-
Gary Gallia, M.D., Ph.D.

- Surgical Director of the Pituitary Center
- Director of the Neurosurgery Skull Base Center
- Director of Endoscopic and Minimally Invasive Neurosurgery
- Professor of Neurosurgery
- Professor of Oncology
- Professor of Otolaryngology - Head and Neck Surgery
Research Interests: Brain tumors, gliomas, skull base tumors, model development, genetics, preclinical testing
-
Gregory Riggins, M.D., Ph.D.

- Irving J. Sherman Research Professor
- Professor of Neurosurgery
- Professor of Oncology
The Brain Cancer Biology & Therapy Laboratory
The goal of the Johns Hopkins Brain Cancer Biology and Therapy Laboratory (led by Dr Gregory Riggins) is to locate the genetic and genomic changes that lead to brain cancer. These molecular changes are evaluated for their potential as therapeutic targets and are often mutated genes, or genes that are over-expressed during the development of a brain cancer.
The brain cancers that the Riggins Laboratory studies are medulloblastomas and glioblastomas. Medulloblastomas are the most common malignant brain tumor for children and glioblastomas are the most common malignant brain tumor for adults. Both tumors are difficult to treat, and new therapies are urgently needed for these cancers.
Our laboratory uses large-scale genomic approaches to locate and analyze the genes that are mutated during brain cancer development. The technologies we now employ are capable of searching nearly all of a cancer genome for molecular alterations that can lead to cancer. The new molecular targets for cancer therapy are first located by large scale gene expression analysis, whole-genome scans for altered gene copy number and high throughput sequence analysis of cancer genomes. The alterations we find are then studied in-depth to determine how they contribute to the development of cancer, whether it is promoting tumor growth, enhancing the ability for the cancer to invade into normal tissue, or preventing the various fail-safe mechanisms programmed into our cells.
Our goal is to find the critical new functions that the tumor gains by a new mutation and if counteracting the mutation can slow or stop tumor growth.
In addition to identifying gene mutations and other alterations in brain cancer, we are using this information to develop better brain cancer therapy. This is done in part by screening large chemical libraries to identify small molecules that kill or halt growth of mutation containing cells. Many of these small molecules may have properties that may allow them to be developed into useful drugs. These potential drugs are being tested in experimental systems as potential therapies for brain cancer.
The positive impact on patient survival and quality of life is our major long-term goal.
Current Projects
Our projects are in two main areas of brain cancer research. Our first goal, since the inception of the laboratory, has been to identify genes that cause brain cancers. In particular, we have identified genes that are part of the basis of the formation of glioblastomas and medulloblastomas. Starting about four years ago, we sought practical applications for our research and embarked on an ambitious plan to identify new and better anti-cancer drugs. Our goal is to target the molecular changes that result in brain and other cancers. This work includes screening small molecules for new leads.
Cancer Genomics
Cancers, including brain cancers, arise due to deleterious changes to DNA — the genetic material that provides life instructions to our cells. The most common and easily recognized DNA alterations are mutations that alter a protein-coding sequence within the one of the 20,000 plus genes in our DNA. These mutations, along with other genetic and epigenetic changes, then in turn alter the amount and sequence of the RNA and protein expressed in a cancerous cell.
Gene Expression
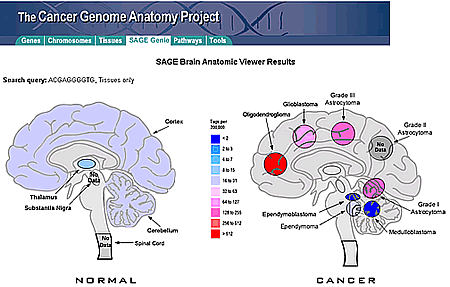 This image shows an example from the ‘SAGE Genie Anatomic viewer’ of a gene that has high expression only in glial tumors.
This image shows an example from the ‘SAGE Genie Anatomic viewer’ of a gene that has high expression only in glial tumors.Many of our projects use the latest techniques to measure gene expression in malignant cells and experimental systems we engineer to study cancer related genes. Studying the transcripts expressed in cancer cells was the first functional genomics tool we have applied to studying cancer cells. As part of this work, our lab organized the Cancer Genome Anatomy Project’s SAGE database known as SAGE Genie. SAGE Genie is one of the largest and most commonly used Cancer Gene Expression Databases.
Some of our projects are now trying to determine why certain genes are over-expressed in brain cancers, compared to normal brain, and evaluating if these genes are good therapeutic targets.
High-throughput Mutation Screens
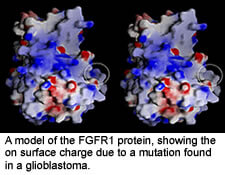
Of particular interest to our lab is the identification of cancer-causing gene mutations.
We have already identified new mutations in kinase genes (FGFR1 and PDGFRA) that are probably genetic changes that lead to tumor formation in glioblastomas. This work is published in PNAS.
Using Digital Karyotyping — a technique to map amplifications and deletions in high resolution along the entire genome — we found that the OTX2 gene is amplified in some medulloblastomas. Using SAGE we also found it was overexpressed in about 60% of medulloblastomas. We are currently working on the functional and therapeutic implications of this medulloblastoma oncogene. We are currently scaling up to perform larger screens for brain tumor mutations.
Starting in 2006, we now have NIH funding to support a genomics project for high-throughput screens of glioblastoma genomes.
This Glioblastoma Genome Project is in conjunction with the Venter Institute.
Drug Screens and Evaluations
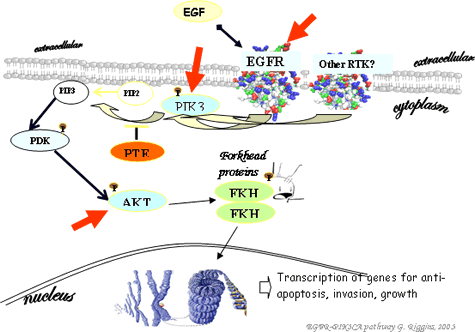 Transcription of genes for anti-apoptosis, invasion, growth
Transcription of genes for anti-apoptosis, invasion, growthA major goal of our laboratory is to identify small molecules that inhibit the mutations that we identify in our cancer genomics projects. Starting with known medicinal compounds, we are studying which compounds and modes of delivery might be best for inhibiting glioblastomas and medulloblastomas. Often there are no effective drugs for inhibiting the pathways and mutations we find altered in brain cancers.
Due to this dire need for new and useful drugs, we have started our own small-molecule screening program. We have assembled over 30,000 different pure small molecule compounds in the laboratory, and use these for high-throughput cell based screen. Using cells engineered with cancer-causing mutations and reporter systems that can be adapted to high throughput screens, we have already identified several leads that inhibit genes in the EGFR and AKT pathways. In addition to the small molecule screens we are collaborating with Research Triangle Institute and Mycosynthetix to screen a diverse natural compound library.
Education and Training
-
We routinely have positions open in the laboratory for highly qualified scientists interested in brain tumor research, cancer genomics and/or new drug development. At present, all of our laboratory positions are filled, but please check back here in the future for updates.
-
Excellent dissertation projected opportunities exist in our laboratory for brain cancer research. Students currently enrolled in the any of the Johns Hopkins University School of Medicine Graduate programs are welcome to plan research rotations within our laboratory. Students in the MD/PhD program or graduate programs of Biochemistry, Cellular & Molecular Biology, Biomedical Engineering, Cellular & Molecular Medicine, Health Sciences Informatics, Human Genetics & Molecular Biology, Neuroscience, Pathobiology, Pharmacology & Molecular Sciences, Program in Molecular and Computational Biophysics or any of the programs are welcome to discuss the research opportunities in the laboratory.
Dr. Riggins has joint appointments in the Neurosurgery, Oncology and Genetic Medicine departments, and is currently applying for membership to graduate training program(s).
-
Our laboratory provides opportunities for clinical fellows seeking a research project in brain cancer laboratory research. Projects span from cancer gene discovery to drug testing and development. The Johns Hopkins Department of Neurosurgery provides a two-year research opportunity for residents and this laboratory provides one of many flexible environments for ground-breaking research in neurooncology.
Also at Johns Hopkins, in combination with the NIH, is an NIH funded training grant, Research Training in Neuro-Oncology, which provides a means for clinical fellows to gain new experiences in clinical care and laboratory research.
Lab Members
Avadhut Joshi, PhD
Research Fellows

