Amoeba Biology Reveals Potential Treatment Target for Lung Disease
04/13/2021
In a series of experiments that began with amoebas — single-celled organisms that extend podlike appendages to move around — Johns Hopkins Medicine scientists say they have identified a genetic pathway that could be activated to help sweep out mucus from the lungs of people with chronic obstructive pulmonary disease a widespread lung ailment.
“Physician-scientists and fundamental biologists worked together to understand a problem at the root of a major human illness, and the problem, as often happens, relates to the core biology of cells,” says Doug Robinson, Ph.D., professor of cell biology, pharmacology and molecular sciences, medicine (pulmonary division), oncology, and chemical and biomedical engineering at the Johns Hopkins University School of Medicine.
Chronic obstructive pulmonary disease (COPD) is the fourth leading cause of death in the U.S., affecting more the 15 million adults, according to the U.S. Centers for Disease Control and Prevention. The disease causes the lungs to fill up with mucus and phlegm, and people with COPD experience chronic cough, wheezing and difficulty breathing. Cigarette smoking is the main cause in as many as three-quarters of COPD cases, and there is no cure or effective treatment available despite decades of research.
In a report on their new work, published Feb. 25 in the Journal of Cell Science, the researchers say they took a new approach to understanding the biology of the disorder by focusing on an organism with a much simpler biological structure than human cells to identify genes that might protect against the damaging chemicals in cigarette smoke.
Robinson and his collaborator, Ramana Sidhaye, M.D., also a professor of medicine in the Division of Pulmonology at Johns Hopkins, with their former lab member Corrine Kliment, M.D., Ph.D., counted on the knowledge that as species evolved, genetic pathways were frequently retained across the animal kingdom.
Enter the soil-dwelling amoeba Dictyostelium discoideum, which has long been studied to understand cell movement and communication. The scientists pumped lab-grade cigarette smoke through a tube and bubbled it into the liquid nutrients bathing the amoeba. Then, the scientists used engineered amoeba to identify genes that could provide protection against the smoke.
Looking at the genes that provided protection, creating “survivor” cells, one family of genes stood out among the rest: adenine nucleotide translocase (ANT). Proteins made by this group of genes are found in the membrane, or surface, of a cell’s energy powerhouse structure, known as mitochondria. Typically, mitochondria help make the fuel that cells use to survive. When an ANT gene is highly active, cells get better at making fuel, protecting them from the smoke.
Kliment, Robinson and the team suspected they also help amoeba overcome the damaging effects of cigarette smoke.
To better understand how ANT genes behave in humans, the scientists studied tissue samples of cells lining the lungs taken from 28 people with COPD who were treated at the University of Pittsburgh and compared the lung cells’ genetic activity with cells from 20 people with normal lung function.
