Research Story Tip: Lyme Disease Bacteria Alter Immune System and May Cause It to Attack Healthy Cells
12/08/2020
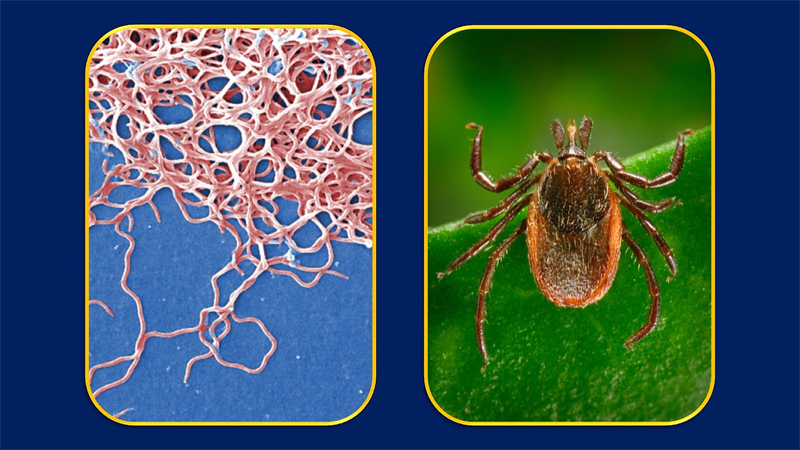
With the incidence of Lyme disease rising to over 300,000 new U.S. cases annually, more people are suffering with the debilitating and persistent symptoms associated with what clinicians call post-treatment Lyme disease syndrome. Now, researchers at the Johns Hopkins Lyme Disease Research Center have found that the bacterium behind the disease, , causes significant changes in how the human body responds to its presence.
In a recent study, the researchers showed that Borrelia burgdorferi alters dendritic cells, which normally present antigens — proteins from pathogens such as bacteria and viruses — to immune system T-cells, signaling an immune response against the foreign invaders. However, Borrelia burgdorferi stops this communication, which may then lead to the immune system mistakenly attacking healthy cells.
A report on the findings were published in the September 2020 issue of Frontiers in Medicine.
“We believe these observations are relevant not only to how Borrelia burgdorferi disrupts the immune system but other infections as well,” says senior author Mark Soloski, Ph.D., co-director for basic research at the Johns Hopkins Lyme Disease Clinical Research Center, and professor of medicine at the Johns Hopkins University School of Medicine. “Antibodies that react with a person’s own tissues or organs have been reported in patients with infections, including COVID-19.”
In an attempt to better understand how a Lyme disease infection contributes to weakening the immune system, the Johns Hopkins Medicine researchers isolated dendritic cells from healthy study participants and exposed them to Borrelia burgdorferi. They found that bacterial infection causes receptor sites on the surface of dendritic cells, known as HLA-DRs, to mature and become active. HLA-DRs normally present antigens to killer T-cells, the immune system agents that remove invaders from the body.
However, the researchers believe that when the HLA-DRs interact with Borrelia burgdorferi, they are structurally changed and keep the dendritic cells from “marking” the bacterial proteins as foreign. As a result, the dendritic cells attract T-cells but in response to healthy cells in the area rather than the Lyme disease microbes.
The researchers further surmise that if a person has a genetic predisposition to autoimmune diseases such as lupus or rheumatoid arthritis, infection by Borrelia burgdorferi may trigger their development.
Future research on HLA-DR and dendritic cell response to Borrelia burgdorferi, the researchers say, could contribute to new treatments for Lyme disease and a better understanding of how autoimmune diseases may arise.
Soloski is available for interviews.