 |
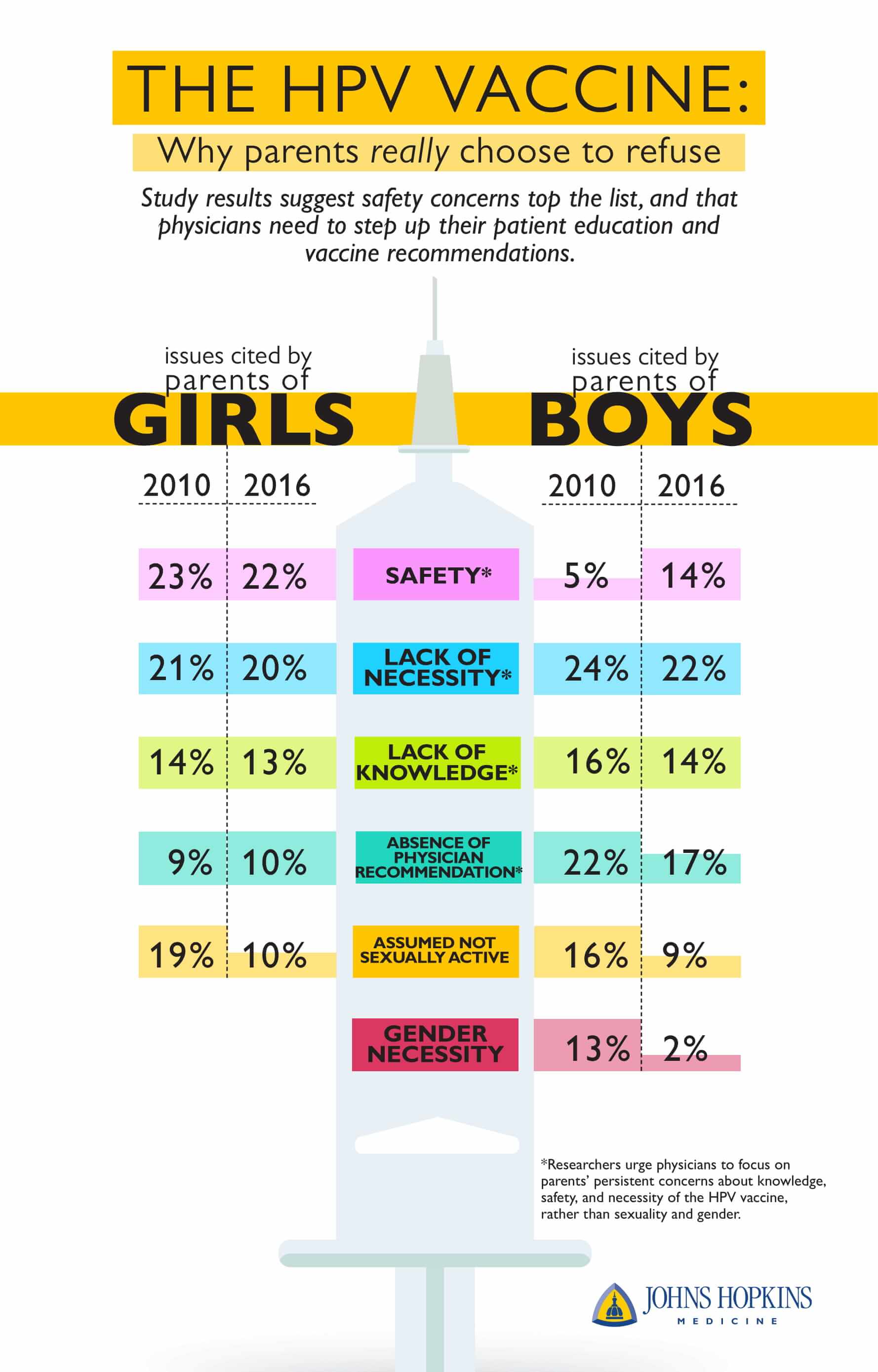
Top reasons why parents choose to refuse the HPV vaccine for their children |
The findings, published in the November issue of the Journal of Adolescent Health, could help public health officials and professional societies develop new interventions to increase rates of HPV vaccination.
The HPV vaccine has already shown promise in helping to stem long-rising rates of cancers transmitted by the virus, including an estimated 31,500 cases in the United States annually of cancers of the cervix, vagina, vulva, oropharynx and anus. The U.S. Food and Drug Administration approved the vaccine—beginning at age 9—in 2006 for females and in 2009 for males. But it wasn’t recommended for use in males until 2011 by the Advisory Committee on Immunization Practices, the group of medical experts that gives guidance on vaccines for the public. Worldwide studies have shown the vaccine to be virtually 100 percent effective and very safe, with the FDA concluding that the vast majority of side effects are minor, and that benefits continue to outweigh adverse events.
