Distinguishing Child Polio-Like Illness from Similar Diseases
12/03/2018
Johns Hopkins researchers have analyzed patient data from 45 cases of what they thought was acute flaccid myelitis (AFM), the polio-like outbreak occurring in U.S. children, and realized that only 75 percent of diagnosed cases were AFM.
The researchers say they hope that clearer diagnostic criteria identified in their study, published Nov. 30 in JAMA Pediatrics, will help patients receive the right treatment for their diagnosis.
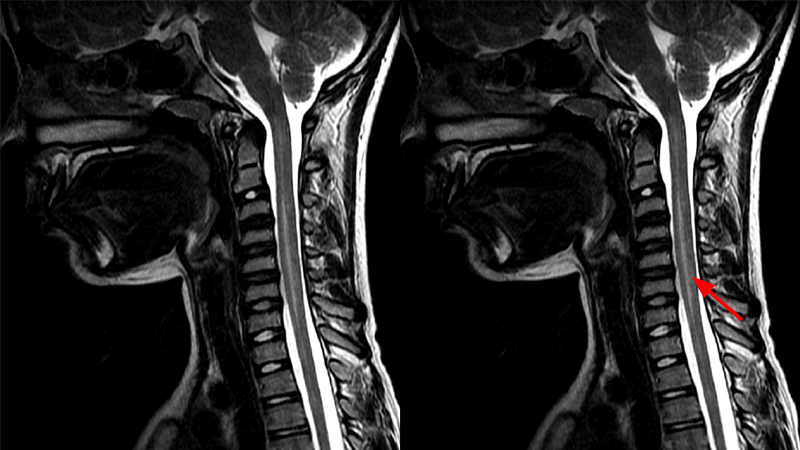
The Centers for Disease Control and Prevention defines AFM as weakness in one or more arms or legs as well as damage to the gray matter of the spinal cord as detected by MRI. But, the researchers thought that other illnesses that affect the spinal cord and nervous system were getting lumped in with the AFM cases.Lead author and clinical fellow, Matthew Elrick, M.D., Ph.D., and his neurologist colleagues reviewed the medical records and available MRIs of patients and categorized the children as definitively having AFM or having a potential alternative diagnosis. The researchers then compared the characteristics of the definitive cases with the potential alternative diagnoses.
Those patients with definitive AFM had a fever or viral infection before the onset of weakness in the arms or legs. They also lost function of their limbs in one side of the body first, with the majority of children losing function of a single limb or all four eventually. The children with definitive AFM also had many white blood cells in their spinal cords and less protein in their cerebral spinal fluid than the children with alternative diagnoses. Unlike those cases with alternative diagnoses, the children with AFM only had damage in the spinal cord’s gray matter—where the bodies of the nerve cells reside—and not in the brain or the spinal cord’s white matter—where the connections between nerve cells that send messages back and forth reside. Children with AFM respond better with infusions of immunoglobins—a collect of antibodies that can help tag pathogens as invaders so the immune system can eliminate them.
The most common alternative diagnoses were transverse myelitis—an inflammation of the spinal cord—and spinal cord stroke. Other diagnoses included demyelinating syndromes, Guillain-Barre syndrome, Chiari I myelopathy and meningitis. Immune suppressants are ideal for reducing spinal cord inflammation in diseases such as transverse myelitis, but could be detrimental to patients with AFM.
