Taking Action Against Antibiotic Resistance
Antimicrobial stewards at Johns Hopkins chart a course for fewer medications, better health.

From left: Morgan Katz, Sara Cosgrove and Valeria Fabre, infectious disease physicians at The Johns Hopkins Hospital and the Johns Hopkins Bayview Medical Center.
Here’s a common scenario: A resident of a long-term care facility develops cloudy urine, and a culture comes back with growing bacteria that could signal a urinary tract infection.
For many clinicians, the logical course of action would be to prescribe antibiotics, even though the cloudy urine and the presence of bacteria alone do not necessarily indicate a urinary tract infection (UTI).
Instead, say antimicrobial stewards at Johns Hopkins, antibiotics should be avoided unless the resident has signs and symptoms of a true UTI.
Antibiotics are inexpensive and readily available. They often prove beneficial and even lifesaving. When they don’t work, they still can give clinicians, as well as patients and their families, the comforting assurance that something is being done to help the person get better.
But overprescribing can be harmful to patients, and it promotes resistance to bacteria that makes treatments less effective in the future.
Sara Cosgrove, Valeria Fabre and Morgan Katz, infectious disease physicians and antimicrobial stewards at The Johns Hopkins Hospital and the Johns Hopkins Bayview Medical Center, are helping clinicians take a more nuanced approach, providing education and tools to better manage antibiotic use at Johns Hopkins, long-term care facilities and even in other countries.
Prescribing antibiotics to all long-term care patients with positive urine cultures, regardless of symptoms, is a major source of increased antibiotic resistance, says Katz, assistant professor of medicine.
And, in many cases, it’s not necessary.
“About 50% of nursing home residents have asymptomatic bacteria,” she explains. “As you get older, your urinary tract can get colonized with bacteria, but it often does not cause symptoms and doesn't need to be treated.”
With funding from the Agency for Healthcare Research and Quality (AHRQ), Cosgrove and Katz developed an education program to guide antibiotic use in skilled nursing facilities, residential and continuing care communities, and hospice and dementia care settings.
The intervention includes 15 webinars for clinical staff members, plus activities, and posters and other materials, that frame antibiotic stewardship as an important method to promote patient safety.
Clinicians were urged to be sure, before prescribing antibiotics, that the patient would truly benefit from the medication, and if so to ask themselves daily when the treatment could be decreased or stopped. (See sidebar about the four moments of antibiotic decision making, published in the Journal of the American Medical Association in 2019. Authors included Cosgrove and Johns Hopkins associate professor of pediatrics Pranita Tamma. The information was later modified for acute, long-term care and ambulatory care settings.)
Care facilities that used the material reduced antibiotic use, note Cosgrove, Katz and others in a February 2022 JAMA Network Open report.
The results show the effectiveness of antimicrobial stewardship programs, even — or especially — in settings with people who may be nonverbal or experiencing vague symptoms, says Katz.
As antibiotic stewards at Johns Hopkins, Cosgrove and Katz set guidelines that clinicians can access through an app and on workstations.
“They’re very comprehensive,” says Cosgrove, a Johns Hopkins professor of medicine. “They say how to respond to specific conditions, and we have sections on dosing and on the antibiotics themselves.”
Yet guidelines alone are not enough, she says.
The stewards provide antimicrobial education to students and clinicians, and require approval from infectious disease specialists for some antibiotic prescriptions. Clinical pharmacists are trained in antibiotic approvals and in how to have conversations with clinicians about stopping and narrowing therapy.
However, “it is not possible for the three or four people in your stewardship program to intervene on all patients receiving antibiotics in the hospital,” Cosgrove says. “What really makes me happy is when I hear clinicians talking about these things, saying they’re going to narrow the duration of treatment or that they’re going to stop antibiotics because they don’t think the patient has an infection.”
A Spotlight on Antimicrobial Stewardship
Antibiotics have serious downsides, particularly when overprescribed, the clinicians note. They can destroy useful gut flora, causing discomfort and placing people at risk for Clostridioides difficile infection, which can cause a type of diarrhea that can progress to be life threatening.
Zoom out to the population at large, and overuse of antibiotics undermines their efficacy, as bacteria adapt to survive the medications.
Fabre, associate professor of medicine, works with infectious disease physicians and microbiologists in Latin American countries to develop stewardship programs at their hospitals, and she hopes to expand the effort to outpatient facilities.
“Most hospitals [in Latin America] perform antibiotic stewardship activities, but they don’t necessarily have a program,” Fabre says. Her work includes setting up clinical tools to determine when using antibiotics is unnecessary or can wait, educating the pharmacists and nurses who administer antibiotics, and helping hospitals assess their current programs, resources and antibiotic use.
Cosgrove notes that concerns about antibiotic overuse are as old as the medications themselves.
“We were warned by Alexander Fleming (who discovered the world’s first antibiotic, penicillin, in 1928) that if we use too much penicillin, particularly in situations where it is not needed, we could have problems with resistance,” Cosgrove says.
Since then, reliance on antibiotics has escalated with advances in medical care, such as organ transplants and other surgeries. So has microbe resistance, as bacteria evolve to survive new antibiotic offerings.
In 2014, President Barack Obama promoted a national strategy for combating antibiotic-resistant bacteria, guided by a report developed by the President’s Council of Advisors on Science and Technology, members of which are scientists and engineers.
“When used appropriately, antibiotics are amazing,” says Cosgrove, a member of the council’s inaugural working group. “If you have strep throat or pneumonia and you take antibiotics, you feel better right away. They save so many lives. Because of that, they also sometimes become a security blanket. It’s hard to say no to antibiotics, to explain to a patient that it’s not an infection, it’s an asthma flare.”
The report to the president notes: “Without rapid and coordinated action, the Nation risks losing the tremendous public health progress made over the last century from the discovery and development of antibiotic drugs, thereby threatening patient care, economic growth, public health, agriculture, economic security, and national security.”
The report cites Centers for Disease Control and Prevention findings that “up to 50 percent of all the antibiotics prescribed for patients in the United States are not needed or are not optimally prescribed.”
Johns Hopkins antimicrobial stewards are doing their part to change that.
The Four Moments of Antibiotic Decision Making
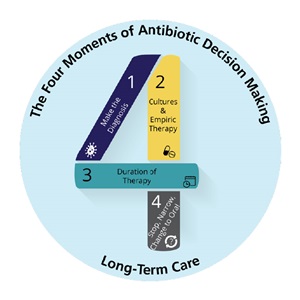
Moment One: Does the patient have symptoms that suggest an infection?
Moment Two: What type of infection is it? Have we collected appropriate cultures before starting antibiotics? What empiric therapy should be initiated?
Moment Three: What duration of antibiotic therapy is needed for the patient’s diagnosis?
Moment Four: It’s been 2–3 days since we started antibiotics. Re-evaluate the patient and review results of diagnostic tests. Can we stop antibiotics? Can we narrow therapy? Can we change to oral antibiotics?
