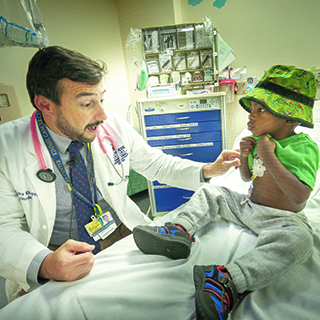
Like adult patients, pediatric patients receive radiation therapy as treatment for a variety of cancers. Brain tumors are the most common solid tumor in children and the cancer where most experts agree proton has the edge because of its ability to so precisely spare surrounding normal cells.
It is clear that every patient does not need proton therapy. “It’s a necessary tool to have to use at certain times, not every time,” says Theodore DeWeese. “We look at each patient—pediatric and adult—individually to bring the best technology and treatment plan we have to bear against their cancer. We look at anatomy of where the tumor is and what is the best approach to kill the cancer and preserve everything else.”
In fact, how to lessen the adverse effects of radiation has long been an area of research among the Kimmel Cancer Center’s pediatric radiation oncologists.
Although it is generally accepted that proton therapy provides benefit over other types of radiation therapy for pediatric patients, research studies are lacking, and our experts understand better than most the important role of laboratory and clinical science in setting the standard of pediatric cancer care. We’ve been leaders for more than a half-century.
 Moody Wharam, M.D.
Moody Wharam, M.D.When the National Cancer Institute established four study groups to investigate common childhood cancers in the late 1970’s, Johns Hopkins radiation oncologist Moody Wharam was the only expert appointed to two of the groups. From 1980 to 1990, he served as director of the radiation oncology committee of the Pediatric Oncology Group, now known as the Children’s Oncology Group, the world’s largest organization devoted exclusively to childhood and adolescent cancer research. Wharam and Kimmel Cancer Center collaborators were active participants in all of the pivotal pediatric cancer research of the time—research that led to dramatic increases in pediatric cancer survival rates.
“The way we manage radiation therapy in children today is based on what he did through all those years of tireless work. That’s why we do research,” says DeWeese.
The cruel irony that the radiation treatments given to save the lives of young patients also has the potential to cause harm continues to trouble radiation oncologists. Radiation to growing bones and organs can impede normal development, and radiation to the brain, a common site of pediatric cancers, too often results in impairments to learning and other cognitive brain functions.
In this long history of improving care for pediatric cancer patients, proton therapy is viewed as another major advance in managing late effects of radiation therapy. Matthew Ladra, director of pediatric radiation oncology, is eager to begin proton therapy studies. Ladra was the first radiation oncologist to earn a proton therapy-specific fellowship, which he completed at Massachusetts General Hospital. This training led to a directorship of the pediatric service at the Provision Center for Proton Therapy in Knoxville, TN.
Jen Holt, who also worked at the Provision Center, joined Ladra as nurse manager for the pediatric radiation oncology program.
“When children get exposed to radiation at a young age, they are at much higher risk for issues down the road when they are long term survivors,” says Ladra. He is among a select number of radiation oncologists whose practice and research focus solely on pediatric cancers.
Our goal is to radiate what’s supposed to be radiated and leave everything else alone. Proton therapy helps us do that.
- Matthew Ladra, M.D., M.P.H.
The ability to better steer protons to the cancer and stop the beam means developing brains, the heart, lungs and growing bones can be better protected.
Ladra, says he has seen the benefits. He recalls brain tumor patients he treated with proton therapy who have none of the telltale signs of a brain tumor battle. “They have no cognitive issues. They are growing normally. It’s very rewarding, and the technology we have at Johns Hopkins is even better, and that means there are still advances that can be made,” says Ladra.
Still he knows that there is a difference between anecdotal reports of benefits and scientific evidence. The latter is a key element that has been missing from the conversation.
Novel research, including a map of the brain that relates dose of radiation to impact on specific areas of the brain, showing the maximum dose of radiation each area of a young brain can tolerate without causing functional deficits, is providing information that other centers don’t have. It is revealing areas that will require smaller doses of radiation but also others that could safely tolerate larger doses.
The opportunity to study the benefits of proton therapy is what attracted him to the Kimmel Cancer Center. The Johns Hopkins Proton Therapy Center is only one of two in the country that has a dedicated pediatric facility and a proton research program.
“This is a truly visionary approach. Research is the only way to get at concrete evidence of the advantage of using protons to treat children and to show us how we can improve the care of kids moving forward,” says Holt.
The dedicated pediatric oncology service has its own team of experts—radiation oncologists and technicians, pediatric nurses, including a nurse practitioner and nurse navigator, a child life specialist, a nutritionist, survivorship and family counselors and a pediatric anesthesiologist, as very young patients often require some sedation during treatment.
“The proton therapy technology is much better now, and we will have the most up-to-date proton facility, but expertise is critical,” says DeWeese. “Like anything else, it has to be done well. We are learning now that there can be issues with proton therapy when not done correctly.
