Study: Rapid Test for Detecting COVID-19 Highly Accurate for Children and Adolescents
01/14/2022
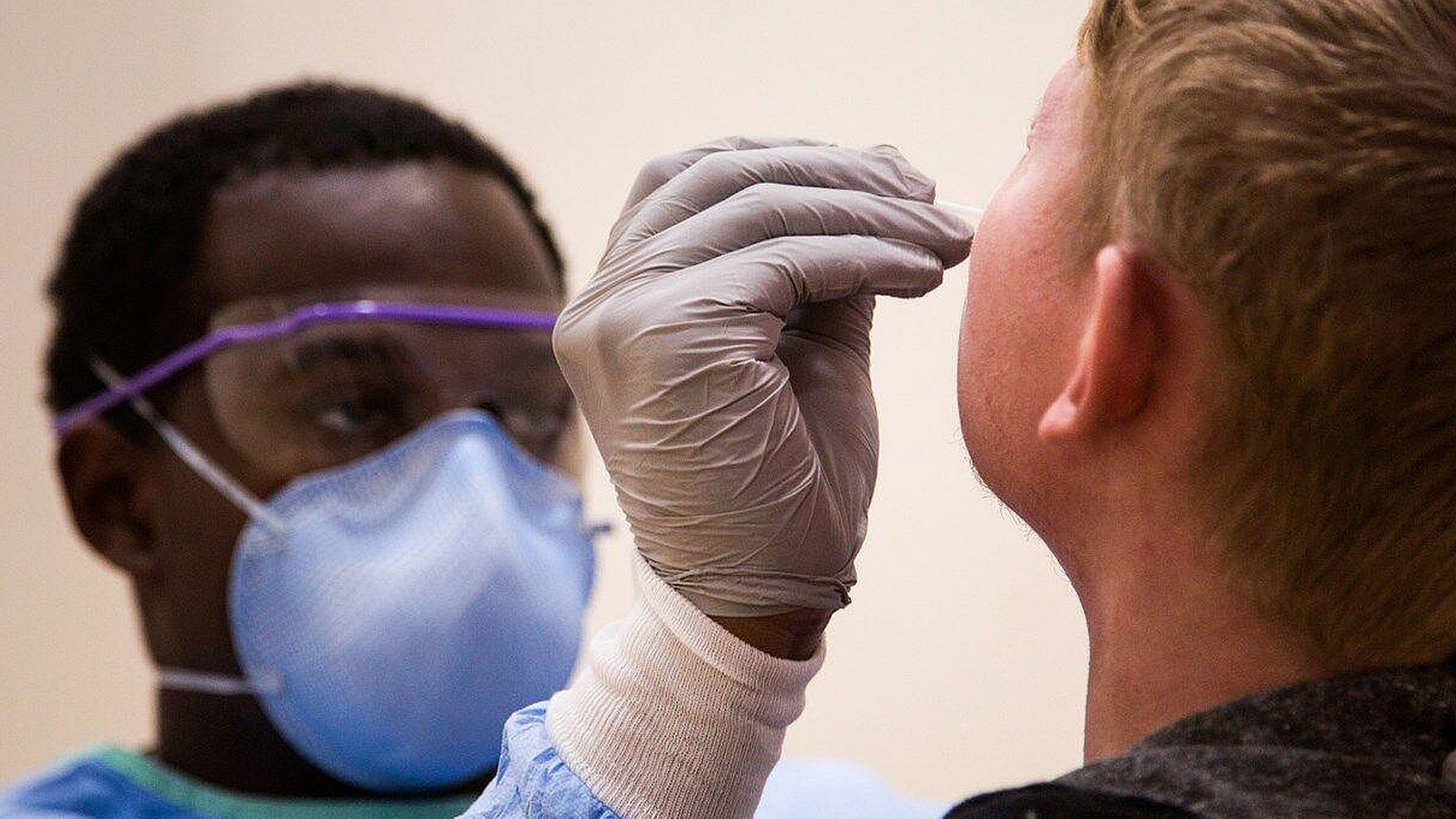
In a large prospective study of just over 1,000 patients ages 17 and younger who were seen at the Baltimore Convention Center Field Hospital (BCCFH) testing site during a seven-month period last year, researchers from Johns Hopkins Medicine and collaborating institutions report that a rapid antigen test for SARS-CoV-2 — the virus that causes COVID-19 — proved highly accurate when compared to the established standard virus detection method: the polymerase chain reaction (PCR).
The study researchers feel this suggests that rapid antigen testing can be confidently used to screen for children and adolescents who are infected but not showing symptoms. Such screening, they believe, could help keep classrooms safer when students attend in person.
The findings were first posted online Jan. 6, 2022, on the preprint website MedRxiv, where scientists and clinicians have been sharing urgent COVID-19 research before peer-reviewed journal publication.
“Quick, accurate and accessible diagnostic testing for SARS-CoV-2 in pediatric populations is critical to keeping children in classrooms, especially given the contagiousness of the newer virus variants, including delta and omicron,” says study senior author Zishan Siddiqui, M.D., assistant professor of medicine at the Johns Hopkins University School of Medicine. “Our research — conducted when the delta variant predominated — provides a timelier measure of the rapid antigen test’s accuracy in children than studies done before the more transmissible variants became prevalent.”
Siddiqui says the study showed that the rapid antigen test was high in sensitivity (ability to identify people for whom the PCR test would detect a SARS-CoV-2 infection) at 92.7% for all participants and specificity (ability to identify people for whom the PCR test would not detect a SARS-CoV-2 infection) at 98% for all participants.
