Activating 'Inflammasome' May Improve Cancer’s Response To Immunotherapy And Parp Inhibitors
10/27/2020
The inflammasome — a protein signaling network that is activated to rid the body of virus or bacteria-infected cells — may play an important role in triggering an immune response to cancer and causing an existing class of drugs to work better against cancers.
A collaborative research study led by experts at the Johns Hopkins Kimmel Cancer Center and University of Maryland Marlene and Stewart Greenebaum Cancer Center, supported by Stand Up To Cancer and the Adelson Medical Research Foundation, found that the inflammasome imparts a DNA repair defect-like state in cancer cells. In laboratory and animal models of ovarian and breast cancer cells, it induced an immune activating signal that directly made the cells susceptible to treatment with drugs called PARP inhibitors, drugs that disable the cancer cell’s ability to repair DNA damage caused by anticancer therapies. As a result, the cancer cell dies.
The findings published online May 26 in the Proceedings of the National Academy of Sciences, appear to apply across multiple tumor types and create the potential for a wider use of PARP inhibitors.
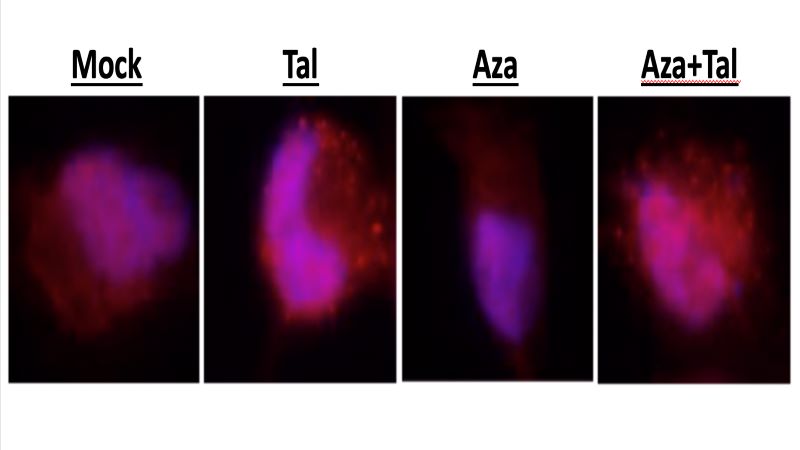
In laboratory models, the researchers used the epigenetic drug 5-azacytidine to induce transcriptional BRCAness in two-thirds and one-third of ovarian and triple negative breast cancer cell lines tested. These BRCAness data were correlated with inflammasome activation in two cell lines, which demonstrated the most marked induction of BRCAness, explains Michael Topper, Ph.D., co-corresponding author on the study, Evelyn Grollman Glick Scholar and instructor in oncology at the Johns Hopkins Kimmel Cancer Center. Epigenetics refers to chemical alterations to the DNA of cells that can change gene behavior without mutating the DNA. The drug 5-azacityidine is classified as a demethylating agent because it blocks a chemical process known as DNA methylation and can restore function to some cancer suppressor genes. Ongoing research also studies the ability of this drug, and other epigenetic drugs, to prime cancer cells for a better response to immunotherapies.
We believe we have uncovered a novel relationship in which the drug not only primes the immune response but also causes the breast and ovarian cancer cells to act as if they have a BRCA mutation. We think this reveals a new mechanism that has not previously been linked to immune therapy response,” says Topper.
Turning the inflammasome on with epigenetic therapy, makes cancer cells targets of the immune system and responsive to drugs known as PARP inhibitors, the researchers say. “Specifically, it makes tumor cells that do not have BRCA mutations act like they do,” says Feyruz Rassool, Ph.D., the senior corresponding author, professor of radiation oncology and co-director of Experimental Therapeutics Program at the University of Maryland Marlene and Stewart Greenebaum Cancer Center.
BRCA mutations alter the body’s ability to repair DNA, putting those affected at higher risk of developing breast, ovarian, pancreas and other cancers. However, cancers—particularly breast and ovarian cancers—that contain BRCA mutations often respond to treatment with PARP inhibitors, which disable the cancer cell’s ability to repair damage caused by anticancer drugs and radiation therapy.
“This mutation is present in only a small percentage of patients with breast and ovarian cancers, and this is the only setting where PARP inhibitors have demonstrable clinical efficacy,” says co-author Stephen Baylin, M.D., Virginia and D.K. Ludwig Professor for Cancer Research.
Using 5-azacytidine to make cancer cells, which do not have BRCA mutations act like they have the mutations—a situation the researchers refer to as “BRCAness”—sensitizes cancer cells to treatment with PARP inhibitors and may expand the benefit of the drug to more patients.
“The relationships between the inflammasome in the tumor cells and diminished ability of the cells to repair DNA damage may apply to multiple common tumor types,” says Baylin. In data obtained from The Cancer Genome Atlas, Topper showed the possibility that activating the inflammasome with 5-azacytidine could produce “BRCAness” in many common tumor types. Treating with drugs like 5-azacytidine could extend treatment to patients with a broad range of cancers. A clinical trial combining an inhibitor of DNA methylation and a PARP inhibitor in patients with breast cancers, which do not have BRCA mutations, has begun through Stand up to Cancer.
The researchers also explain that a pathway called STING (stimulator of interferon genes) is a key regulator of the inflammasome. STING, shown to convert cold tumors, or tumors that do not attract the attention of the immune system, into hot tumors, ones that are most likely to respond to immunotherapies. STING causes CD8+ T cells to traffic to tumors and, in animal models, made breast cancer cells more responsive to immune checkpoint inhibitors.
In a surprising twist, the work of the investigators could potentially shed light on a severe and deadly inflammatory process, called cytokine storm syndrome (CSS), occurring in SARS-CoV-2 infection, the researchers say. They hypothesize that overactivation of the inflammasome may be a key regulator of CSS, the most severe complication of COVID-19 infection. Topper, Rassool and Baylin are collaborating with an international consortium called COV-IRT (COVID-19 International Research Team), aimed at using an open science model to rapidly advance COVID-19 research and therapies. They hope to use their inflammasome discovery to study and develop a serum test to predict early which patients will develop the most severe COVID-19 infections and to look for existing drugs that could inhibit the inflammasome and stop CSS.
In addition to Topper, Rassool and Baylin, other investigators participating in the research included Lena McLaughlin, Lora Stojanovic, Aksinija Kogan, Julia Rutherford, Eun Yong Choi, Ying Zou and Rena Lapidus, from University of Maryland, and Ray-Whay Chiu Yen, and Limin Xia from the Johns Hopkins Kimmel Cancer Center.
The research was funded by the Van Andel Institute–Stand up to Cancer, the Adelson Medical Research Foundation, Evelyn Grollman Glick Scholar, The Hodson Trust, the Leukemia Lymphoma Society, the Maryland Cigarette Restitution Fund Program, the National Cancer Institute–Cancer Center Support Grant P30 CA134274 University of Maryland Marlene and Stewart Greenebaum Comprehensive Cancer Center, the Molecular Medicine Graduate Program, University of Maryland, the Biochemistry Graduate Program, University of Maryland and the Human Genetics Graduate Program, University of Maryland, the Commonwealth Foundation, the Defense Health Program through the Department of Defense Ovarian Cancer Research Program, and Teal Innovator Award OC130454/W81XWH-14-1-0385.