Proton therapy may also be a better option for pediatric patients with sarcoma, cancers of the bone and soft connective tissue. Sarcomas are particularly challenging to treat because they often occur in the vicinity of other vital anatomy and growing organs. With its precision, the proton beam offers the ability to get at the cancer without harming these nearby structures. As a result, experts believe it may help patients avoid amputation.
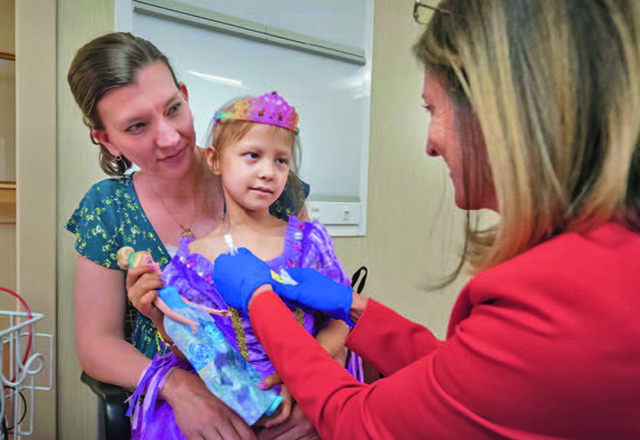 The dedicated pediatric oncology service has its own team of experts, including pediatric anesthesiologist Eugenie Heitmiller, M.D.
The dedicated pediatric oncology service has its own team of experts, including pediatric anesthesiologist Eugenie Heitmiller, M.D.Spinal tumors, cancers in the head and neck, tumors that are close to other organs—which in the small bodies of children can be many—and abdominal and pelvic tumors are also well suited to proton therapy.
For example, a toddler with a tumor sitting close to growth plates in the pelvis can be treated with proton therapy to protect the pelvic bones from radiation damage that can cause the growth plates to close, resulting in growth issues and other problems later in life. In other cancers, such as Hodgkin lymphoma, that require radiation to the chest, proton therapy can protect the heart and lungs. In other cases, another type of radiation therapy may be preferable.
“Proton therapy is an essential tool to have at certain times, but it’s not the only tool,” says Ladra. “We look at anatomy of where the tumor is and what we need to preserve and decide case by case if the patient would most benefit from proton therapy.”
A teenage patient recently treated for osteosarcoma that had spread, creating a golf ball-sized tumor in the patient’s lung, benefited from stereotactic ablative radiation. Surgery was not an option because of pre-exiting damage to the lung. Immunotherapy with drugs aimed at boosting the immune system to attack the cancer was not keeping the cancer in check, so the multispecialty team of doctors decided to use stereotactic radiosurgery to go after the tumor in her lung. The tumor disappeared, and the patient remains cancer-free.
The combined treatment of immunotherapy and stereotactic ablative radiation allowed her to avoid more toxic chemotherapy that is frequently ineffective against advanced osteosarcoma. For the teenager who was about to begin high school, it was also a quality of life issue. She didn’t want her hair to fall out and the radiation/immunotherapy combination worked better against her cancer without altering her appearance.
Working in collaboration with experts at the Bloomberg~Kimmel Institute for Cancer Immunotherapy, our radiation oncologists uncovered evidence that cancer cells killed by radiation signal the immune system as they die, revealing their identity as a cancer cell and setting cancer-killing immune cells into action. Similar studies are planned combining immunotherapy and proton therapy.
“In a center with so much strength in every area of cancer research and therapy, we have more information to help inform our treatment decisions and that leads to novel, patient-centered medicine and better outcomes,” says Holt. “There are so many things available here—comparative planning, specialized nursing care, multispecialty collaboration—that are not available at other places. The fact that we’re different from most of the proton centers out there is also what makes us better. Our patients get it and their parents get it.”
 Akila Viswanathan, M.D., M.P.H. (left) and Jeffrey Dome, M.D., Ph.D.
Akila Viswanathan, M.D., M.P.H. (left) and Jeffrey Dome, M.D., Ph.D.The knowledge about the cancer being treated must be equivalent to the proton expertise, Akila Viswanathan stresses. The multispecialty approach the Kimmel Cancer Center uses means each patient’s care is informed by every specialist. Radiation oncologists, medical oncologists, pathologists, nurses, surgeons and other experts work together to evaluate every case and develop the best treatment plan. “This multidisciplinary component is so important because what really makes proton therapy at the Kimmel Cancer Center special is what our experts bring to it,” she says.
Unique Collaboration
It is this kind of pioneering influence that earned the radiation oncology program distinction as one of a select few in the nation with a long and proven track record of excellence in treating pediatric cancers.
In 2013, it helped pave the way for a collaboration with Children’s National. It creates one of the largest pediatric radiation oncology programs in the country, and the increase in patient volume promises to speed clinical discovery.
“It is another example of our strategic focus to consistently partner with organizations in the region to bring high-quality accessible care to children and families,” says Elizabeth Flury, Executive Vice President and Chief Strategy Officer at Children’s National. “When we base our strategic decisions around what’s best for the child, everyone wins. This collaboration is a perfect example of that thinking.”
