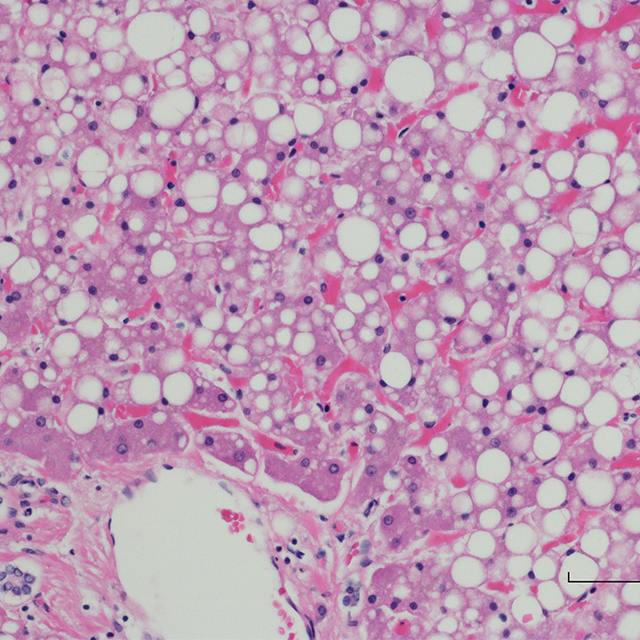
It is no secret that alcohol use disorder is often deeply stigmatizing. But this stigma doesn’t just affect patients’ mental health, says Johns Hopkins hepatologist Po-Hung “Victor” Chen — for some patients, it can be a matter of life and death. For decades, hospitals around the world that provide liver transplants for alcohol-associated liver disease required patients to abstain from drinking for at least six months prior to the procedure. However, Chen says, many patients won’t survive six months without this rescue surgery.
Originally, the six-month requirement for alcohol abstinence “was intended to help patients recover so that some may not need a transplant at all, [but] many in the medical community believed that patients’ ability to abstain was a surrogate for their likelihood to return to drinking after transplant,” he adds. “Patients [have] had to prove themselves worthy of this surgery. We’re working [to dispel] that stigma.”
Over the past decade, studies from Europe and the U.S. have shown that about a third of patients return to drinking after their liver transplants, whether they have abstained from drinking six months prior or not. In addition, earlier research by Chen and his colleagues showed that whether patients had abstained from drinking or not had no effect on patients’ post-transplant outcomes. Based partly on this body of research, Johns Hopkins is one of the few hospitals in the U.S. that regularly offer early liver transplants (ELT), waiving the six-month abstinence requirement for some patients after holistic psychosocial assessments.
While selected patients have been able to access this lifesaving surgery, little was known about their experiences before and after their transplants — information that could help Johns Hopkins and other hospitals provide better care.
A Study on Patient Experience Following Early Liver Transplant
Chen and colleagues recently published a qualitative study examining the experiences of 20 patients who received ELT at Johns Hopkins. The researchers recruited patients who had their transplant surgeries between October 2012 and September 2020. Each of these patients was interviewed about their overall experiences related to challenges after the transplant; relationships with family, friends, or other supportive people before and after the operation; experiences with alcohol use; and self-perceptions and stigma.
Several themes emerged. For example, prior to the procedure, many of these patients described alcohol as being a constant part of life, negatively affecting personal relationships and their careers, and feeling stuck in the cycle of drinking. The study participants often expressed a rapid decline in their health as their disease worsened and their livers decompensated.
Experiences diverged substantially after ELT. While some study participants experienced continued stigma or shame, others felt a new sense of self-worth. Some struggled with their relationships, particularly with family members who continued to drink while patients remained sober, but others successfully reestablished relationships that had faded. Although some patients struggled to find work after their transplants, others thrived professionally.
Chen notes that he and his colleagues who treat patients with alcohol-associated liver disease work closely with addiction medicine specialists, who are running a clinical trial to understand the best interventions to maintain alcohol abstinence after ELT. Additionally, their qualitative study suggests that a more holistic approach to meeting patients’ mental health and social needs could help them stay healthier and navigate their complex psychosocial challenges post-transplant. In the meantime, the team continues to evaluate patients on a case-by-case basis to identify those who would most benefit from ELT.
“Having had some alcohol recently is not a reason [by itself] to disqualify these patients from a lifesaving transplant,” he says.
To refer a patient, call the Johns Hopkins Comprehensive Transplant Center at 410-614-2989 or the Division of Gastroenterology and Hepatology at 410-933-7495 (Maryland) or 202-660-5555 (District of Columbia).