrine insufficiency
- Understanding the natural history of chronic pancreatitis
- New imaging techniques to diagnose chronic pancreatitis and assess pancreatic function
- Management of pancreatic duct stones (multicenter study)
Autoimmune Pancreatitis
- New monoclonal antibody to treat type 1 autoimmune pancreatitis (clinical trial)
- Imaging to classify patients
Total Pancreatectomy with Islet Autotransplantation
- Use of a patient’s liver cells to produce insulin producing cells after pancreas removal
Pancreatic Pain
- A bedside tool to assess and describe pain in patients with chronic pancreatitis and pancreatic cancer
Clinical Trials
Care Locations
-
Green Spring Station
Lutherville, MD
-
Sibley Memorial Hospital
Washington, DC
Support the Pancreatitis Center
Your donation can help advance pancreatitis research at Johns Hopkins, which hopefully will lead to development of better treatment options and reduction in the costs of care. You can designate your gift to the Pancreatitis Center or a specific physician.