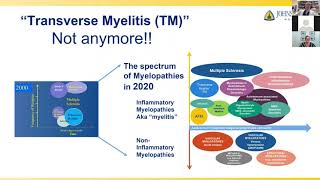
The Johns Hopkins Myelitis and Myelopathy Center, formerly the Transverse Myelitis Center, was the first center in the U.S. and the world dedicated to the diagnosis, management and research of transverse myelitis. We have since expanded our focus to cover the full spectrum of myelitis and myelopathy disorders, both in adults and children. Our goal is to help patients maximize treatment, recovery and daily function as we conduct research to a gain better understanding of these debilitating diseases.
Conditions We Treat
- Transverse myelitis (idiopathic, metabolic, infectious, and post-infectious)
- Acute flaccid myelitis
- Compressive and spondylotic myelopathies
- Encephalomyelitis
- Myelin oligodendrocyte glycoprotein (MOG) antibody associated disease (MOGAD)
- Neuromyelitis Optica Spectrum Disorder (NMOSD)
- Spinal cord strokes
- Vascular myelopathies
Expert Care for Patients with Myelopathies
Neurologic Care for Newly Diagnosed
We help newly diagnosed patients who are going though an acute phase of the disease and need expert neurological care. Our team will also work with you to create a plan for long-term symptoms management.
Multi-Specialty Symptom Management
We also help people who have lived with myelopathy for some time and are looking to better manage symptoms and improve quality of life. We will connect you with Johns Hopkins experts in rehabilitation, pain medicine and other fields and will help you build a custom care plan.
Appointment Information
In case of an emergency, please contact 911 and/or go to the nearest hospital. Otherwise, please use the following information to schedule an appointment with or refer a patient to the Johns Hopkins Myelitis and Myelopathy Center.
When you call 410-614-1522 to request an appointment at our center, our call center staff will ask you a few questions and will request you to send relevant medical records. Please have the following information ready before you call:
- Notes from emergency department and/or hospital admission concerning your neurological diagnosis.
- Clinic notes from neurological assessments.
- Laboratory results including blood work and cerebrospinal fluid results.
- Images of MRI studies of the brain and spine, angiograms. You can upload the digital images to AMBRA.
- Any other significant clinical documents concerning your diagnosis.
- Contact information, including cellphone, home phone and e-mail.
- Front and back of your insurance card.
If you do not have a confirmed diagnosis of myelopathy, you will be referred for an evaluation with a general neurologist outside of our center. If your myelopathy diagnosis is confirmed, we will see you in our clinic.
2022 Research Update: Multiple Sclerosis, Myelitis and Myelopathies and Neuromyelitis Optica
Our center conducts numerous research studies on myelopathies, looking to improve diagnosis and treatment. Drs. Carlos Pardo, Ellen Mowry, Peter Calabresi and Shiv Saidha offer an overview of what’s new in clinical research related to transverse myelitis, multiple sclerosis and other myelopathies, including the effects of COVID-19 on people who have these conditions.
View our published researchOur Research Publications
-
- Evidence for and against subclinical disease activity and progressive disease in MOG antibody disease and neuromyelitis optica spectrum disorder. Molazadeh N, Filippatou AG, Vasileiou ES, Levy M, Sotirchos ES. J Neuroimmunol. 2021 Nov 15;360:577702. doi: 10.1016/j.jneuroim.202577702. Epub 2021 Aug 26.
- Optic Neuritis-Independent Retinal Atrophy in Neuromyelitis Optica Spectrum Disorder. Filippatou AG, Vasileiou ES, He Y, Fitzgerald KC, Kalaitzidis G, Lambe J, Mealy MA, Levy M, Liu Y, Prince JL, Mowry EM, Saidha S, Calabresi PA, Sotirchos ES. J Neuroophthalmol. 2021 May 17. doi: 10.1097/WNO.000000000000128
- In vivo identification of morphologic retinal abnormalities in neuromyelitis optica. Sotirchos ES, Saidha S, Byraiah G, Mealy MA, Ibrahim MA, Sepah YJ, Newsome SD, Ratchford JN, Frohman EM, Balcer LJ, Crainiceanu CM, Nguyen QD, Levy M, Calabresi PA. Neurology. 2013 Apr 9;80(15):1406-14. doi: 10.1212/WNL.0b013e31828c2f7a. Epub 2013 Mar 20.
- AQP4-IgG and MOG-IgG Related Optic Neuritis-Prevalence, Optical Coherence Tomography Findings, and Visual Outcomes: A Systematic Review and Meta-Analysis. Filippatou AG, Mukharesh L, Saidha S, Calabresi PA, Sotirchos ES. Front Neurol. 2020 Oct 8;11:540156. doi: 10.3389/fneur.2020.540156. eCollection 2020.
- Aquaporin-4 IgG seropositivity is associated with worse visual outcomes after optic neuritis than MOG-IgG seropositivity and multiple sclerosis, independent of macular ganglion cell layer thinning. Sotirchos ES, Filippatou A, Fitzgerald KC, Salama S, Pardo S, Wang J, Ogbuokiri E, Cowley NJ, Pellegrini N, Murphy OC, Mealy MA, Prince JL, Levy M, Calabresi PA, Saidha S. Mult Scler. 2020 Oct;26(11):1360-1371. doi: 10.1177/1352458519864928. Epub 2019 Jul 31.
