Basal Cell Cancer of the Head and Neck
Featured Expert:
What is basal cell cancer of the head and neck?
Basal cell cancer is the most common form of skin cancer, accounting for nearly 80% of all skin cancers. Basal cell cancers arise from abnormal basal cells in the skin. It is rarely fatal, but it can be locally aggressive.
What are the symptoms of basal cell cancer of the head and neck?
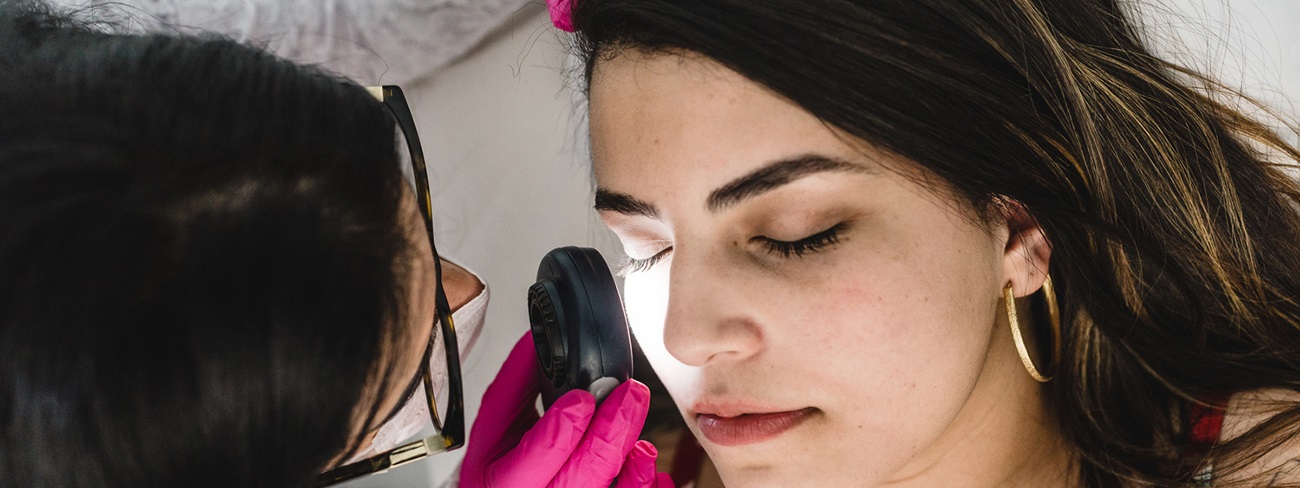
Basal cell cancers usually present as an abnormal growth on the skin. The growth may have the appearance of a wart, crusty spot, reddish patch, mole, nodule or bump, or a sore that does not heal. It may or may not bleed and can sometimes be painful. These are usually slow-growing tumors that begin as small spots on sun-exposed areas of the face. Because they can have such a range of appearances, any new persistent skin lesion should be evaluated.
Johns Hopkins Head and Neck Cancer Specialists

Our head and neck surgeons and speech-language pathologists take a proactive approach to cancer treatment. Meet the Johns Hopkins specialists who will work closely with you during your journey.
What are the risk factors for basal cell cancer of the head and neck?
- Sun exposure.
- Tanning bed exposure.
- Fair skin.
- Age over 50 years.
- A history of skin cancer.
- A previous burn.
- Prior radiation to the head and neck area.
- Immunosuppression, either from a medical condition or by medications (such as those taken by transplant patients).
UV radiation exposure from the sun or tanning beds is responsible for 90% of basal cell cancers.
How is basal cell cancer of the head and neck diagnosed?
Diagnosis is made by clinical exam and a biopsy. Basal cell cancers are staged by size and extent of growth. These cancers rarely metastasize to lymph nodes or other organs, but they can grow quite large and invade small nerves and local structures.
Biopsy can help determine if the basal cell cancer is a low-risk tumor or a high-risk tumor that requires more aggressive treatment. Low-risk tumors are often nodular and do not have nerve involvement. High-risk tumors in the head and neck are those that involve the central face, nose and eye area, as well as those tumors that are greater than or equal to 10 millimeters on the cheeks, scalp and neck; tumors that are recurrent or arising from previously radiated tissue; and tumors arising in patients who are immunosuppressed. An aggressive growth pattern on the pathology evaluation and perineural invasion (nerve involvement) are also features of high-risk basal cell cancers.
Basal Cell Cancer of the Head and Neck Treatment
Surgery is the preferred method of treatment for basal cell cancer. Radiation is an alternative when surgery is not desirable because of cosmetic concerns or medical reasons. Many early stage small basal cell cancers can be removed by Mohs surgery, which is a technique that spares normal tissue through repeated intraoperative margin testing, removing only the cancer and leaving adjacent normal tissue. Excision, curettage and desiccation, and cryosurgery can also be used to remove the cancer while sparing normal tissue. Large tumors and tumors with nerve or lymph node involvement are not suitable for Mohs surgery and require a multimodality approach to treatment with formal surgical resection and adjuvant radiation or chemotherapy. Larger tumors require reconstruction, which can be done at the time of surgery if margin status is clear.
Patients with high-risk tumors should meet with a radiation therapist to discuss postoperative radiation. In patients with high-risk tumors who are not surgical candidates, systemic treatment with chemotherapy that inhibits the Hedgehog pathway of tumor progression has been shown to be effective. Such cases require multidisciplinary care by a team of surgeons, radiation oncologists and medical oncologists.
Johns Hopkins Head and Neck Cancer Surgery

Our team offers comprehensive treatments for cancers affecting the nasal passages, sinuses, the throat and nearby areas. Our head and neck surgeons work closely with medical and radiation oncologists, endocrinologists and other specialists to provide well-rounded care.