Ms. Brenda Raymond
Administrative Staff

Our Funding
Our laboratory's efforts to identify new drug targets and develop new molecular based therapies for brain cancer are gratefully supported by the following generous donors, centers and funding agencies:
- The National Cancer Institute
- The National Institute of Neurological Diseases and Strokes
- The Ludwig Center at The Johns Hopkins University (Established by the Virginia & D.K. Ludwig Fund for Cancer Research, an affiliate of the Ludwig Institute for Cancer Research)
- The Children's Cancer Foundation
- The Johns Hopkins Department of Neurosurgery
Dr Gregory Riggins is the inaugural recipient of the Irving J. Sherman, M.D. Research Professorship in Neurosurgery Research. Dr. Sherman is a retired Neurosurgeon who trained under Dr. Walter Dandy at Johns Hopkins. Dr. Sherman graduated from the School of Medicine in 1940 and from the School of Arts and Sciences in 1936. The Professorship was established in 2002 by Florence Sherman, in honor of her husband.
Contact Us
Gregory J. Riggins, M.D., Ph.D.
Irving J. Sherman M.D. Neurosurgery Research Professorship Recipient
Associate Professor of Neurosurgery, Oncology & Genetic Medicine
Johns Hopkins University, CRB II Rm. 257
1550 Orleans Street
Baltimore, MD 21231
E-mail: [email protected]
Phone: 410-502-2905
Fax: 410-502-5559

