Women Underrepresented in Academic Hospital Medicine Leadership Roles, Study Finds
06/25/2020
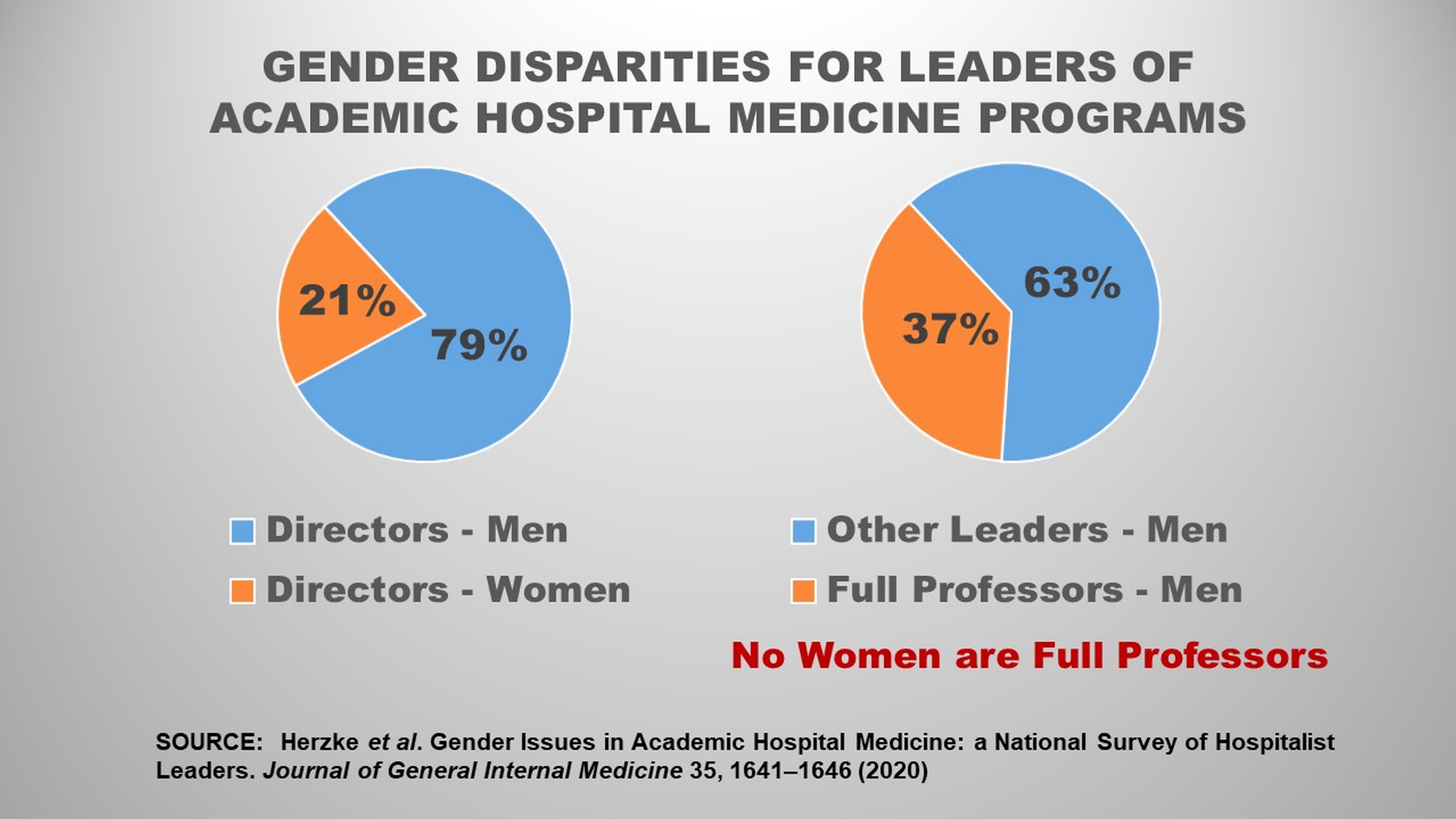
In recent years, the number of women who entered U.S. medical school surpassed the number of men. But gender inequities still exist in many areas of medicine. Of academic hospital medicine programs, 79% are run by men, Johns Hopkins researchers report in a new paper published March 3 in the Journal of General Internal Medicine, and male hospitalist leaders are more likely to have attained the rank of full professor than women leaders.
“Despite making a number of strides in medicine when it comes to gender bias, this is an area where we still haven’t reached full equality,” says Carrie Herzke, M.D., assistant professor of medicine and associate vice chair for clinical affairs in the Department of Medicine at the Johns Hopkins University School of Medicine.
Previous studies found that, in academic medicine, women comprise only 39% of full-time faculty and 22% of full-time professors. They are also significantly underrepresented in hospital leadership positions, and there are gender disparities regarding career advancement and compensation.
Hospital medicine as a dedicated medical specialty is a relatively young field. “Hospitalists” who are trained in internal medicine and focus their work on hospitalized patients rather than outpatient settings have only existed for about two decades. Due to how new the field is, some speculate it may have fewer gender imbalances than more established fields of medicine.
In collaboration with the Society of Hospital Medicine, Herzke and her colleagues conducted a survey of all U.S. academic hospital programs associated with the Association of American Medical Colleges. After identifying 135 programs, surveys were sent electronically to academic hospitalist leaders of each program. Participants were asked about the gender of the hospitalist program leader, the program’s size and organization, faculty characteristics, and perceptions about promotion and faculty development.
“We had a sense that there were some gender issues when people had looked at these areas before,” says Herzke. “Obviously, our hope was that we would see fewer inequities in our data.”
Of the 135 programs, 80 responded to the survey, and responding programs did not differ significantly from nonresponding programs in terms of funding, region, age or type of institution. While programs reported approximately equal numbers of male and female faculty members, 79% of program directors were male. Moreover, 37% of male hospitalist leaders were full professors while no female hospitalist leaders held that rank.
“Even in this new specialty, we don’t have gender parity,” says Herzke. “There have been numerous studies suggesting that programs, and society in general, do better when we have more diverse teams and diverse leadership.”
Herzke and her colleagues plan more studies to look at promotion and faculty development in academic hospital medicine. Also, they plan similar studies to understand if there are issues with racial inequity in leadership in academic hospital medicine. This topic in particular, says Herzke, is incredibly important to evaluate and, if inequality exists, address.
In addition to Carrie Herzke, authors of the Journal of General Internal Medicine paper are Amanda Bertram, Hsin-Chieh Yeh, Ariella Apfel and Joseph Cofrancesco Jr. of Johns Hopkins and Joanna Bonsall of Emory University.
The authors received no financial support for the research.