- Evidence of subclinical quantitative retinal layer abnormalities in AQP4-IgG seropositive NMOSD. Filippatou AG, Vasileiou ES, He Y, Fitzgerald KC, Kalaitzidis G, Lambe J, Mealy MA, Levy M, Liu Y, Prince JL, Mowry EM, Saidha S, Calabresi PA, Sotirchos ES. Mult Scler. 2021 Oct;27(11):1738-1748. doi: 10.1177/1352458520977771. Epub 2020 Dec 14.
-
- Acute flaccid myelitis: cause, diagnosis, and management. Murphy OC, Messacar K, Benson L, Bove R, Carpenter JL, Crawford T, Dean J, DeBiasi R, Desai J, Elrick MJ, Farias-Moeller R, Gombolay GY, Greenberg B, Harmelink M, Hong S, Hopkins SE, Oleszek J, Otten C, Sadowsky CL, Schreiner TL, Thakur KT, Van Haren K, Carballo CM, Chong PF, Fall A, Gowda VK, Helfferich J, Kira R, Lim M, Lopez EL, Wells EM, Yeh EA, Pardo CA; AFM working group. Lancet. 2021 Jan 23;397(10271):334-346. doi: 10.1016/S0140-6736(20)32723-9. Epub 2020 Dec 23. PMID: 33357469; PMCID: PMC7909727.
- Acute Flaccid Myelitis: A Clinical Review. Murphy OC, Pardo CA. Semin Neurol. 2020 Apr;40(2):211-218. doi: 10.1055/s-0040-1705123. Epub 2020 Mar 6. PMID: 32143233.
- Comparative quantitative clinical, neuroimaging, and functional profiles in children with acute flaccid myelitis at acute and convalescent stages of disease. Gordon-Lipkin E, Muñoz LS, Klein JL, Dean J, Izbudak I, Pardo CA. Dev Med Child Neurol. 2019 Mar;61(3):366-375. doi: 10.1111/dmcn.14030. Epub 2018 Sep 17. PMID: 30225922.
-
- Diagnostic Criteria for Neurosarcoidosis: From the Neurosarcoidosis Consortium Consensus Group. Stern BJ, Royal W 3rd, Gelfand JM, Clifford DB, Tavee J, Pawate S, Berger JR, Aksamit AJ, Krumholz A, Pardo CA, Moller DR, Judson MA, Drent M, Baughman RP. Definition and Consensus JAMA Neurol. 2018 Dec 1;75(12):1546-1553. doi: 10.1001/jamaneurol.2018.2295. PMID: 30167654.
- Clinical and MRI phenotypes of sarcoidosis-associated myelopathy. Murphy OC, Salazar-Camelo A, Jimenez JA, Barreras P, Reyes MI, Garcia MA, Moller DR, Chen ES, Pardo CA. Neurol Neuroimmunol Neuroinflamm. 2020 Apr 8;7(4):e72 doi: 10.1212/NXI.0000000000000722. PMID: 32269072; PMCID: PMC7176244.
-
- Transverse Myelitis: pathogenesis, diagnosis and treatment. Krishnan C, Kaplin AI, Deshpande DM, Pardo CA, Kerr DA. Front Biosci. 2004 May 1;9:1483-99. doi: 10.2741/135 PMID: 14977560.
- Clinical biomarkers differentiate myelitis from vascular and other causes of myelopathy. Barreras P, Fitzgerald KC, Mealy MA, Jimenez JA, Becker D, Newsome SD, Levy M, Gailloud P, Pardo CA. Neurology. 2018 Jan 2;90(1):e12-e21. doi: 10.1212/WNL.0000000000004765. Epub 2017 Dec 1. PMID: 29196574; PMCID: PMC5754646.
-
- MOGAD: How It Differs From and Resembles Other Neuroinflammatory Disorders. Shahriari M, Sotirchos ES, Newsome SD, Yousem DM. AJR Am J Roentgenol. 2021 Apr;216(4):1031-1039. doi: 10.2214/AJR.20.2406 Epub 2021 Feb 17.
-
- Spinal fistulas documented by contrast enhanced computed tomography during myelopathy workup: a lost opportunity. Hedjoudje A, Murphy OC, Gregg L, Pardo CA, Gailloud P. Neuroradiology. 2021 Feb;63(2):201-207. doi: 10.1007/s00234-020-02601-x. Epub 2020 Nov 16. PMID: 33196864.
- Analysis of 30 Spinal Angiograms Falsely Reported as Normal in 18 Patients with Subsequently Documented Spinal Vascular Malformations. Barreras P, Heck D, Greenberg B, Wolinsky JP, Pardo CA, Gailloud P. AJNR Am J Neuroradiol. 2017 Sep;38(9):1814-1819. doi: 10.3174/ajnr.A5275. Epub 2017 Jul 20. PMID: 28729296; PMCID: PMC7963703.