Dan Belz, MD MPH

- Co-Director of the Nontuberculosis Mycobacteria and Bronchiectasis Center
- Assistant Professor of Medicine
Expertise: Pulmonology
Established in 2018, the Johns Hopkins Center for Nontuberculous Mycobacteria and Bronchiectasis is dedicated to the specialized care of adult patients with suspected or confirmed nontuberculous mycobacteria (NTM) infection (in the lung or elsewhere) and/or non-cystic fibrosis bronchiectasis. The Center is made up of a multi-disciplinary team of experts with training in pulmonary medicine, infectious diseases and airway clearance techniques. Patients of this Center are able to be seen by pulmonologists, infectious diseases physicians and physical therapists with expertise in airway clearance techniques during the same clinic session.
NTM are a diverse group of environmental bacteria that are found in soil and water. In certain individuals, these bacteria can cause human disease, which most frequently occurs in the form of a chronic lung infection that can be mistaken for tuberculosis. Less commonly, these bacteria can cause skin or soft tissue infections, swollen lymph nodes (glands), or disseminated disease throughout the body. People with underlying lung disease, such as bronchiectasis or COPD, or individuals who are immunosuppressed (such as from HIV, or due to immune suppressing medications such as chemotherapy or TNF-alpha inhibitors), are at increased risk for infections with these bacteria. Unlike tuberculosis, NTM are not thought to pass directly from person-to-person. NTM lung disease is a major challenge for physicians to both diagnose and treat. Testing for these bacteria in the laboratory must be done in a specialized way, and sometimes a minimally invasive procedure called a bronchoscopy is required to identify these bacteria in the lungs. Not all people who harbor NTM will require antibiotic treatment. People who do require treatment are prescribed prolonged courses of combination antibiotic therapy and airway clearance techniques.
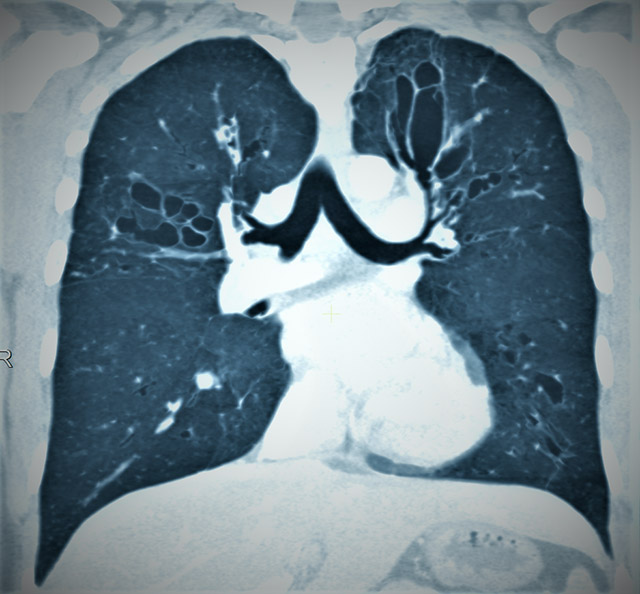
Bronchiectasis is a clinical syndrome of cough, sputum production and recurrent respiratory infections that occurs in the setting of permanent damage to the airways of the lungs. Chest imaging of people with bronchiectasis shows dilated airways, and these damaged airways are not able to clear mucus and infections appropriately. Once structural lung disease and airflow obstruction develop in bronchiectasis, there is a vicious cycle that includes chronic infection and bacterial colonization paired with failure of mucus clearance, which leads to sustained airway inflammation and further tissue damage. There are many medical conditions that are associated with bronchiectasis, including a history of prior lung infections, congenital lung disease and immunodeficiency or rheumatologic problems, among others. Successful care of patients with bronchiectasis includes determining the cause of bronchiectasis, teaching airway clearance techniques and managing both chronic and acute lung infections.
Patients are seen on Fridays from 8:00 AM to 2:00 PM.
Appointments: 410-550-2590
Fax: 410-500-4259
For cystic fibrosis patients, please visit the Johns Hopkins Cystic Fibrosis Center website
Prior to scheduling your first appointment we will request and review your medical records in order to ensure 1) that the Johns Hopkins Center for NTM and Bronchiectasis is the most appropriate clinic for your medical needs, and 2) that we have key information regarding your medical history to date. This comprehensive records review is a critical step to ensure we understand your health care needs, have available the relevant information needed to devise an individualized treatment plan for you, and have a productive initial clinical visit in our Center. As appropriate, this records review will include:
Despite our best efforts to obtain all relevant medical records in advance of your appointment, we may determine that we are still missing some key pieces of information.
If you have any questions regarding our records review process, please call our appointment line at 410-550-5864.
As part of your evaluation in the Johns Hopkins Center for NTM and Bronchiectasis, we may request that your chest imaging be submitted for a second-opinion review by a Johns Hopkins radiologist. Depending on your medical insurance, you may receive a bill for this interpretation. You have the ability to opt out of this service.
If you have any questions regarding the second opinion of chest imaging, please call our appointment line at 410-550-5864.
Our Center operates under a multidisciplinary clinic model. During the same clinic session, you may see multiple providers from different disciplines, such as pulmonary medicine, infectious disease and/or physical therapists who specialize in airway clearance, as appropriate. Additionally, we attempt to schedule ancillary testing, such pulmonary function testing, sputum induction, or chest imaging, to coincide with your appointment date. Accordingly, clinical encounters may be longer than one would expect, thus we recommend allotting an entire morning for your visit to our Center.

Expertise: Pulmonology

Meghan Ramsay, RN, CRNP, CCM
Nurse Practitioner and Clinical Case Manager
Lead Nurse Practitioner, Director of Outpatient Parenteral Antimicrobial Therapy
Expertise, Disease and Conditions: Bronchiectasis, Mycobacterial Lung Disease

Expertise: Infectious Diseases, Hospital Medicine

Expertise: Infectious Diseases
Sera-Kim Huenergard, PT DPT
Fin “Albert” Mears, PT
Renee Vaughnley, PT DPT
Johns Hopkins Bayview Medical Center
Asthma and Allergy Building
Second Floor
5501 Hopkins Bayview Circle
Baltimore, MD 21224