Why It’s Vital That All People — Including People of Color — Take Part in Clinical Research Studies
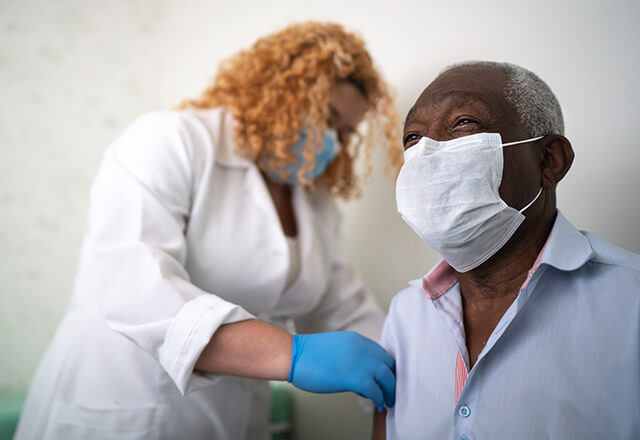
From clinical trials to studies in healthy volunteers, clinical research cannot happen without the help of people who choose to take part in it. Not all people—including people of color, people with disabilities, and others — have been included as often as they should in studies. There are several reasons. It could be because people had limited access to health care or because of biases in the ways studies were designed. It could also be because some people did not trust researchers. To ensure everyone has the chance to be as healthy as possible, the groups of people who participate in medical studies must represent our society at large. Right now, it does not.
As an example. a 2020 report from the U.S. Food and Drug Administration showed:
-
75%
of research participants are white, while white people are 60% of people in the U.S.
-
8%
of research participants are African-American/Black, while African-American/Black people are 13% of people in the U.S.
-
11%
of research participants are Latino/Hispanic, while Latino/Hispanic people are 18% of people in the U.S.
-
6%
of research participants are Asian, while Asian Americans are 6% of people in the U.S.
Johns Hopkins Medicine is actively working to overcome these issues and make sure clinical research includes and benefits all people.
Participation Promotes Medical Equity
Research participants are key to making medical progress. So is diversity among those participants.
To advance equity in health care, it is critical that all people, including people of color, participate in clinical research. The reasons include:
- Race, disability and socioeconomic status, and other demographic factors can affect people’s risk of developing certain conditions. It also can impact their responses to medical interventions and their overall health outcomes. The more that participants who take part in clinical research make up a diverse group, the more likely that the research results — and any decisions to start or stop clinical treatments — will apply to a diverse group of patients.
- It is important that research participants represent the people who are most impacted by the disease or condition being studied. For example, certain cancers and sickle cell disease are much more common among people of color, making it crucial that people of color take part in clinical studies of these serious illnesses.
“We are all more similar than we are different, but there can be differences in how people process medicines,” says Namandje N. Bumpus, Ph.D., director of the Johns Hopkins Department of Pharmacology and Molecular Sciences. “We want therapies to work for as many people as possible. The best way for that to happen is for all people to have access to participate in clinical research.”
How Johns Hopkins Medicine Is Restoring Trust in Clinical Research
Unfortunately, hundreds of years of unethical behavior disguised as medicine has left millions of people of color cynical about medicine and opposed to taking part in medical research. This includes horrific experiments conducted on enslaved people throughout America, to the shameful Tuskegee Study of Untreated Syphilis in Black men.
Collaborating with the Community
Researchers at Johns Hopkins Medicine are working with community leaders to show people of color how things have changed. The Community Research Advisory Council, organized by the Institute for Clinical and Translational Research, is composed of community leaders in the Baltimore area who provide feedback to research teams about how to design and conduct studies in ways that provide value to the entire community. These seminars provide a forum for people to ask questions and have their concerns addressed. Johns Hopkins All Children’s Health also has a community advisory board and Johns Hopkins hospitals in the Washington, D.C. region have members of the community among their Research Review Committees.
Overcoming Bias and Access Issues in the System
Beyond building awareness and restoring trust among people of color, Johns Hopkins Medicine is also working to make it easier for all people to participate in clinical research.
Sometimes the way a study is designed can unintentionally exclude people who are underrepresented in clinical research, including people of color. All clinical trials have a list of characteristics that help define what types of participants to include or not include in a study. This is intended to help show that a treatment is effective in a specific group, such as cancer patients. But if that list is too narrow, certain populations can be left out. Other aspects of a clinical trial—from where the study takes place to the time of day when participants are needed—can also affect people’s involvement.
As one way to help deal with these issues, training is required for all Johns Hopkins Medicine managers and above in unconscious bias. Unconscious bias is prejudice or stereotypes that people form about certain groups that they may not even be aware of. These programs will help people better understand bias in all forms—including racism, sexism and ageism—and how it can be overcome.
To further encourage equity in research, Johns Hopkins Medicine also seeks to improve diversity among the research teams themselves. This includes everything from hiring more scientists of color to making sure people of color hold different positions throughout research teams to recruiting bilingual research staff. This helps make diverse participants more comfortable and more likely to enroll in a study.

