Pediatric Hospital Medicine Fellowship
Program Mission Statement
Our mission is to prepare future pediatric hospitalists to provide exemplary family-centered care, to be leaders and teachers of pediatric hospital medicine, and contribute to research and quality efforts within the field of pediatric inpatient medicine.
Program Aims
- To practice patient centered medicine of the highest standard for medically complex pediatric patients.
- To develop an area of specialized skills in one of four domains: clinical research, advocacy, quality improvement or medical education.
- To inspire trainees to incorporate leadership into their professional identity formation.
Innovative Learning Environment
The Mission of the PHM fellowship program is to train the next generation of leaders in Pediatric Hospital Medicine within an innovative, collaborative, personalized and learner-centric environment. Fellows will develop superior skills in delivering family-engaged patient care through a systems-based model, advocating for safety, quality and value-based care, and in advancing scientific research and investigation.
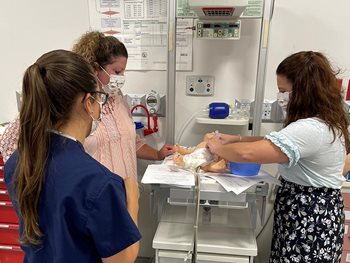
Our simulation center will expose fellows to state-of-the-art simulation experiences with the most advanced technology available for simulation-based learning.
A personalized academic structure will allow the fellow to advance individual learning objectives and develop expertise in a specialized area of interest with the following highlights:
- Individualized learning objectives
-
Weekly “on-the-job” mentorship meetings
- Opportunities to develop expertise in specific areas of individual interest
- Emphasis on active learning and simulation
Research and Investigation
The Johns Hopkins All Children’s PHM fellowship program provides the fellow a range of opportunities to pursue clinical, integrative basic science and translational research, as well as quality improvement and educational scholarship. The program benefits from research collaboration with the Johns Hopkins Medicine campus in Baltimore, Maryland.
Training Opportunities
Fellow scholarship endeavors are supported by the cores and shared resources offered by the Johns Hopkins All Children’s Institute for Clinical and Translational Research (ICTR). Housed within the Research and Education Building, the ICTR strives to engage and support investigators across all levels of experience. Fellows have access to the Center for Pediatric Early-Phase Trials, Clinical Coordinating Center for Pediatric Multicenter Studies, and Data Coordinating Center for Pediatric Multicenter Studies, as well as the shared resources that provide biostatistical and data acquisition support necessary for scholarly activity.
In addition to core research services, we offer two unique resources to fellows. The Program for Pediatric Health Equity Research, led by Dr. Raquel Hernandez M.D., M.P.H., strives to address child health disparities and promotes diverse research efforts to address these disparities across both inpatient and outpatient care settings. Additionally, the Center for Clinical/Translational Research Training, Education, Engagement, and Mentorship (C-TEEM), led by Dr. John Morrison M.D., Ph.D. (PHM fellowship alumni), offers fellows several opportunities to engage with the research organization and serves as a launching pad to assist fellows with taking projects through the research life cycle.
During their training, fellows within our program are provided several opportunities to collaborate with colleagues to develop, execute, and disseminate their scholarly work. The weekly Division of Hospital Medicine Works-in-Progress meetings provide fellows with a platform to receive and provide feedback on projects of all stages while also exposing fellows to a core research and quality improvement methodology curriculum. Fellows also have the opportunity to share their work at the institutional wide Interdisciplinary Research Forum (sponsored by the C-TEEM) and the Pediatric Grand Rounds. Fellows wanting in-depth training in clinical and translational research practices are able to participate in the Clinical and Translational Research Training Track (CTRT), that provides a year-long mentored research experience paired with targeted didactic lectures and offers participants up to $20,000 to fund research-related needs. Additional training in key topics relevant to careers in academia are provide by the monthly Seminar Series in Academia.
Current Research Efforts
The Division of Hospital Medicine prides itself in pursuing a variety of scholarly activities. Faculty are active in grant-funded clinical and translational research relevant to the field of Pediatric Hospital Medicine including: bronchiolitis and other respiratory infections, complex care management, hospital readmissions and sepsis recognition. Additionally, several faculty are active in medical education research including trainee autonomy, simulation-based training, and undergraduate medical education. Supported by the Johns Hopkins Armstrong Institute for Patient Safety and Quality, our pediatric hospitalists have several ongoing quality improvement efforts surrounding sepsis recognition, clinical documentation improvement, care coordination, and addressing unmet social needs. Fellows with interests outside of the aforementioned areas are welcomed and supported to expand their ideas, and are further supported in establishing a team of mentors through the C-TEEM Trainee Mentorship Committee!
Clinical
Johns Hopkins All Children’s Hospital is the primary training site for the PHM fellow. This 259-bed hospital is home to a 56-bed pediatric medicine unit and 28-bed neurosurgery and surgery unit.
Many of the patients on these units are cared for by the hospitalist team, either independently or co-managing with a wide range of surgical and medical subspecialty services.
The fellow will also spend 4 weeks at a community hospital in the Tampa Bay metropolitan area, with the focus in core pediatric hospital medicine skills. 36-40 patients per day are divided amongst three resident teams led by hospitalists.
Rotations at a Glance
Core Clinical Rotations (8 months)
- Hospital Medicine
- Complex Care
- Surgical Co-management
- Critical Care (EM, PICU, NICU, Transport)
- Newborn Care
Systems and Scholarship (8 months)
- Improvement Science
- Clinical and Translational Research
- Medical Education
- Leadership
- Practice Management
- Patient Safety
- Advocacy
Individualized Curriculum (8 months)
- Child Abuse and Neglect
- Additional time in pediatric subspecialties (i.e. Palliative Care, ID, Pulmonology, Nephrology)
- Pain Management
- Transport Medicine
- Emergency Medicine
- Additional time for scholarship and non-clinical electives
- Medical informatics

