On a cool spring Saturday morning, Katie O’Conor and nine other Johns Hopkins clinicians and administrators arrive at the intersection of North Fremont Avenue and Laurens Street, in the Upton neighborhood of West Baltimore.
They set up folding chairs and tables, arrange computers and stack consent forms. They put out single-serve snacks and bottles of water.
In a few minutes, people who inject drugs would come to this city-run syringe exchange site to swap their used supplies for clean ones. When they did, the Johns Hopkins mobile COVID-19 vaccination clinic would be ready.
“What I love about this is we are adapting the environment to meet the community’s needs,” says O’Conor, an emergency medicine/anesthesiology resident and co-chair of the Johns Hopkins Vaccine Equity Task Force.
That day, the Johns Hopkins team would vaccinate 60 people, says O’Conor.
That may seem like a small number in a city of nearly 576,000, but O’Conor knows that every shot in every arm brings the pandemic closer to containment, particularly when those arms belong to people most at risk for getting seriously ill or dying of COVID-19.
Her group and other vaccine equity teams at Johns Hopkins Medicine are concentrating their efforts on people who are hardest hit by the COVID-19 pandemic, including those who are Black, Latino, Indigenous or elderly. The idea is to remove logistical and psychological barriers for people who may lack the time or transportation to make and keep vaccine appointments.
O’Conor and others at Johns Hopkins are making it easier for them by bringing the doses to street corners, churches and public housing complexes.
“We do not require anyone else to have computer or health literacy,” says O’Conor. “It’s on us.”
At the syringe exchange site, participants did not need appointments. Instead, Johns Hopkins administrators registered them on the spot, assuring them that their information would not wind up with law enforcement or immigration officials.
People at the syringe exchange site were already taking action to protect their health; O’Conor says she was not surprised that they also lined up for the vaccine.
It helped that they were offered a choice between the two-dose Pfizer vaccine and the single-dose Johnson & Johnson vaccine. “This population, with substance use and unstable housing, doesn’t often have access to choices, on their terms,” says O’Conor, adding that about 60% chose Pfizer.
O’Conor’s mobile vaccination clinics, operating since late February, have provided at least one vaccine dose to more than 2,700 Baltimoreans.
Nearly 2,000 additional city residents have received at least one dose through clinics run by Kathleen Page, co-director of Centro SOL, the Johns Hopkins-based group that promotes health equity for Latinos in Baltimore. (See sidebar for more about vaccine outreach to Baltimore’s Spanish-speaking residents.)
And 2,545 people in Washington, D.C., communities with high infection rates are fully vaccinated, thanks to Johns Hopkins clinics.
“In order to achieve high vaccination rates, we need to reach out to every group,” says Ben Bigelow, the Johns Hopkins medical student who is spearheading all three vaccine equity efforts across Johns Hopkins Medicine.
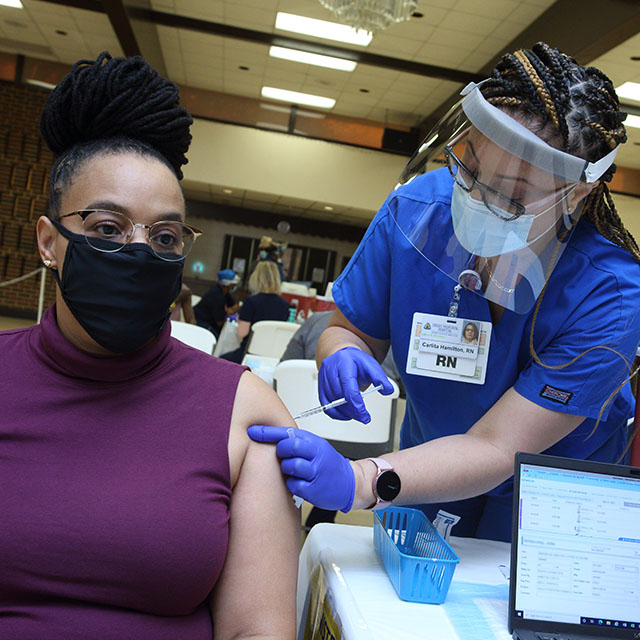
Delivering COVID-19 Vaccine Equity
Vaccine equity teams at Johns Hopkins are setting up COVID-19 vaccine clinics on street corners and in churches, making vaccination easier for people with demanding work schedules, transportation challenges, language barriers or concerns about citizenship.