Teen’s Mysterious Condition Leads to Opening of New Johns Hopkins Children’s Center Clinic
10/07/2021
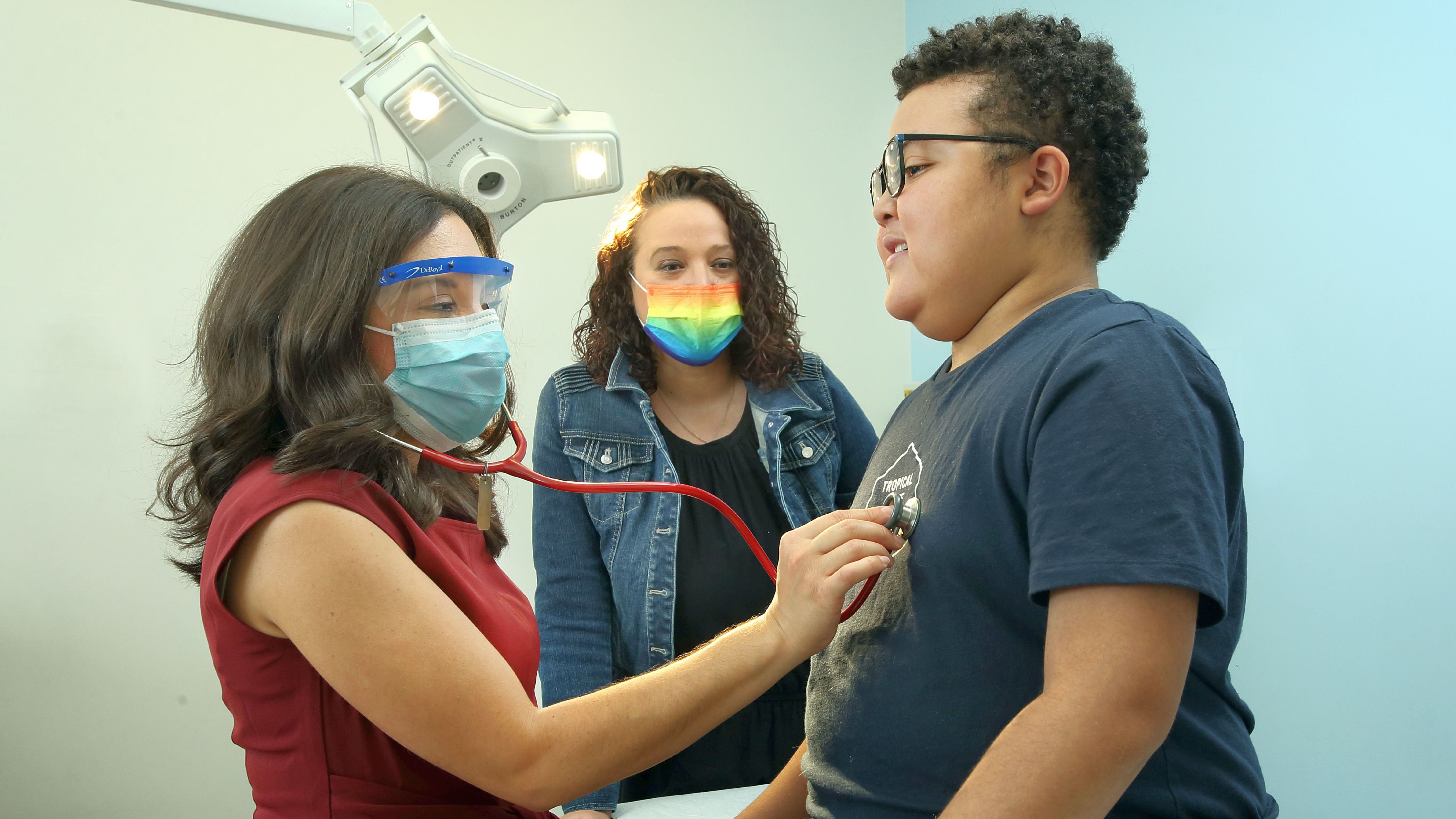
Thirteen-year-old Gregory Rhoden’s condition has been a mystery his entire life. He was born prematurely and his lungs seemed underdeveloped. While he had some respiratory issues growing up, it wasn’t until a running event in kindergarten that he began complaining of chest pain and shortness of breath. A doctor labeled Gregory’s symptoms as asthma and allergies, and referred him to an allergist.
