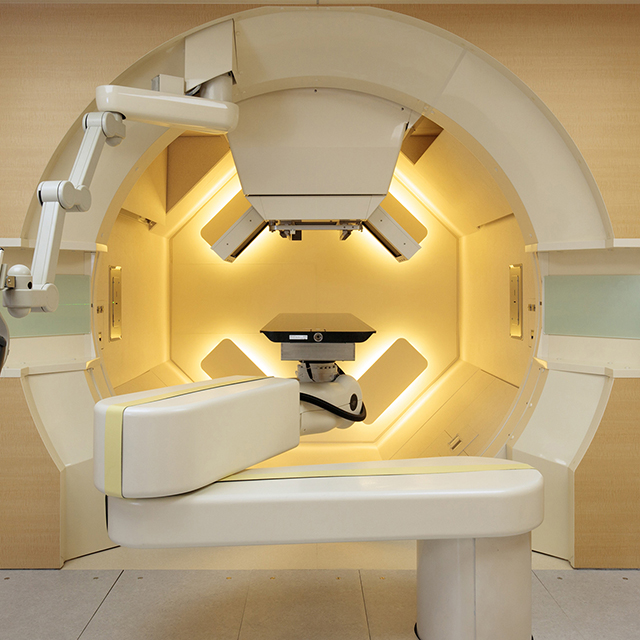
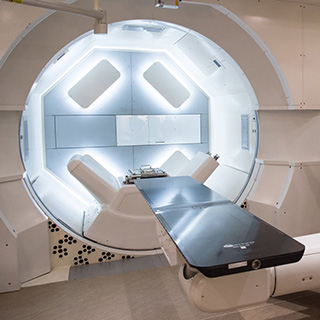
Traditional radiation, which uses X-rays to destroy cancer cells, allows 30 percent to 40 percent of the dose to pass through the targeted tumor. By contrast, proton therapy uses subatomic particles that stop at the depth of the tumor, preventing unnecessary damage to adjacent healthy cells and tissue. The result: less damage to delicate structures, such as the brain, heart and spinal column.
“We [now] have the ability to precisely target tumors with proton radiation, using sophisticated image guidance and ‘pencil beam’ scanning technology,” says Christina Tsien, medical director of the proton center, which is housed at Sibley Memorial Hospital in Washington D.C., and staffed with clinicians from the Johns Hopkins Kimmel Cancer Center.
“This allows us to deliver higher radiation doses to cancer cells while sparing nearby vital organs and normal tissues. As a result, patients are better able to tolerate radiation treatment with fewer short- and long-term side effects.”
Spinal tumors just behind the heart, tumors next to the eye, or tumors in the muscles next to reproductive organs are all situations where proton therapy shines. The risk of secondary cancers from treatment also decreases.
“We are able to treat a variety of cancer types,” says Curt Deville, clinical director and associate proton director.
Proton Power: The Synchrotron
<p style="text-align:start">At the Johns Hopkins Proton Therapy Center, the action starts in a huge particle accelerator known as a synchrotron, where protons spin at ultra-fast speeds before making their journey to treatment rooms. Here's a look at how the process unfolds.</p>
Proton therapy can be especially valuable for children because it minimizes the excess radiation that can impair growth, cognition, fertility, vision or hearing, notes Matthew Ladra, director of pediatric oncology at the Kimmel Cancer Center at Sibley.
A typical course of proton therapy is five days a week, for several weeks. The treatment itself takes just a few minutes, plus time for preparation and positioning. It’s usually painless, and most patients immediately return to daily activities.