$14 Million Grant to Fund Clinical Trial to Study Effectiveness of Hydrocephalus Treatment
08/25/2021
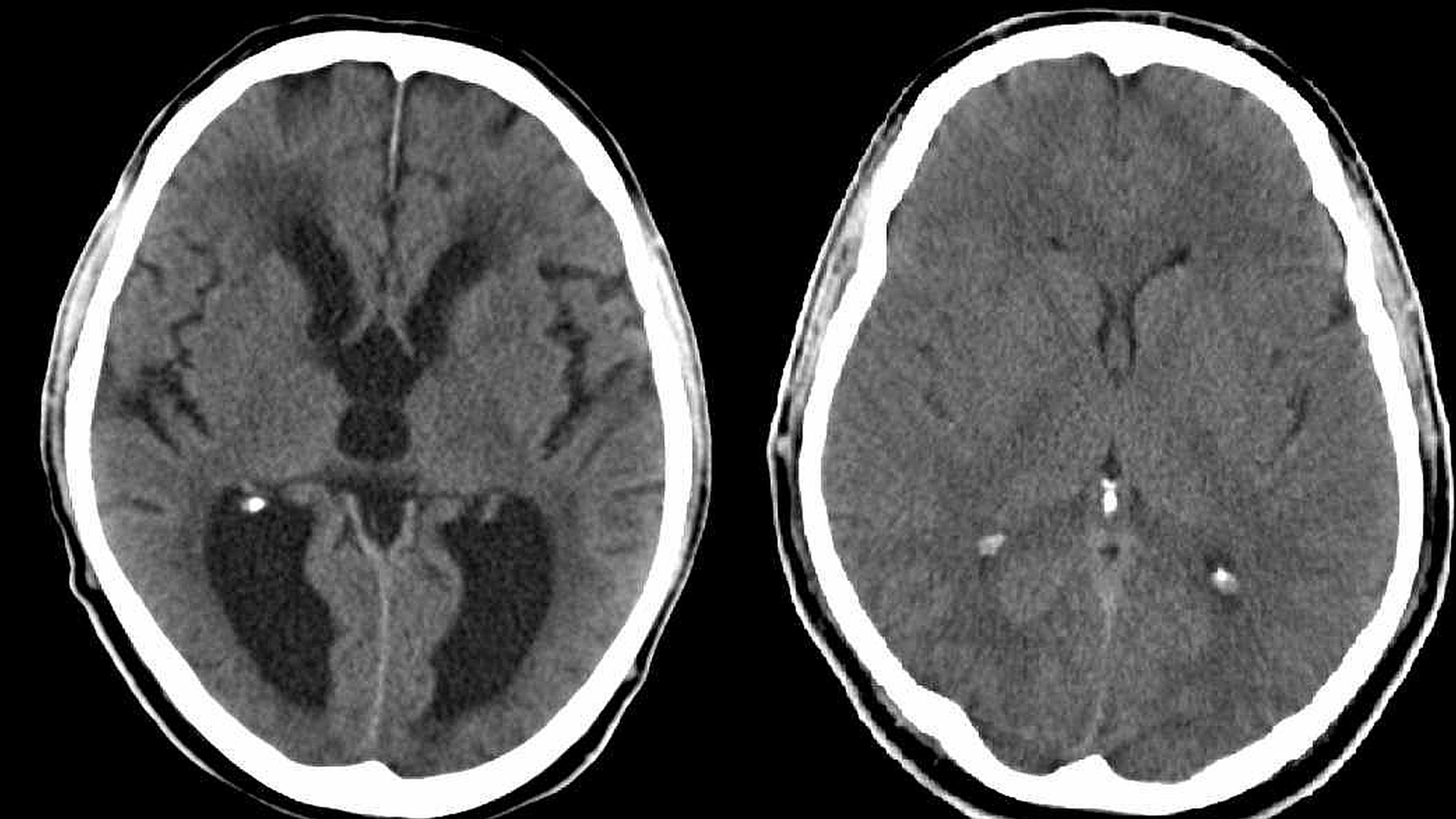
Patients diagnosed with idiopathic normal pressure hydrocephalus (iNPH), a type of brain swelling most commonly seen in older adults — and for which the underlying cause is unknown — are typically treated by surgically installing a shunt (drain) to remove the excess fluid associated with the condition. However, there is controversy in the medical community as to whether or not shunts are an effective form of treatment for patients with iNPH.
Thanks to a $14 million National Institute of Neurological Disorders and Stroke (NINDS) grant, researchers at the Johns Hopkins Cerebral Fluid Center in the Department of Neurosurgery hope to change that. The research is being conducted in partnership with the Adult Hydrocephalus Clinical Research Network (AHCRN) and coordinated by the Hydrocephalus Association, a non-profit organization that raises awareness of and support research on hydrocephalus.
According to the NINDS, hydrocephalus is an abnormal buildup of cerebrospinal fluid (CSF) — the clear liquid that protects and cushions the brain — circulating in the brain’s cavities (ventricles). Hydrocephalus occurs when the normal flow and absorption of CSF is blocked, leaving the excess fluid to widen and swell the ventricles. This puts pressure on the brain and keeps it from properly functioning, leading in turn to neurological damage and, in severe cases, death.
In the Placebo-Controlled Efficacy in iNPH Shunting (PENS) Trial, 100 patients with iNPH will undergo shunt surgery; however, the shunt will be open (on) in one group and remain closed (off) in the other. Only the surgeon will know if the shunt is open or closed. Through evaluations before and after surgery, researchers will determine if typical hydrocephalus-associated symptoms such as walking speed, cognition, mood and bladder control are alleviated in participants during the study period. The data will then be used to assess the effectiveness of treatment. After three months, patients in the closed group will have their shunts opened.
“This study is important because some in the medical community are currently not convinced that shunts are an effective treatment for iNPH,” says Mark Luciano, M.D., Ph.D., professor of neurosurgery at the Johns Hopkins University School of Medicine and director of the Cerebral Fluid Center. “Much of this uncertainty is due to the lack of a high quality randomized controlled trial, so we hope that our study will yield solid evidence about whether shunt surgery significantly helps the sufferers of iNPH.”
Luciano, who is a founding member of the AHCRN, says the trial will be the first to evaluate the true physiological response of shunting. Twenty teams at institutions around the world will contribute data to the study, along with evaluating a variety of methods to better diagnose iNPH.
“The idea of doing a true study on iNPH is something I’ve been working toward for more than 12 years,” Luciano says. “We believe this study will provide a needed firm foundation, not only to study the effectiveness of current treatments in iNPH, but to develop and evaluate new treatments in the future.”
Luciano is available for interviews.