Despite recommendation by ACIP to include the vaccine as part of the routine childhood vaccination series, current use of the vaccine in the U.S. remains relatively low. In 2016, the most recent year for which data on vaccination rates are available, only 50 percent of eligible females and 38 percent of eligible males had completed the vaccine series.
“We wanted to better understand why parents choose not to vaccinate their children against HPV, since that information is critical for developing improved public health campaigns and provider messages to increase vaccination rates,” says study author Anne Rositch, M.S.P.H., Ph.D., assistant professor in the Department of Epidemiology at Johns Hopkins Bloomberg School of Public Health. She holds a joint appointment in oncology at the Johns Hopkins Sidney Kimmel Comprehensive Cancer Center.
For the study, the researchers mined data from the 2010–2016 National Immunization Survey-Teen (NIS-Teen), a series of annual vaccine monitoring surveys conducted by the U.S. Centers for Disease Control and Prevention. NIS-Teen collects information from a nationally representative sample of parents about their children’s vaccine usage, with vaccine rates verified with information collected from each child’s physician.
During those years, the survey included questions about whether parents planned to vaccinate their children against HPV if they hadn’t already—and, if not, why they were choosing not to. The research team analyzed responses to that specific question, which was asked each year from 2010-2016. In 2010, there were responses from 3,068 parents of girls and 7,236 parents of boys age 13-17. In 2016 there were responses from 1,633 parents of girls and 2,255 parents of boys age 13-17. The question was open-ended, allowing parents to name their reasons rather than choosing from a list.
Rositch and her colleagues, including Anna Beavis, M.D., M.P.H., and Kimberly Levinson, M.D., M.P.H., both assistant professors in the Department of Gynecology and Obstetrics at the Johns Hopkins University School of Medicine; and Melinda Krakow, M.P.H., Ph.D., a former master’s of public health student at the Johns Hopkins Bloomberg School of Public Health, sorted the answers into “reason” categories, separating the data by year and by children’s gender.
They found that for girls, the top four reasons parents gave for not vaccinating stayed relatively stable between 2010 and 2016. These included safety concerns (cited by 23 percent of non-vaccinating parents in 2010 versus 22 percent in 2016), lack of necessity (21 percent versus 20 percent), knowledge (14 percent versus 13 percent) and physician recommendation (9 percent versus 10 percent). Those citing their child’s lack of sexual activity shrank by nearly half over these years (19 percent versus 10 percent).
For boys, the top reasons cited by parents for not vaccinating in 2010 all decreased over time. These included lack of necessity (24 percent versus 22 percent), physician recommendation (22 percent versus 17 percent), knowledge (16 percent versus 14 percent), child’s lack of sexual activity (16 percent versus 9 percent) and gender (13 percent versus 2 percent). Notably, however, concerns about safety increased from 5 percent in 2010 to 14 percent in 2016. The researchers are not sure why that is, but do note that less than 1 percent of parents of males from 2010 to 2016 reported anti-vaccination concerns as a reason to not vaccinate their child. The researchers say it’s unlikely these safety concerns are attributed to exposure to false anti-vaccination information.
Beavis says that their findings demonstrate that parents are less concerned with the HPV vaccine’s relation to gender and sexual activity, and that public health campaigns should focus on persistent concerns about safety and necessity of the vaccine for both boys and girls in order to be responsive to parents’ true concerns. She suggests that doctors who commonly administer the HPV vaccine, including family practice physicians, obstetricians/gynecologists and pediatricians, should focus on the fact that the HPV vaccine has enormous potential to prevent cancers and has a strong safety profile from over a decade of vaccine administration.
These physicians may also be more likely to broach the subject with parents, and recommend the vaccine, if they themselves better understand that relatively few parents avoid vaccinating due to concerns over sexual activity.
“We think all physicians need to be champions of this vaccine that has the potential to prevent tens of thousands of cases of cancers each year,” Beavis says. “Providing a strong recommendation is a powerful way to improve vaccination rates.”
Up to 80 percent of sexually active Americans will be infected with HPV at some point during their lives, according to the American Sexual Health Association. The majority of these infections resolve without symptoms. However, HPV is sexually transmitted and can cause genital warts and benign tumors on the aerodigestive tract, a condition called laryngeal papillomatosis. Additionally, certain strains can cause changes in DNA that encourage the formation of cancers in both males and females.
HPV can be transmitted by other means than sexual intercourse. The Guttmacher Institute, which conducts independent research on sexual activity, sexually transmitted diseases and reproductive health, reports that an estimated 50 percent of teens ages 15 to 19 have oral sex with an opposite sex partner and 1 in 10 has anal sex with an opposite sex partner.
The HPV vaccine can protect against nine cancer-causing strains of HPV. The recommended dosing schedule for the vaccine now involves two injections if the first is administered before age 15, or three injections if the first is administered after age 15.