The scientists found that COPD patients had about 20% less genetic expression of the ANT2 gene than those with normal lung function. They also found that mice exposed to smoke lose ANT2 gene expression.
Next, Robinson, Kliment and their research team sought to discover how ANT2 might provide protection from cigarette smoke chemicals and, in the process, discovered something completely unexpected.
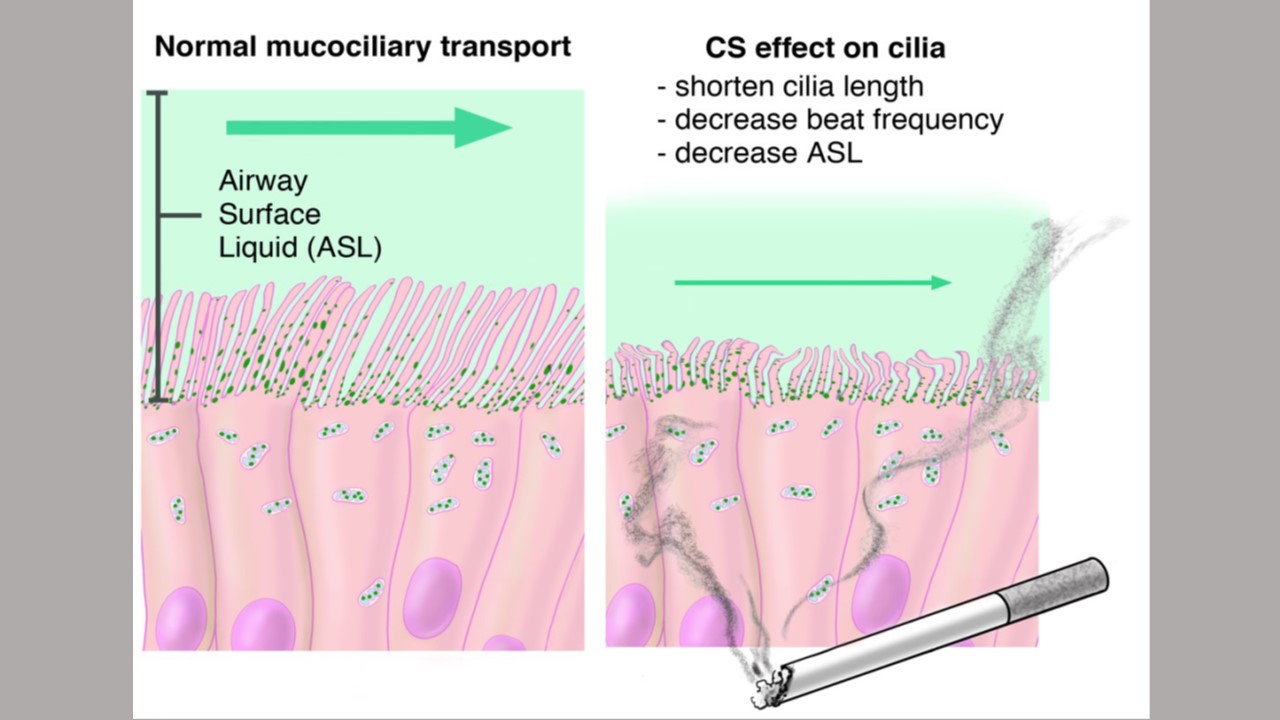
Cells lining the lungs use fingerlike projections called cilia to sweep mucus and other particles out of the lungs. In mammals, including people, the scientists found that the ANT2 gene produces proteins that localize in and around the cilia that work to release tiny amounts of the cell’s fuel into a watery substance next to the cell. The fuel enhances the ability of the cilia to “beat” rhythmically and regularly to sweep away the mucus.
“In COPD patients, mucus becomes too thick to sweep out of the lungs,” says Robinson.
The Johns Hopkins Medicine team found that, compared with human lung cells with normal ANT2 function, cilia in human lung cells lacking ANT2 beat 35% less effectively when exposed to smoke. In addition, the watery liquid next to the cell was about half the height of normal cells, suggesting the liquid was denser, which can also contribute to lower beat rates.
When the scientists genetically engineered the lung cells to have an overactive ANT2 gene and exposed them to smoke, the cells’ cilia beat with the same intensity as normal cells not exposed to smoke. The watery layer next to these cells was about 2.5 times taller than that of cells lacking ANT2.
“Cells are good at repurposing cellular processes across species, and in our experiments, we found that mammals have repurposed the ANT gene to help deliver cellular cues to build the appropriate hydration layer in airways,” says Robinson. “Who would have thought that a mitochondrial protein could also live at the cell surface and be responsible for helping airway cilia beat and move?”
Robinson says that further research may yield discoveries to develop gene therapy or drugs to add ANT2 function back into lung-lining cells as a potential treatment for COPD.
Robinson is now working to start a biotechnology company to further develop the technology. Kliment is continuing the work in her new laboratory at the University of Pittsburgh, where she is now an assistant professor of medicine in the Division of Pulmonary, Allergy and Critical Care Medicine.
Other scientists who contributed to the research include Jennifer Nguyen, YaWen Lu, Steven Claypool, and Pablo Iglesias from Johns Hopkins, and Mary Jane Kaltreider, Josiah Radder, Frank Sciurba, Yingze Zhang, and Alyssa Gregory from the University of Pittsburgh.
Funding for the research was provided by the National Institutes of Health’s National Heart, Lung, and Blood Institute (F32HL129660, K08HL141595, R01HL124099, R01HL108882); National Institute of General Medical Sciences (R01GM66817); a Biochemistry, Cellular, and Molecular Biology Program Training Grant (T32GM007445); the Burroughs Wellcome Fund; Parker B Francis Pulmonary Fellowship; the Johns Hopkins Bauernschmidt Fellowship Foundation; the Thomas Wilson Foundation; the American Heart Association; the Airway Cell and Tissue Core; the National Institute of Diabetes and Digestive and Kidney Diseases and the Cystic Fibrosis Foundation.