In the fifth grade, the boy’s condition worsened. His mother, Katja Fort Rhoden, says Gregory started coughing up “yucky sputum.” She took him to the emergency department at Johns Hopkins Children’s Center (JHCC), where he was diagnosed with a chest infection.
“It looked like it was walking pneumonia, but his pulmonary function tests [PFTs] were really abnormal — even for a kid with pneumonia,” recalls Fort Rhoden. To shed some light on the mystery, Gregory was referred to JHCC pediatric pulmonologist Christy Sadreameli, M.D., M.H.S., who also is an assistant professor of pediatrics at the Johns Hopkins University School of Medicine.
After reviewing Gregory’s abnormal PFTs, Sadreameli ordered a CT scan of his lungs. The images revealed unusual findings including emphysema. His mother had a history of chronic variable immune deficiency, an immune system disorder that increases the risk of infections, particularly in the respiratory system. Fort Rhoden’s lung disease had eventually worsened to the point that she needed a double lung transplant.
It was Gregory’s mysterious condition that spurred Sadreameli to begin forming the Childhood Interstitial Lung Disease Clinic (chILD) at Johns Hopkins with a team from JHCC’s neonatology and pulmonology departments to better understand and more successfully treat rare pediatric respiratory diseases.
Sadreameli knew that mother and son shared a similar lung disease, but what was it?
Gregory underwent testing for many known lung disorders including cystic fibrosis, as well as screening for a genetic or an autoimmune cause of his condition.
“I knew that what we were dealing with something that was extremely rare — a lung disease that had not yet been fully documented in the literature,” Sadreameli says.
The genetic workup revealed that Fort Rhoden and her son had the same mutation on the platelet-derived growth factor receptor alpha (PDGFRA) gene. This gene was known to be crucial for lung development, but mutations in the gene had not been linked with any known lung diseases in humans.
With this clue, Sadreameli spoke with her multidisciplinary team members at Johns Hopkins and contacted experts beyond the institution, who agreed that she had a compelling hypothesis — the PDGFRA mutation could explain the lung disease that Fort Rhoden and her son shared.
Sadreameli calls Gregory’s condition a diffuse lung disease of unknown etiology.
“Gregory also has emphysema and a bleeding disorder [pulmonary capillaritis] in his lungs,” she says. “It is uncommon to have both at the same time, and his mom has a very similar disorder.”
She adds that Gregory and his mother likely have a genetic disease that impacts the lungs and immune system.
“He has taught me much over the years as I cared for him clinically, which has impacted the direction of my research program and my current interests,” Sadreameli says. “I really feel that Gregory is the one-of-a-kind patient that changed things for me.”
Sadreameli has received a grant to study the disease at new chILD clinic that she and her colleagues started to better care for patients like Gregory and other patients with unusual pediatric lung disorders. Johns Hopkins also is part of the national registry —established by the Children’s Interstitial Lung Disease Research Network — which collects data about patients with such disorders that can inform research and treatments.
“It’s a clinical research initiative that could open the door to understanding new ways children can get lung disease,” says Sadreameli. “There may be other children like Gregory in the future, so if we can identify their problems, we could discover other new diseases.”
Sadreameli says Gregory may need to have a lung transplant in the future. “My goal is to make that as long from now as possible, or maybe prevent needing it altogether” she says.
Gregory, a fan of video games, model building and science, is aware that he might need a transplant someday. His mother says “he thinks it’s cool.”
Fort Rhoden says that in spite of his lung disease, Gregory attended space camp when he was younger, and now won’t let anything deter his dream of becoming an astrophysicist.
“His condition is a heavy load to carry, and it has disrupted his teenage years a lot,” she says. “But he’s been remarkable in keeping moving. He’s got a really positive outlook as a kid and takes things in stride.”
Sadreameli, Fort Rhoden and Gregory are available for interviews.
See also: Uncovering an Unknown Lung Disease