The sensitivity was similar for symptomatic (92.3%) and asymptomatic (92.6%) cases.
The study also determined, Siddiqui says, that the negative predictive value (NPV — the probability that a person who tests negative has not been infected with SARS-CoV-2, as PCR would show) was high for both symptomatic (99.2%) and asymptomatic (99.7) young people.
These are significant findings, Siddiqui explains, because the rapid test offers advantages over the PCR test, including time savings (both during sampling and processing), cost savings and most importantly, ease of distribution and application — which can be done basically anywhere, including schools. This can help overcome COVID testing disparities for children and adolescents in medically underserved communities.
“Our findings of near 100% NPVs for both symptomatic and asymptomatic children and adolescents should pave the way for parents and school administrators to place more trust in the rapid antigen test results,” says study co-lead author Mary Jane Vaeth, a clinical assistant at the BCCFH.
“In turn, we hope that these results can inform educators in developing appropriate testing procedures to keep children in school,” adds study co-lead author Kristie Sun, a medical student at the Case Western Reserve University School of Medicine and public health graduate from The Johns Hopkins University.
The first step for both the PCR and rapid antigen tests is obtaining a patient sample, either from a nasal swab or a bit of saliva. The difference lies in how the sample is processed and analyzed. A PCR test takes a tiny bit of SARS-CoV-2 genetic material from a sample and reproduces it thousands of times so it can be more easily detected. A rapid antigen test uses laboratory-produced antibodies to seek out and latch onto proteins on the surface of SARS-CoV-2 particles in the sample.
The PCR test requires a skilled laboratory technician, special equipment and up to an hour or more to process. Often, results are not available until one or two days after the test. Additionally, testing on a massive scale can only be conducted at a large, centralized facility, such as a hospital laboratory.
On the other hand, rapid antigen testing uses a pre-made kit with a reagent that contains antibodies specific for SARS-CoV-2. The test can be conducted by anyone after brief training, can be administered anywhere and provides results in approximately 15 minutes.
In an earlier study at the BCCFH, Siddiqui and colleagues determined that while the PCR test may be better from a clinical perspective — it’s basically 100% accurate at detecting SARS-CoV-2 — the rapid antigen test appears to be better from a public health standpoint because of its ease of use, and because it proved to have sufficient accuracy, specificity and reliability for detecting the virus in a high-volume setting.
The researchers conducting the latest study wanted to see if the same was true for younger people.
As described in the preprint, the researchers administered both the rapid antigen and PCR detection methods for 1,054 children and adolescents age 17 and younger who came to the Baltimore field hospital for testing from May 7, 2021, to Dec. 6, 2021. Participants were screened before their tests for possible exposure to SARS-CoV-2 and for COVID-19 symptoms. Staff members were trained equivalently on test procedures and were monitored during administration to ensure quality control and reliable results.
Siddiqui says his team reported a high accuracy for rapid antigen tests to detect SARS-CoV-2 in children and adolescents. He believes that could play an important role in allowing students to limit their absences from school and other activities while in quarantine or awaiting confirming PCR test results.
“Our finding also provides support for the use of rapid tests in implementing ‘test-to-stay’ strategies, where exposed schoolchildren are enabled to continue uninterrupted in-person learning while being tested frequently after exposure,” he explains.
However, Siddiqui cautions that a negative rapid antigen test in children and adolescents should not be taken as a license to abandon other COVID-19 safety measures such as physical distancing, masking, frequent hand-washing and maintaining good ventilation.
“The rapid test should be considered another important layer of safety in keeping our children safer,” he says. “Based on our study findings — which did show a 30% false positive rate for the rapid test — a PCR test, when available, is recommended to confirm a positive rapid test result.”
Operated since April 2020 as a collaboration among Johns Hopkins Medicine, the University of Maryland Medical System and the Maryland Department of Health, the BCCFH provides SARS-CoV-2 testing and COVID-19 in-patient care, monoclonal antibody infusion therapy and vaccinations for Baltimore area residents, including those in medically underserved communities.
In a future study, the researchers plan to assess the accuracy of rapid antigen tests being marketed for home use.
Along with Siddiqui and Sun, the members of the study team from Johns Hopkins Medicine are James Ficke, Ishaan Gupta, Melinda Kantsiper, Charles Locke, Yukari Manabe and Matthew Robinson. Other study co-authors are Vaeth, Maisha Foyez, Asia Mitchell, Ria Peralta and Sophia Purekal from the BCCFH; Charles Callahan (who served as co-director of the BCCFH), James Campbell, Adrianne Hammershaimb and Kristie Johnson from the University of Maryland School of Medicine; and Maryam Elhabashy from the University of Maryland Baltimore County. Members of the CONQUER COVID Consortium also participated.
The rapid antigen test used in this study — and provided by the Maryland Department of Health to the research team at no charge — is the BinaxNOW test manufactured by Abbott Laboratories.
Manabe reports support from institutional grants given to Johns Hopkins Medicine from the National Institutes of Health; Becton, Dickinson and Co.; the U.S. Centers for Disease Control and Prevention; and the Baltimore City Health Department. She also reports equipment, drugs, medical writing, gifts or other services given to Johns Hopkins Medicine from Hologic; Becton, Dickinson and Co.; Roche; Cepheid and Chembio Diagnostics.
Robinson reports support from institutional grants given to Johns Hopkins Medicine from the National Institutes of Health; Becton, Dickinson and Co.; and the U.S. Centers for Disease Control and Prevention, as well equipment, drugs and materials given to Johns Hopkins Medicine from Becton, Dickinson and Co.
All other study authors report no conflicts of interest.
