Small Animal Cardiovascular Phenotyping and Model Core
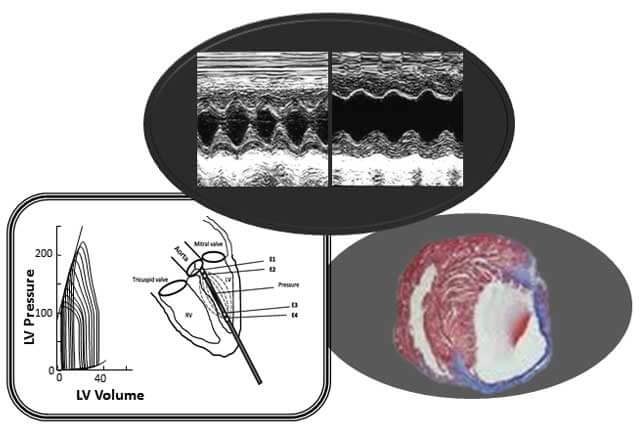
The Core Lab provides small animal cardiovascular phenotyping and model core for cardiovascular research.
Heart Function and Geometry by Ultrasound and Doppler Imaging
In This Section:
- Heart Disease Models
- Chronic Electrocardiographic Telemetry
- Pressure Volume Loops
- EchoDoppler Studies
- For other potential services, please contact Dr. Nadan Wang.
Heart Disease Models
We provide a variety of surgically generated heart disease models for use in mice or rats. This includes aortic or pulmonary artery banding for pressure-overload, myocardial infarction or ischemic reperfusion models of the left ventricle, and osmotic pump implantation for delivery of pharmaceuticals.
Our services include:
-
This is performed via a limited supraclavicular access incision, using direct suture placed around the transverse aorta. Varying levels of severity are offered. Our severe TAC model generates gradients of about 50-60 mmHg, and generally produces substantial hypertrophy and chamber dilation by 1 week.
These hearts develop rapid and early systolic dysfunction. A moderate level of TAC generates more compensatory hypertrophy without dilation by 1 week, more gradual dilation by 3 weeks, and can ultimately lead to some systolic dysfunction by 6 weeks. General survival rates range in the 75-80% range, with mortality typically occurring in the first week.
-
The proximal or mid left anterior descending artery of the left ventricle is ensnared using a small suture, and permanently ligated. This surgery yields a 1-week mortality rate of ~35% in normal mice, generally due to chamber dilation and wall rupture, and occurring in the first several days after the procedure.
-
This is similar to service B, only the ligation is provided for 45 minutes only, and then the artery is allowed to reperfuse. Mortality is reduced substantially, though there is somewhat more variability with the extent and distribution of the infarction injury.
-
Similar to aortic constriction, but with a suture band placed around the proximal pulmonary artery to generate pressure overload for the right ventricle.
-
Implantable pumps are filled with reagents per investigator and are inserted to provide 2-4 weeks of continuous intravenous or intraperitoneal drug delivery. Additional charges are made for the pumps themselves if the investigator cannot provide these, and drug must be provided by the investigator.
Chronic Electrocardiographic Telemetry
Electrocardiographic recordings from implantable transmitters are available via this service. Data Scientific systems are used, and data for multiple days (depending on need) based on telemetry provided.
Pressure Volume Loops
Analysis of Right or Left Heart Function
A miniature pressure-volume catheter is inserted into the relevant ventricle to measure in situ cardiac function using pressure-volume relationships. This is used to assess ventricular pressures, systolic and diastolic function, relaxation rates, filling rates, load-independent contractility parameters, diastolic compliance, and other indexes. These studies are not designed to be survival surgeries.
Our services include:
-
This can be performed via an intravenous or carotid access, or by ventricular apical catheter placement in an open chest configuration.
-
This is performed using the combined pressure-volume catheter. Data can be provided with full calibration – that is volumes are calibrated to provide absolute values – or are kept as relative volumes. Investigators can discuss their needs with the Core to determine which is appropriate for their study.
-
This is similar to a basic pressure volume assessment, only in this case interventions with multiple calculations are performed. Interventions could be delivery of a drug at one or two doses, pacing heart rate or sub-acute aortic banding.
EchoDoppler Studies
Functional assessment of the heart and major blood vessels is provided by this service. Images are generated using one of two systems – a Accuson Sequoia echo-Doppler system or a state-of-the-art Visual-Sonics Vevo 2100 imaging system. The first is useful for routine M-mode and 2-D imaging, and for flow Doppler assessments.
The latter provides higher resolution imaging and also has tissue Doppler capabilities including speckle tracking for regional strain analysis. It would be the preferred imaging method for hearts with regional wall motion abnormalities, and when more subtle changes in function are anticipated. Functional imaging is also available to assess aortic diameter and wall thickening, flow in the aorta to assess vascular stiffening (pulse wave velocity, velocity time integral used to determine cardiac output, etc.).
Our services include:
-
This determines chamber dimensions, fractional shortening, wall thickness, and estimated wall mass and ejection fraction (cylindrical model).
-
Comprehensive M-mode and 2-D imaging determines cardiac function, volumes and ejection fraction, cardiac output, and more detailed morphometry.
-
Doppler Flow imaging assesses systolic and diastolic function based on flow ratios, timing intervals, cardiac output, etc.
-
Tissue Doppler imaging determines diastolic and systolic function, including myocardial performance index, isovolumic contraction indices, etc.
-
2-D Speckle tracking for regional strain assessment.
Price List
Contact us for the Small Animal Cardiovascular Phenotyping and Model Core price list.
Contact
Nadan Wang
410-502-2044
[email protected]
Michelle "Missy" Leppo
410-955-3814
[email protected]
Shi Pan
410-502-2044
[email protected]
David Kass
410-955-7153
[email protected]
