Clues Found Regarding Tumor Suppressor Gene’s Breast Cancer Activity
12/08/2022
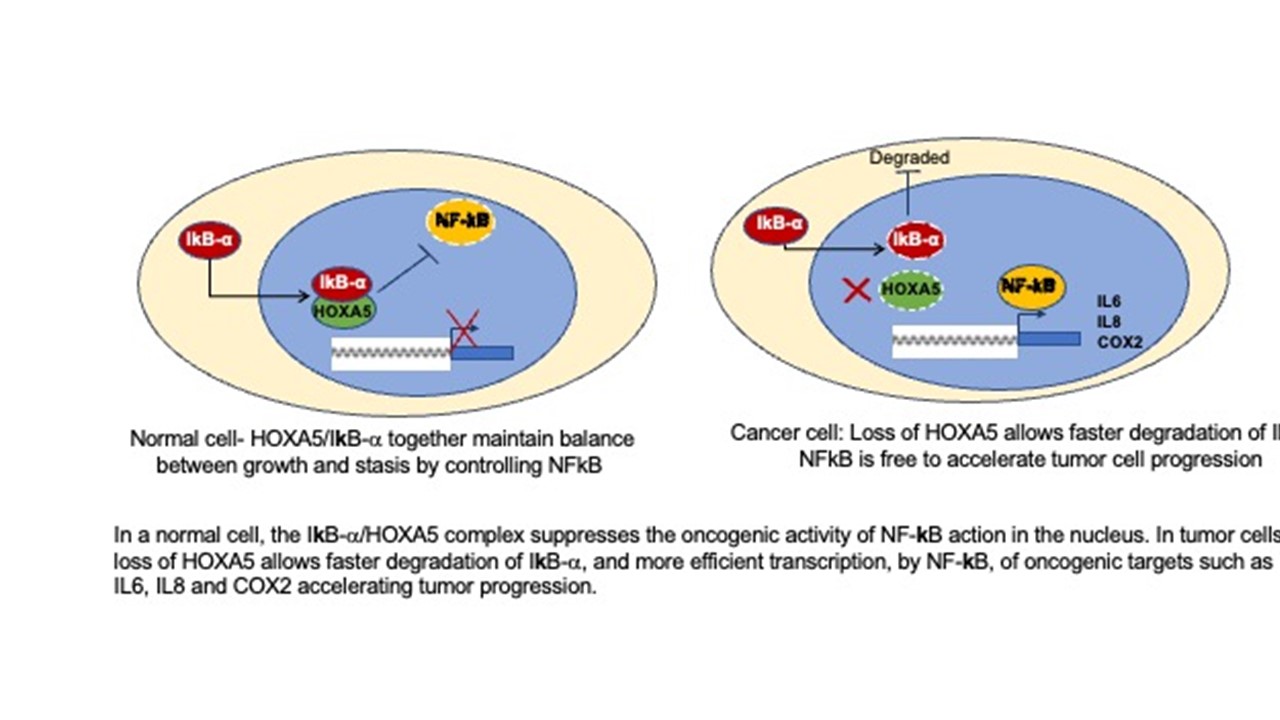
Researchers at the Johns Hopkins Kimmel Cancer Center have revealed how the gene HOXA5 may work to suppress formation of breast cancers. A new study indicates that it binds to another protein in an inflammatory cell pathway, boosting that protein’s cancer-suppressing properties.
A description of the work was published Oct. 15 in Cancer Research.
HOXA5 is in cells lining the breast, where it normally acts as a tumor suppressor and transcription factor. It helps new cells mature toward performing their ultimate functions, says senior study author Saraswati Sukumar, Ph.D., a professor of oncology and pathology at the Johns Hopkins University School of Medicine who has been studying this protein for 25 years.
Loss of HOXA5 results in cells becoming stuck in their incomplete differentiation stage, during which they begin to divide too much. This can lead to cancer. HOXA5 expression is lost in about 60% to 70% of all breast cancers, often occurring during an early stage of disease. Loss of HOXA5 alone, however, is not always sufficient to start the breast cancer process, and Sukumar’s team focused on understanding other steps involved.
In studies of breast cancer cell lines and in mice, Sukumar’s team discovered that HOXA5 has a partner — it binds to and stabilizes the cellular protein I kappa B alpha (IκB-α), which in turn inhibits NF-kappa B (NF-κB), a protein complex. Typically, NF-κB rushes to the nucleus and starts transcription of many cancer-causing genes, then IκB-α stops it. When HOXA5 is present, it’s able to help IκB-α suppress NF-κB activity more potently, but when HOXA5 is lost, IκB-α’s effect on NF-κB is lessened, and the potential for cancer development is greater.
“Our studies demonstrate that HOXA5 is acting to put brakes on a very important inflammatory pathway, which has been shown to be a promoter of the development of tumors,” Sukumar says. “Understanding precisely how this happens is of great importance, because increasing the amount of HOXA5 in these tumor cells may be a way forward to try to reverse the tumor formation process.”
In laboratory studies, Priya Pai, lead author and postdoctoral fellow, studied a cell line from nonmalignant tissue lining the breast (epithelial cells) that contained mutations in key breast cancer genes. Breast cancer cells sometimes become resistant to endocrine treatment by acquiring mutations in the gene PIK3CA, or resistant to anti-HER2 therapy through mutations in the HER2 gene. In cells that had mutations in the HER2 and PIK3CA genes, loss of HOXA5 induced the start of precancerous activity. When injected into mouse mammary ducts, the cells produced invasive tumor growth. The NF-κB pathway was significantly upregulated in the cells after HOXA5 was silenced. As a result of activation of the NF-κB pathway, multiple NF-κB target genes involved in exacerbating cancerous changes, such as IL-6 and COX2, also were upregulated. Collectively, the data suggest that the presence of HOXA5 suppresses malignancy in breast epithelial cells by blunting NF-κB action through stabilization of its inhibitor, IκB-α.
A new avenue of research is investigation of how lost HOXA5 can be replaced or reinstated so its tumor-suppressing functions can be restored to the cells, Sukumar says.
The work was supported by the Avon Foundation for Women.
Other researchers were Guannan Wang, Wei Wen Teo, Diana Raez-Rodriguez, Kathleen Gabrielson, Bradley Downs and Akanksha Aggarwal of Johns Hopkins, and Balázs Győrffy of Semmelweis University in Budapest, Hungary.
