COVID Test FAQs
Reviewed By:
Testing is an important tool in helping to limit the spread of COVID-19. Lisa Maragakis, M.D., M.P.H., senior director of infection prevention, answers common questions about testing.
What are the types of coronavirus tests?
There are two basic types of tests for COVID-19.
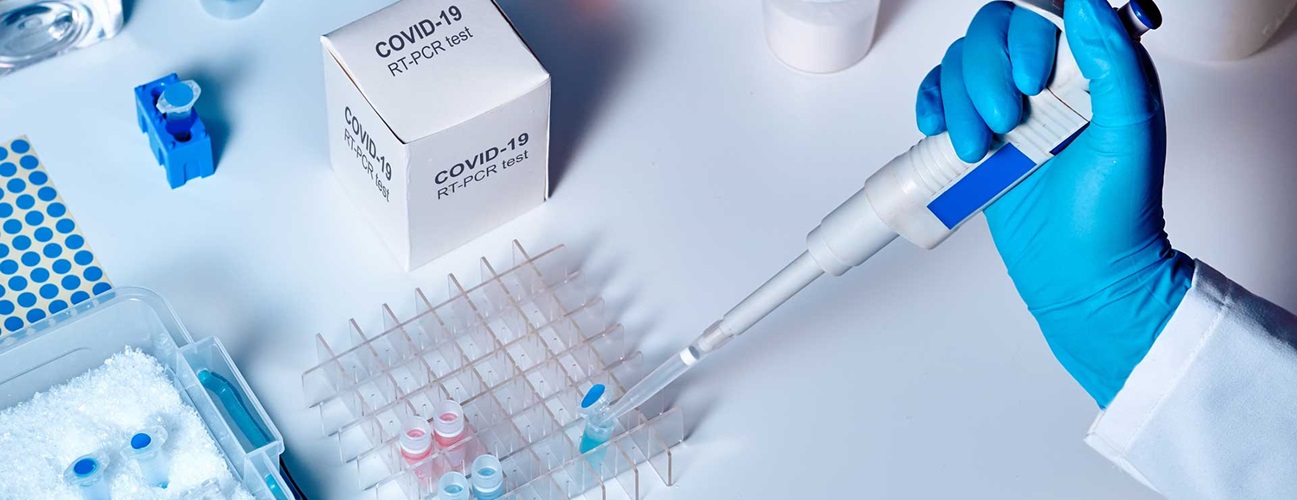
Viral test: This test can tell you if you are currently infected with the coronavirus. A swab is placed in the nose or mouth to gather samples. There are two types of viral tests: laboratory tests (sometimes called polymerase chain reaction [PCR] tests), and rapid tests that detect portions of the virus called antigens.
Laboratory coronavirus tests are given by health care professionals, and results may take a day or more to receive. Since the samples are analyzed in a laboratory, they are very accurate and are often recommended for people with COVID-19 symptoms. Laboratory tests sometimes require an additional test to confirm results.
Due to the rapid spread of COVID-19 in the community, Johns Hopkins Medicine is only offering COVID-19 testing under certain conditions. Review our COVID-19 testing information to learn more.
Rapid antigen tests may be performed in pharmacies or health care facilities, or as self-tests at home. Rapid tests provide results in about 15 minutes. These tests are recommended if you do not have symptoms or if you are taking the test as a risk-prevention measure, such as before going on a work trip or seeing a friend, and you want to be sure you don’t have the coronavirus that causes COVID-19.
Antibody test: This is a blood test that can show if you were previously exposed to or infected with the virus that causes COVID-19, and if your body has created antibodies in an attempt to defend itself. It takes at least 12 days after exposure for your body to make enough antibodies to show up on a test. Antibody tests are not recommended to determine if you currently have COVID-19.
This test helps scientists gather data about how the immune system fights off COVID-19 in recovered patients. A positive antibody test means the person has some level of immune protection either from prior infection or from vaccination, but it is not a guarantee of protection from getting re-infected with the virus. Antibody levels decrease over time, and it is not clear how long antibody protection lasts.
Should I get a coronavirus test?
The answer varies based on many factors including your symptoms, exposure history and underlying risk factors for severe disease.
A rapid test is useful as a preventive measure if you are traveling or if you do not have symptoms but think you may have been exposed to the coronavirus that causes COVID-19. Other important prevention tools are: getting fully vaccinated and receiving a booster when eligible, wearing a mask, maintaining physical distance and frequently washing your hands.
A viral test is important when a person has COVID-19 symptoms, particularly if they are moderate to severe. A viral test may also be helpful for a person with mild symptoms. People with any symptoms should contact their doctor and review Centers for Disease Control and Prevention (CDC) guidelines for isolation and quarantine.
Where can I get a coronavirus test?
Demand for tests is currently high, so you may need to check several resources. Testing sites may include your doctor’s office, a local urgent care facility or a testing location in your area. Maryland.gov provides a list of test locations. You may also be able to get self-tests at selected pharmacies or health care centers.
Due to the high demand, Johns Hopkins Medicine only offers COVID-19 testing under certain conditions. Review our COVID-19 testing information to learn more. We urge people not to go to emergency rooms for routine COVID testing, so that Emergency Department staff are available to prioritize care for patients with urgent or emerging medical needs.
How long do COVID test results take?
Laboratory analysis of viral tests (sometimes called PCR tests) can take a day or more. Rapid test results are available in about 15 minutes. Antibody test results may take a day or longer to obtain.
If I’ve been tested once, do I need to get tested again?
A negative COVID-19 test result reflects only one point in time, so it may be necessary to test more than once if you develop symptoms or were potentially exposed to the virus. If you are tested during the earliest stages of infection, before the virus is detectable, you might be infected despite having a negative test result. And after receiving a negative test result, it is possible to catch the coronavirus later and become infected.
If you are exposed to someone with COVID-19, you should quarantine, watch for symptoms and consider getting tested on day four or five following the exposure. Please review CDC guidelines for isolation and quarantine.
If you have symptoms, let your health care provider know if they persist or worsen. You might need to be tested again.