BMI Assessment
Body Mass Index (BMI) Assessment
There are different ways to assess weight and obesity risk among children. The most common is body mass index (BMI).
BMI offers an estimate of a person’s risk for obesity based on his or her weight relative to height. BMI is not perfect, yet it is the most practical screening tool available to providers.
While BMI does not measure body fat directly, research has shown that BMI is closely associated with more direct measures of body fat, such as skinfold thickness, bioelectrical impedance, densitometry (underwater weighing), and dual energy X-ray absorptiometry (DXA).
Here are the BMI categories for children age 2 to 20 based on percentile. To assess weight status for infants younger than age 2, use the Centers for Disease Control and Prevention (CDC) and World Health Organization (WHO) growth charts.
Body Mass Index Categories in Children Ages 2 to 20
- Underweight: < 5th percentile
- Healthy weight: 5 to 84th percentile
- Overweight: 85 to 94th percentile
- Obesity: 95 to 99th percentile or BMI > 30
- Severe obesity: > 120 percent of the 95th percentile or BMI > 35 kg/m2
Measure BMI and weight at all wellness visits. BMI results that cross major percentiles merits anticipatory guidance at a minimum.
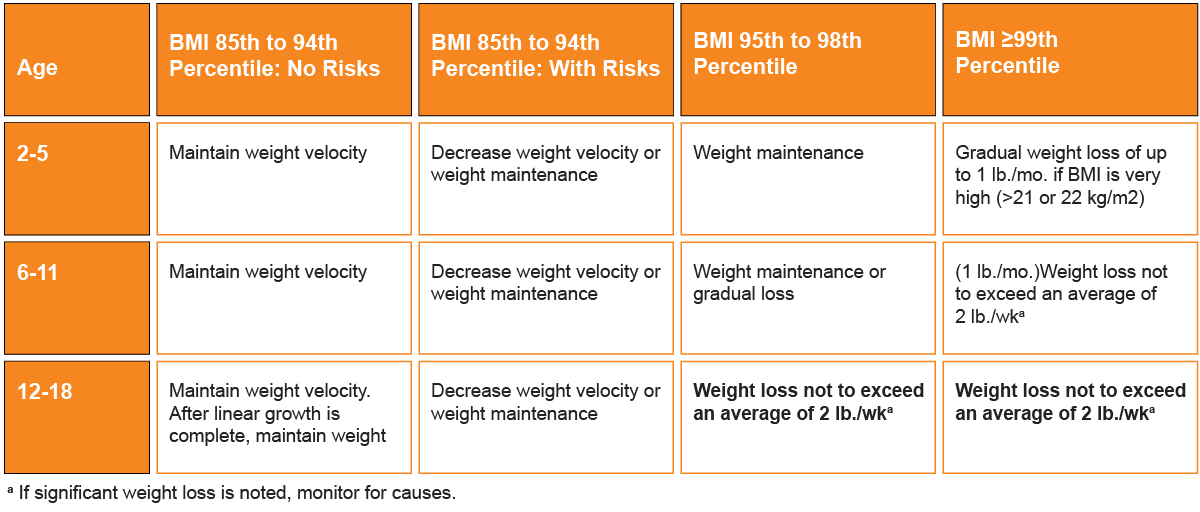
Weight loss targets
The following table adapted from the AAP Healthy Weight Initiative is a guide to help manage overweight and obese children based on their BMI results. Advise parents that short-term weight loss for their children does not always predict long-term success. Generally, behaviors that target dietary changes should be part of any wellness strategy since they have the most immediate effect on weight loss management.