Remembering Andrew
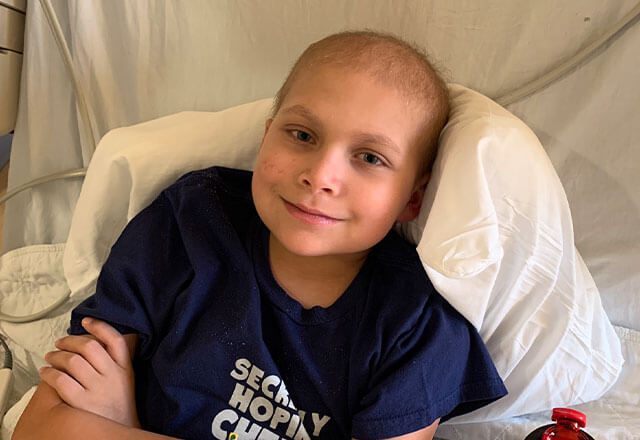
When her son, Andrew, came home from school one day and fell right to sleep, Colleen figured he was coming down with a fever. Usually the class clown and full of energy, he just wasn’t himself. At urgent care, Andrew tested positive for strep throat, and he didn’t bounce back from it like most children do.
Andrew’s health fluctuated, and his pediatrician confirmed he had the flu, but nothing explained the red, veiny marks that appeared on his body. Andrew’s parents took him to get his blood tested, and they got a phone call: Three days before his 10th birthday, Andrew needed to go immediately to Johns Hopkins Children’s Center. The blood work showed that he had acute lymphocytic leukemia.
Colleen remembers Andrew crying, not because of the hospital and not because he was sick, but because he had to miss his birthday party. His parents assured him everything would be OK.
Andrew was an inpatient at Johns Hopkins Children’s Center for more than two weeks, and he spent the next several months in and out of inpatient care during his treatment plan.
“At one point he did ask us, ‘Am I going to die?’” Colleen recalls. “And of course, our answer was always no. Leukemia is very curable.”
Two months in, his doctors at Johns Hopkins made a shocking discovery. Andrew had Burkitt lymphoma. He had been born with a genetic alteration predisposing him to development of the disease, and detection had snuck by until then — the Burkitt lymphoma had been hidden by the leukemia. Andrew was the 13th person in the world with this anomaly.
Doctors tried chimeric antigen receptor (CAR) T-cell therapy, a new experimental treatment that uses the body’s own blood to create enhanced T-cells that can, when put back into the bloodstream, attach to cancerous cells and destroy them. The therapy seemed effective for Andrew, but the Burkitt lymphoma evaded the treatments. One week after Andrew was deemed cancer free, cancerous cells were again found in his body.
While a continuation of this course of drug could have very well been successful, by that point, Andrew was entering into organ failure. The doctors hoped to place him on dialysis for his kidneys, but his body was retaining too much fluid, which would have to be removed first. Surgery was suggested and the family agreed.
Everyone tried until the last moment to save Andrew from his illness, but he never woke up from his surgery. On Dec. 14, parents Colleen and Paul laid next to Andrew in his hospital bed, and they spent their last night together as a family. Colleen made a last request of her baby: “Let me know when you’re in heaven.” At 3:15 a.m. on Dec. 15, Andrew took his last breath. Away from the bed, far out of reach, Colleen’s phone suddenly played music, and Andrew’s parents knew their son was telling them he’d finally found peace.
Andrew’s primary oncologist joined Colleen and Paul as they brought the boy into the halls, and the Children’s Center staff members, who all loved his sunny disposition, gave the brave child his final salute.
The family agreed to a full autopsy. Paul and Colleen hope the CAR T-cell treatment can be supported and can grow so that it’s the first treatment used for children like Andrew. They know there’s progress to be made, and they believe Andrew’s life served a mighty purpose by helping to further leukemia and Burkitt lymphoma research.
“He loved to make the other kids laugh,” Colleen remembers. “Andrew’s legacy is making other pediatric oncology warriors laugh when there’s not much to laugh about.”
“We consider his whole team to be family,” Paul says about Johns Hopkins. “Any support Johns Hopkins receives makes the patient’s treatment better, it makes their time in the hospital easier. Really, it makes the worst time in their lives a little bit easier.”

