What is ECMO?
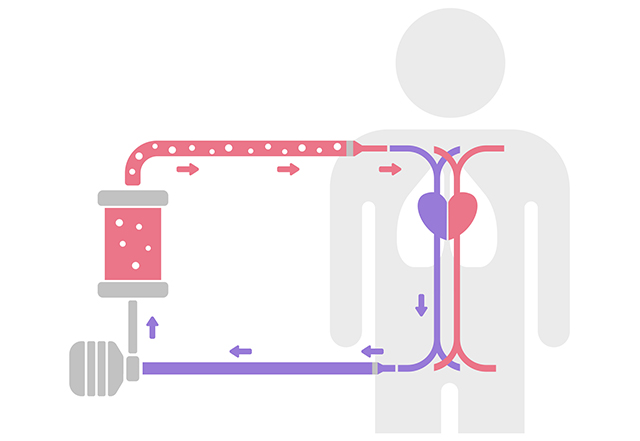
Extracorporeal membrane oxygenation (ECMO) is a short-term device that provides support to vital organs when the heart and lungs are failing.
An ECMO machine runs 24 hours a day. It allows blood to flow to the machine and back in a closed circuit, returning oxygenated blood to the body similar to how your heart pumps. This allows the heart and lungs to rest temporarily. The ECMO team, adjusts the machine to support your loved one throughout the day, ensuring they receive the best possible care.
On This Page
ECMO for COVID-19:
COVID-19 can cause lung damage, and in severe cases, may cause the lungs to stop working. For some patients, VV ECMO may be used as temporary life support to evaluate lung recovery. Patients on VV ECMO for COVID-19 may have different needs and goals than patients on ECMO for other reasons. In addition, visitation may be intermittently restricted during their hospital stay due to the COVID-19 infection.
Conquering COVID: Maria's Story
In October 2020, Maria Young — an active 41-year-old woman — arrived at The Johns Hopkins Hospital in Baltimore, Maryland, with COVID-19 and double pneumonia. A staggering 130 days later, Maria returned to her family. At the hospital, she spent 69 days on ECMO and more than 100 days on a ventilator.
Frequently Asked Questions
-
Seeing your loved one undergo ECMO therapy can cause difficult emotions. Your ECMO care team will ensure your loved one is well taken care for and comfortable. You can expect to see the following care measures:
Chest x-rays:
Your loved one will undergo chest x-rays throughout their therapy to monitor the function of their lungs and heart.IV or Tube Feeding:
Your loved one won't be able to eat normally when undergoing ECMO therapy. When undergoing ECMO, oxygen is conserved and sent to the most vital organs. Depending on the condition of your loved one, the team may decide to insert an IV or place a temporary feeding tube to provide nutrition.Medications:
ECMO is a lifesaving therapy that gives your loved one time to heal from heart and lung failure. Your loved one may receive many medications including antibiotics to reduce infection, pain medication to keep them comfortable, and diuretics to help kidneys produce urine.Tubes and ECMO machine:
Your loved one will have many tubes inserted into their body to help the ECMO machine circulate blood and oxygen from the ECMO machine to different areas of the body.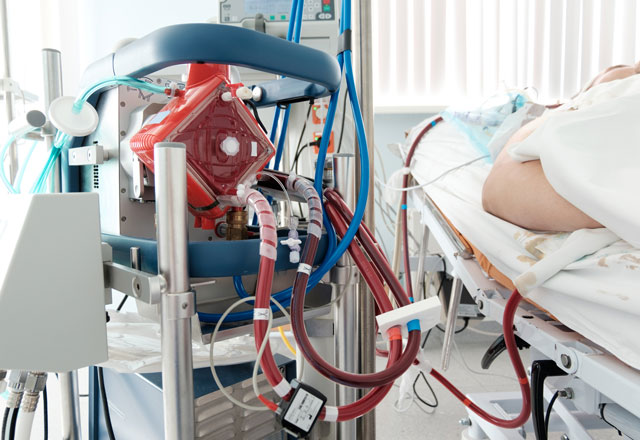
-

Your loved one will be cared for by experienced ECMO specialists which includes:
- Cardiothoracic and vascular surgeons
- ICU doctors (intensivists)
- Nurse practitioners
- Physician assistants
- Perfusionists
- Pulmonologists
- Registered nurses
- Respiratory therapists
- ECMO specialists
-
You and your family are encouraged to take care of your mental health and visit your loved one. Some family members like to interact with their loved one whether that's reading to them, bringing in their favorite music or familiar items.
Waiting rooms are available throughout the 5th floor, please ask the unit clinical customer service representative if you need any assistance.
-

ECMO can be stressful and upsetting to you and your family. It's important to take time to rest and take breaks from visitation at times in order to practice self-care. Case managers and social workers are on staff to assist and support you. We encourage you to seek counselling or psychiatric help if you and your family feel that it is needed. This experience can be very difficult for many people.
We are available to provide supportive resources and help you navigate this difficult time.
-
There are several risks that range from common to uncommon when your loved one is on an ECMO machine:
- Bleeding: Patients are often required to be on blood thinners for the ECMO machine to work best. This may cause patients to bleed from wound sites or internally.
- Infection: Infection is a common risk for patients who undergo ECMO therapy.
- Problems with ECMO equipment: The ECMO equipment is monitored by the perfusion team. In the rare instance of equipment failure, the team is trained in emergency situations.
- Stroke/blood clots: There is a risk of small blood clots and/or air bubbles forming in the tubing or blood vessels which can lead to a stroke.
-
Your loved one may be removed from ECMO once their lungs and/or heart have improved. Once the ECMO machine is turned off, the tubes are removed in the operating room or ICU.
Placement of ECMO support is very serious, and it may be used as a means to give your loved one's vital organs more time to recover after failing.
Sometimes we place people on the ECMO machine to allow family and loved ones time to meet and make important decisions. The whole family may be required to make difficult decisions regarding your loved one's care as not all patients who undergo ECMO make it to recovery.
-
After your loved one is removed from ECMO, they may be placed in the Intensive Care Unit (ICU) on a ventilator until they are able to breathe on their own and their heart's function has improved. Before being discharged, your loved one will need to have good vital signs and is able to eat without difficulty. It may take several days or weeks for your loved one to return to normal depending on their condition.
Your ECMO care team will monitor your loved one and provide guidance on their recovery.
-
ECMO is not a treatment, but a supportive therapy. While ECMO is utilized to help our patients recover or seek the next appropriate intervention, not all patients make it to the next phase of care. The whole family may be required to have some very difficult discussions with the team and form decisions regarding your loved one’s care. The decision may be made to discontinue ECMO support and will be done in the patient’s room with the family present, if that is the family’s wishes.
-

We are here to support you and your loved one through a difficult time. Your ECMO care team will be available to answer any questions you may have and provide support during your loved ones care.
Johns Hopkins palliate care team are also available and can be accessed 24/7.
For more information on ECMO, visit the following websites:
You are being redirected to a website outside Johns Hopkins for informational purposes only. Johns Hopkins is not responsible for any aspect of the external website.