Illustration by Anna Godeassi
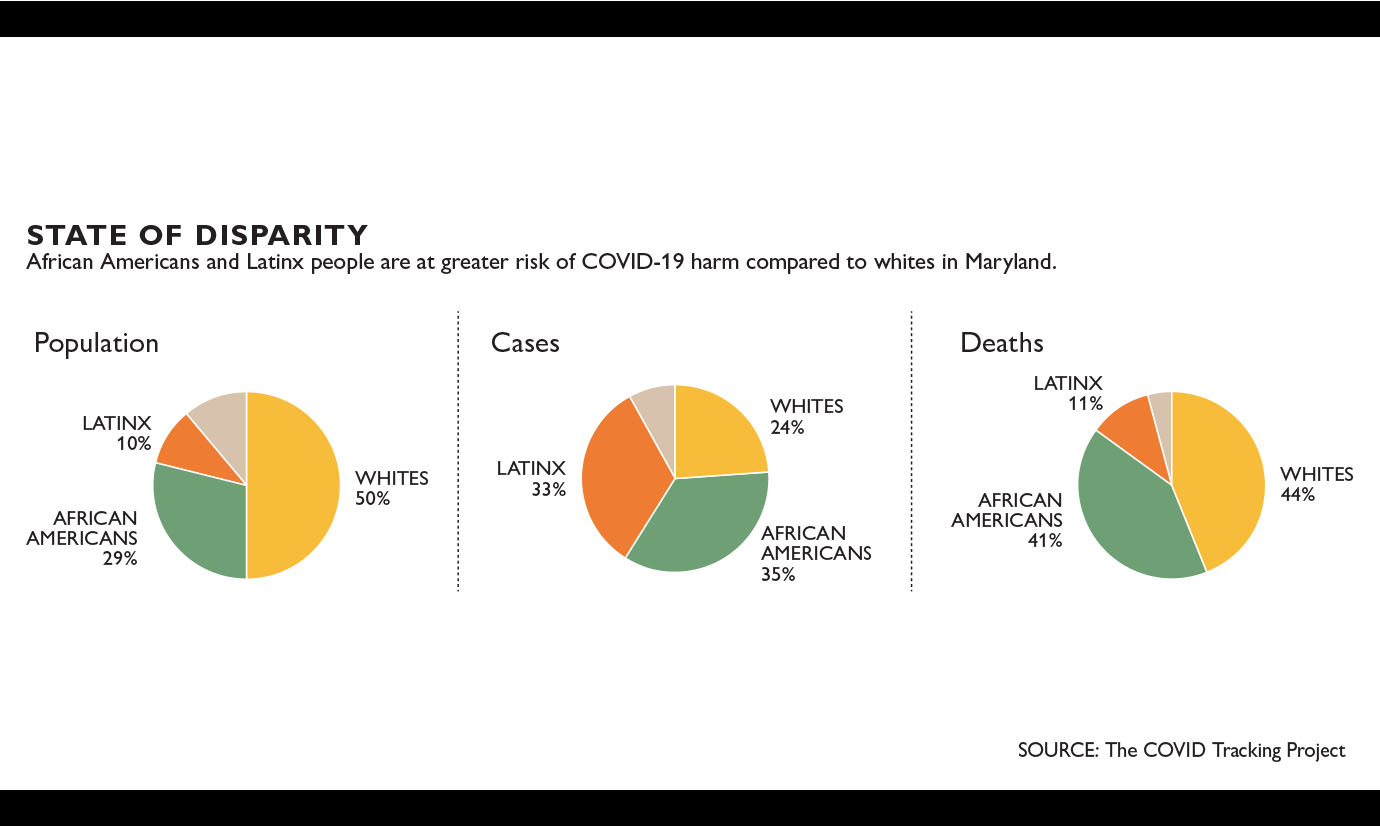
A wide-ranging initiative is addressing the disproportionate harm COVID-19 is causing African American and Latinx people in Baltimore.
Peering at his computer, Panagis Galiatsatos assesses the seating arrangement of a Baltimore church. He’s pleased to see that congregants will be spaced more than 6 feet apart, as recommended to prevent the spread of the coronavirus that causes COVID-19.
Since March, Galiatsatos has been participating in frequent telephone and video conversations with leaders of local churches, synagogues and mosques.
“The frontline people are not the doctors and nurses. We are the last line. The community is the front line,” says Galiatsatos, a pulmonary and critical care doctor and co-founder of Medicine for the Greater Good. “The more the population can spread proper information and not spread the virus, the better we can be at putting an end to this pandemic.”
The conversations are part of a multipronged push by Johns Hopkins Medicine and The Johns Hopkins University to tackle a troubling aspect of the COVID-19 pandemic: the disproportionate harm it is causing to already disadvantaged communities, particularly African American and Latinx people.
Through the effort, called the COVID-19 Pandemic Anchor Strategy, Johns Hopkins leaders coordinate with the Baltimore school system, the city and state health departments, and other agencies to bring information and testing to Baltimore neighborhoods, provide additional bilingual support for Spanish-speaking patients, distribute food and open crucial lines of communication with community residents and leaders.
“You can give people medicine, but if you’re not meeting their basic needs, you’re not really treating the whole person,” says Sherita Hill Golden, vice president and chief diversity officer at Johns Hopkins Medicine and a member of the Anchor Strategy group.
To date, Johns Hopkins experts have led phone and video conversations and town halls with clergy members, parents, students and older adults on topics such as how to entertain children during the summer and legal rights in case of eviction. Virtual movie nights, TikTok competitions and trivia games, offered in English and Spanish, provide more opportunities to build connections with young people. Flyers distributed in English and Spanish give information about physical distancing, mask wearing and other safety measures.
In addition, a new initiative called Juntos seeks to reduce cultural and language isolation for Latinx patients and their families by connecting them with bilingual clinicians. The service does not replace medical interpretation, but it offers additional support for this vulnerable population.
Talia Robledo-Gil, an internal medicine-urban health resident, is among a dozen Juntos volunteers who talk with patients and family members. “With really critically ill patients, it can mean explaining to their loved ones why they need to be intubated, even though they seemed fine yesterday,” says Robledo-Gil.
Johns Hopkins clinicians are also traveling to homeless shelters, sober living facilities and neighborhoods deemed COVID-19 hot spots to provide on-site testing. They set up temporary testing sites in response to requests from the city or from organizations like Health Care for the Homeless or Helping Up Mission. The testing teams notify people of their test results and help them get appropriate care if needed.
Advocacy is also crucial. “We are working with our government and community affairs team to brief state lawmakers about COVID-19 and disparities,” says Golden. There are also plans to recommend legislation aimed at reducing health disparities.