Researchers Probe the New Frontier of Immune Therapy
Johns Hopkins All Children’s Hospital researchers have identified an important gene function with potential for enhancing the immune system.

Masanobu Komatsu, Ph.D.
Our complicated immune system holds many secrets and scientists have been engaged in laboratory detective work for decades seeking not only a better understanding of immunity, but also looking for ways to enhance it.
One of the newest and most promising treatments for cancer and several other serious diseases is to enhance “adaptive immunity,” an immune system enhancement strategy aimed at putting the immune system into “overdrive” so that it can get to work faster and more efficiently in its fight against diseases.
Masanobu Komatsu, Ph.D., a senior scientist in the Johns Hopkins All Children’s Department of Surgery and the Cancer & Blood Disorders Institute, and his colleagues, have been working to gain a better understanding of aspects of the immune system. Their efforts are paying off, as explained in their recent study published in The American Journal of Pathology (Vol. 191 No. 2).
“Our study has provided us with a better understanding of the molecular mechanism by which the immune system responds to pathogens, the organisms that cause disease, and how the immune system develops a defense against pathogens by recruiting disease-fighting white blood cells, called ‘lymphocytes’ to the lymph nodes from blood circulation,” explains Komatsu, who came to Johns Hopkins All Children’s in 2018.
According to Komatsu, lymphocytes are “recruited” by special blood vessels called high endothelial venules, or HEVs. HEVs transport lymphocytes to the body’s lymph nodes, which, Komatsu says, are like “screening and training centers” for lymphocytes. It is where antigens of invading pathogens are presented to lymphocytes and where lymphocytes “muscle up” to fight the pathogens. Think of the lymphocytes as police dogs being exposed to the smell of a criminal’s clothes before chasing him or her down.
Because lymphocytes reactive to a certain pathogen exist at very low levels in circulating blood, lymphocyte recruitment needs a “jump start” to activate immune system efficiency. Finding ways to help speed up lymphocyte recruitment is an important research goal.
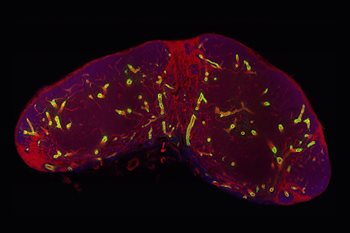
The R-Ras Gene
“For the past 10 years, my lab has been investigating the R-Ras gene and its role in blood vessels,” says Komatsu, who earned his Ph.D. in molecular cell and developmental biology from the University of Miami School of Medicine in 1998. “This research is timely because there is increasing interest in the function of HEVs and how they get lymphocytes to the lymph nodes and to cancerous tissue and chronic inflammation.”
According to Komatsu, the R-Ras gene is triggered by a cytokine (a small protein important in cell signaling) called tumor necrosis factor (TNF). TNF is a substance in the body that not only causes inflammation, but also has many other roles in cell life, such as cell survival, proliferation, differentiation and death. TNF also plays an important role in activating blood vessels to facilitate lymphocyte recruitment.
However, recruiting lymphocytes is just part of the immune process. Further research into how well, and how quickly the immune system can get lymphocytes to the disease site, is a big part of Komatsu’s research.
The most recent published study conducted by Komatsu and his colleagues focuses on the R-Ras gene’s role in quickly adapting the function of HEVs to increase lymphocyte transportation to the lymph nodes upon pathogen infection. Junko Sawada, D.V.M., Ph.D., of the Komatsu Lab is the lead author on the paper and is an instructor of orthopaedic surgery with Johns Hopkins University.
 Junko Sawada, D.V.M., Ph.D.
Junko Sawada, D.V.M., Ph.D.The research team knew that one way to find out just how important R-Ras is to immunity could be discovered by observing what happened with the immune response when the R-Ras gene was missing. Using animal models, the researchers “knocked-out” the R-Ras gene and found that without it both lymphocyte recruitment and immunity development were deficient. They also found that R-Ras heightens the HEV function to accelerate lymphocyte recruitment to the lymph nodes for screening many lymphocytes as quickly as possible.
The Role of Lymph Node Blood Vessels
“Rapid expansion of lymphocyte defense depends on HEVs to functionally adapt for a faster influx of lymphocytes into the lymph nodes,” Komatsu explains. “Our study has helped us to better understand the molecular mechanism of this critical adaptation.”
Interestingly, although HEVs are specialized blood vessels in lymph nodes, these blood vessels sometimes form in malignant tumors and deploy a lot of lymphocytes there. Indeed, recent studies by Komatsu’s group and others suggest that the presence of HEVs in tumors are critical for cancer immunotherapies.
Accordingly, the next step in their research is to modulate R-Ras gene expression to facilitate HEV formation in tumors. The goal now is to find a way to generate many HEVs in tumors for effectively recruiting lymphocytes that fight cancer cells. Boosting the immune response against cancer using the R-Ras gene may be accomplished through a drug or a unique gene therapy.
Another aspect of Komatsu’s research is investigating ways to use the vascular system for drug delivery and that research interest may play a future role in improving the immune response when even more research on the R-Ras has been completed.
Immunity and Us
The results of this study opened windows of opportunity for enhancing immune function that may be useful for treating a great number of diseases. “Our study has provided us with a greater understanding of how blood vessels in our body respond to immune reactions to support the fight against cancer and infectious diseases,” Komatsu says.
Finding ways to develop immunity to a pathogen as quickly as possible has become more important for all of us since the emergence of COVID-19. The researchers reflected on how the COVID-19 pandemic has raised global awareness about the important need for immunity against new pathogens. However, meeting the challenges raised by emerging diseases requires better knowledge about how the immune system works and how we might be able to enhance its efficiency for a unique, “moving target.” This reality makes their future work more important than ever.
“Better knowledge about immunity is important for the survival of humankind, and our study provides new insight into the development of immunity. This finding has broad implications for many life-threatening medical conditions,” Komatsu concludes.