Theodore DeWeese believes it is a national model. “This shows how two nationally respected institutions came together in a collaborative and strategic way to change the face of pediatric cancer care in the region and around the world,” he says.
 Kurt Newman, M.D. (left) and Theodore DeWeese, M.D.
Kurt Newman, M.D. (left) and Theodore DeWeese, M.D.Through the collaboration, patients have access to the combined expertise of Children’s National and the Kimmel Cancer Center’s pediatric oncology program. The Kimmel Cancer Center’s pediatric cancer program has consistently been ranked by U.S. News and World Report as one of the top pediatric cancer programs in the country, and Children’s National was also ranked as one of the top five children’s hospitals in the country. The collaborations include joint clinical trials and research initiatives with the National Institutes of Health.
“Working together through an integrated radiation oncology service—including research—we are providing important new treatment options for kids fighting cancer who live in the capital area or who travel here to take advantage of our joint expertise,” says Kurt Newman, President and Chief Executive Officer of Children’s National. The joining of these two leading programs marks a significant achievement in children’s health, he says.
The collaboration represents the first pediatric radiation oncology program in the national capital region. DeWeese says the dedicated, multispecialty team brings the most advanced therapy and the highest level of safety and quality care for pediatric patients and families.
“There are cases in which radiation is the best way to enhance treatment for a young patient," says Jeffrey Dome, Oncology Division Chief at Children's National. "This collaboration is focused in finding the best strategies based on current research to integrate radiation therapy into a comprehensive care regime."
Built on Tradition
 From left: Lin Whetzel, BS.N., R.N., Jennifer Holt, B.S.N., R.N., Matthew Ladra, M.D., M.P.H., Andrea Lattimore, B.S.N., R.N., Judy Tran, C.R.N.P.
From left: Lin Whetzel, BS.N., R.N., Jennifer Holt, B.S.N., R.N., Matthew Ladra, M.D., M.P.H., Andrea Lattimore, B.S.N., R.N., Judy Tran, C.R.N.P.So many things in cancer research have their roots in the Kimmel Cancer Center. It is this convergence of expertise that makes the Johns Hopkins Proton Therapy Center stand out among others. Kimmel Cancer Center scientists and clinicians bring expertise to all areas of the cancer compendium and are among the undisputed leaders in cancer genetics, epigenetics and immunotherapy. Add to that Magnet nursing status recognition for quality of care and one of the first programs to study late effects of cancer treatment, complete integration of cancer services across all Kimmel Cancer Center locations, and before its doors even open, the Johns Hopkins Proton Therapy Center distinguishes itself among cancer centers and proton centers alike—in the Baltimore/Washington region and around the country.
 Jean Wright, M.D.
Jean Wright, M.D.To ensure quality of care and access to proton therapy among all of our sites, radiation oncologist Daniel Song will lead regional chart rounds to discuss patient cases across all Kimmel Cancer Center locations, including Sibley, Suburban, Green Spring Station, Johns Hopkins Bayview Medical Center and Johns Hopkins Hospital. Jean Wright will oversee safety and quality across all locations. Clinical nurse specialist Jen Weiworka bridges all of the sites, overseeing intensive training for nurses to ensure the same standard of care exists at every Kimmel Cancer Center location.
In addition to the cancer acumen of leaders in every field of cancer research and treatment, the Proton Therapy Center has at its disposal the brain trust of all of Johns Hopkins University to lend their expertise and advance the application of proton therapy alone and in combination with other cancer treatments. This progress is in line with everything else our experts are doing to make cancer therapies work better for patients while also limiting toxicities. Targeted drug therapies, organ-sparing surgeries and less toxic proton therapy all have this goal.
Two specialized institutes will also support our proton center. A new Translational Convergence Institute brings doctors, nurses, astronomers, engineers, computer scientists, physicists, bioethicists, biologists, materials scientists and mathematicians together to work side by side to amass and apply their knowledge to cancer. They will solve complicated and vexing problems, build new technologies, consider out of the box, creative new approaches that can only be found through this type of directed collaboration.
The Bloomberg~Kimmel Institute for Cancer Immunotherapy will help integrate proton therapy with immunotherapy, revolutionary new treatments that activate the immune system to attack cancers. A Drug Discovery and Development program will advance combined treatments with new targeted therapies, and a first-of-its-kind Cancer Invasion and Metastasis Program, co-lead by radiation oncologist Phuoc Tran, will study proton therapy, among other treatments, to transform the management of advanced cancers.
“We can bring together so many things that are not available at other places. This wealth of expertise means we have more information coming, more people informing decisions and solving problems, and that leads to better outcomes for patients,” says Akila Viswanathan. “We approach cancer from all angles. There is not one single preferred solution. Sometimes it is a combination of therapies.”
Viswanathan says one of the most important collaborations will be with the community of primary care providers who choose us to work with them to develop the optimal treatment plans for their patients.
“The Johns Hopkins Proton Therapy Center is one of the few comprehensive proton centers in the world. We will be doing research that has never been done before,” says Theodore DeWeese. “It’s going to be a huge advance for the field.”